
Subscribe
eNewsletter

Ready to get certified?
Free CDCES Coach App
Download
Free Med Pocket Cards

JR is a 15-year-old admitted to the hospital with DKA for the second time this month. JR says they are tired of their parents always telling them how to manage their diabetes. They just stopped wearing their continuous glucose monitor and tell you they “take insulin when they feel like it”.
What best describes what this teenager is experiencing?
Click Here to Test your Knowledge

This presentation will include the latest information on Social Determinants of health, assessment strategies, and approaches. We will explore the psychosocial issues that can discourage individuals from adopting healthier behaviors and provides strategies to identify and overcome these barriers. Life studies are used to apply theory to real-life situations. A great course for anyone in the field of diabetes education or for those looking for a new perspective on assessment and coping strategies.
Objectives:
Intended Audience: A great course for healthcare professionals in the field of diabetes education looking for a straightforward explanation of identification and treatment of hyperglycemic crises.
Instructor: Beverly Thomassian RN, MPH, CDCES, BC-ADM is a working educator and a nationally recognized diabetes expert.
All hours earned count toward your CDCES Accreditation Information
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.

We quizzed test takers on diabetes and sexual health. 73% of respondents, chose the best answer. Since we are addressing diabetes distress in our December newsletter, we thought this would be the right time to explore this topic in more depth. As we all know, sexual health and well being are interrelated. We want to share this important info on discussing sexual well being, so you can pass it on to people living with diabetes and your colleagues.
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer below: Answer Question
Question: JR is a 33-year-old who is non-binary and was recently diagnosed with type 2 diabetes. During your assessment, JR asks if diabetes can affect their sexual health.
What is the best response?
Answer Choices:
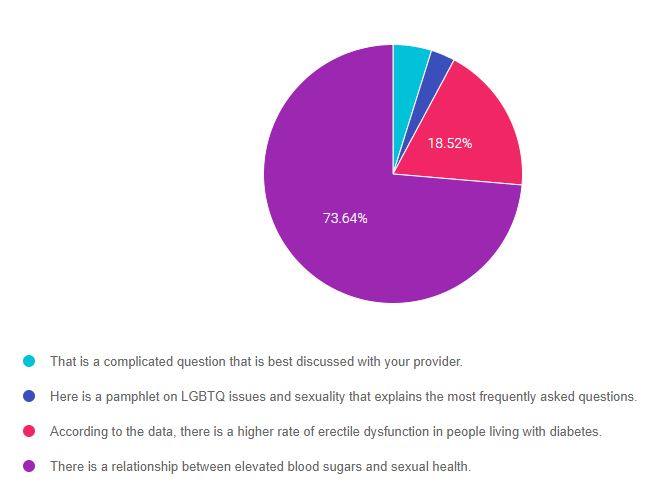
As shown above, the most common choice was option 4, the second most common answer was option 3, then option 1, and finally option 2.
If you are thinking about taking the certification exam, providing person-centered care is at the heart of the exam. Being familiar with diabetes care across the lifespan and for diverse populations is also really important. This practice test question will set you up for success. Test writers anticipate possible answers based on the details in the question. They will wave those “juicy answers” that seem so familiar to you, right under your nose. Your job is to weed through the to choose the BEST answer based on the person’s characteristics.
In this Question of the week, we are working with JR who identifies as non-binary. Let’s take a moment and address how this might impact our approach to care.
First, since JR let’s us know that they are non-binary, what does that mean?
Nonbinary describes someone whose gender doesn’t fit within the gender binary of a man or a woman. “Nonbinary” is an umbrella term that expresses a wide range of gender identities; other terms someone may use to describe themselves is genderqueer or gender non-conforming, among others. It is important to check in with each person and ask them how they identify. One way of doing this is to introduce yourself, along with your pronouns, and then ask what pronouns the other person uses, as in the example below.
“Hello, my name is Beverly and I go by ‘she, her’ pronouns. What pronouns do you use?”
or
“How would you like me to refer to you?”
By paying careful attention to each person’s experience from the moment they walk in the door until we say goodbye, we can find ways to create a more inclusive environment. This awareness of the details, such as inclusive gender questions on intake forms or gender-neutral signage on the bathrooms, are great first steps to show your care and respect for those you work with.
Next, what do we know about providing care to members of the lesbian, gay, bisexual, transgender, and queer (LGBTQ+) community with diabetes?
Studies have shown that those who are LGBTQ+ are subject to unique health disparities and worse health outcomes than their heterosexual counterparts, which has clinical relevance in the delivery of diabetes care and education. Diabetes care and education specialists are in a pivotal position to advocate for this medically underserved and vulnerable population, to make sure they get the best possible care.
Lastly, JR wants to know how diabetes will affect their sexual health.
At this juncture, we may provide a general overview of how elevated blood sugars can affect blood vessel health and cause nerve damage, that may impact their sexual function over time (such as difficulty feeling pleasure or achieving an orgasm). Then we might ask if they have any particular questions. Our willingness to explore this sensitive topic free of judgment will be very meaningful. And, it’s okay if this feels new and uncomfortable.
“We all have our own personal experiences and internalized biases which impact the care we deliver. Our job is to practice cultural humility by checking in with our biases so they do not interfere with helping someone find a path to thriving with diabetes. It can feel uncomfortable at first, but as we take the time to expand our knowledge about others, it will feel more comfortable”
And just know, it takes time to get up to speed. I’d encourage readers to check out the ADCES handout below and watch this funny video clip that a colleague sent me, “What “The Sex Talk” Looks Like Now, by Alternatino. This video made me crack up and appreciate the nuance of all the terms. Thanks so much, for your willingness to consider this topic. I truly hope you find it helpful in improving in delivery of care.
Answer 1 is incorrect. 4.82% chose this answer, “That is a complicated question that is best discussed with your provider.” Even though sexual health may not be our area of expertise, we can certainly provide a general answer and explore their particular questions. Of course, if a question is beyond our knowledge, referring back to the provider would be best.
Answer 2 is incorrect. 3.01% of you chose this answer, “Here is a pamphlet on LGBTQ+ issues and sexuality that explains the most frequently asked questions.” This is not the best answer, because it doesn’t address the question the person is asking. JR wants to know how diabetes can affect their sexual health, not the relationship between LGBTQ+ and sexuality.
Answer 3 is incorrect. 18.52% of respondents chose this answer, “According to the data, there is a higher rate of erectile dysfunction in people living with diabetes.” It is true that up to 50% of men with diabetes experience erectile dysfunction. However, we are not sure of JR’s sex assigned at birth, so this answer may not apply to JR. Instead, we could provide a general overview of how elevated blood sugars can affect blood vessel health and cause nerve damage, that may impact their sexual function over time (such as difficulty feeling pleasure or achieving an orgasm).
Finally, Answer 4 is correct. 73.64% chose this answer, “There is a relationship between elevated blood sugars and sexual health.” YES. This is the BEST answer. And, we might then ask if they have any particular questions.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this important learning activity!
ADCES Inclusive Care for LGBTQ+ People with Diabetes Handout – this handout provides definitions, terms to avoid, and a cultural competency checklist to help you move towards improving inclusivity within your practice.
All Gender Restroom Sign PDF
A Guide To Gender Identity Terms by NPR – A glossary for gender identity terms to use more inclusive language.
Diabetes Prevention and Management for LGBTQ+ People Handout – this handout includes research of diabetes within the LGBTQ+ community, along with clinical considerations, programs, and resources for diabetes educators to use within their practice.
Policies on Lesbian, Gay, Bisexual, Transgender & Queer (LGBTQ+) issues – this resource by the American Medical Association lists all the current healthcare policies in place for the LGBTQ+ community.
Helio’s LGBTQ+ Health Updates Resource Center – this is a “collection of news articles and features that provide the latest information on the unique health needs of individuals in the LGBTQ+ community.”

This presentation will include the latest information on Social Determinants of health, assessment strategies, and approaches. We will explore the psychosocial issues that can discourage individuals from adopting healthier behaviors and provides strategies to identify and overcome these barriers. Life studies are used to apply theory to real-life situations. A great course for anyone in the field of diabetes education or for those looking for a new perspective on assessment and coping strategies.
Objectives:
Intended Audience: A great course for healthcare professionals in the field of diabetes education looking for a straightforward explanation of identification and treatment of hyperglycemic crises.
Instructor: Beverly Thomassian RN, MPH, CDCES, BC-ADM is a working educator and a nationally recognized diabetes expert.
All hours earned count toward your CDCES Accreditation Information
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.

December eNews | Diabetes Distress & Holidays? New Handout with 12 Reframes to Help
Happy December
Greetings to my wonderful health care colleagues. Thank you for all the love and care you have provided this year. I know you touch the lives and hearts of many people who boldly try their best to self-manage their diabetes and I am grateful for you!
As I am sure you have witnessed over time, holidays can amplify stress levels for people living with diabetes. With that in mind, we think this is a perfect time to provide you with some tools to address diabetes distress and burnout during the holidays and in preparation for those New Year resolutions.
Approximately 30% of people with diabetes experience distress at any given time. In addition, many people may be struggling with diabetes burnout.
As health care providers, how do we know if someone is in diabetes distress or is burning out on their self-care?
We might connect with these individuals in a hyperglycemic or hypoglycemic crisis. Maybe they are not showing up for their appointments. These individuals might be mistakenly labeled as “non-adherent” or it may be wrongly assumed that they just don’t care. However, we are compelled to reach out to them and provide a compassionate check-in of their emotional health and state of well-being.
Diabetes specialists help identify and address diabetes distress to improve quality of life and outcomes.
Read more to learn the definition and signs of diabetes distress and burnout and what action to take. Download our FREE Handouts on Surviving the Holidays and Ideas to Deal with Diabetes Distress.
We hope you can join us for our Annual Webinar Updates starting in December. We have over 50 courses to update, so Coach Bev likes to get an early start (see schedule below).
Wishing you health and moments of awe as we move toward 2022.
Coach Beverly, Bryanna, and Jackson
Click here to read our full December 2021 newsletter.
Featured Topics
Upcoming Webinars
Featured Items
You are invited to join Coach Beverly for this FREE Webinar. And, if you want to have access to an additional 220+ sample practice online questions, you can purchase the complete Test Taking Toolkit.
During this webinar, Coach Beverly will help you transform your nervousness into focused energy that will help you succeed. She will provide test-taking tips based on her experience taking the certification exam six times.
This includes a review of 20 sample test questions with test-taking strategies. This does not include access to the recorded webinar or the practice questions.
This includes access to the recorded version of this webinar on your Online University Student Portal. Plus, the Test Taking Toolkit provides you with over 220 sample online practice questions, simulating the exam experience. A perfect way to assess your knowledge and create a focused study plan, while increasing your test-taking confidence.
Don’t worry if you can’t make it live.
Your registration guarantees access to the recorded version.
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.

Our November 30th Question of the week quizzed test takers on Diabetes Distress. 75% of respondents, chose the best answer, which is awesome. Providing person centered care and assessing for diabetes distress are both critically important knowledge points for clinical practice and also for the certification exams.
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer below: Answer Question
Question:
About 30% of people living with type 1 diabetes experience diabetes distress.
Which of the following statements reflects someone struggling with diabetes distress?
Answer Choices:
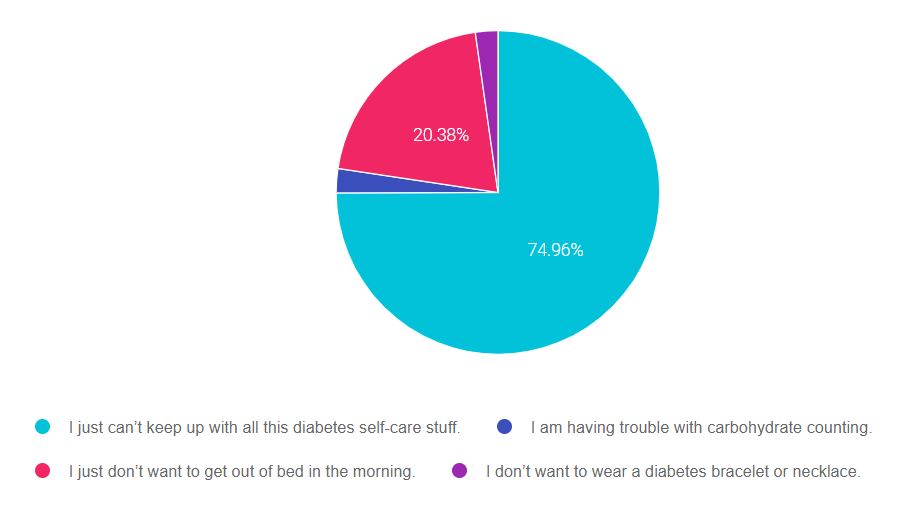
As shown above, the most common choice was option 3, the second most common answer was option 2, then option 4, and finally option 1.
Answer 1 is correct. 74.96% chose this answer, “I just can’t keep up with all this diabetes self-care stuff.” Yes, GREAT JOB. When diabetes self-care all starts feeling like it’s too much or like it’s out of control, that’s when we might say a person is experiencing diabetes distress. Regimen distress is the most common area that people with diabetes come up against. Please see our blog on How to Identify Diabetes Distress and Burnout for information on how to help with diabetes distress.
Answer 2 is incorrect. 2.42% of you chose this answer, “I am having trouble with carbohydrate counting.” This comment indicates a common knowledge gap that can be addressed through providing resources and carb counting information and does not indicate distress.
Answer 3 is incorrect. 20.38% of respondents chose this answer, “I just don’t want to get out of bed in the morning.” If a person with diabetes makes this statement, we would be concerned that they are grappling with more than distress. This comment would prompt us to screen for depression. Please see this link to download the Diabetes Distress Scale and other psychosocial screening tools.
Finally, Answer 4 is incorrect. 2.25% chose this answer, “I don’t want to wear a diabetes bracelet or necklace.” Although we recommend that people taking insulin wear diabetes identification in case of emergency, it is not mandatory and they can chose not to wear one. This comment alone does not indicate diabetes distress.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!
Please see our blog on How to Identify Diabetes Distress and Burnout for more information.
Please see this link to download the Diabetes Distress Scale and other psychosocial screening tools.

This presentation will include the latest information on Social Determinants of health, assessment strategies, and approaches. We will explore the psychosocial issues that can discourage individuals from adopting healthier behaviors and provides strategies to identify and overcome these barriers. Life studies are used to apply theory to real-life situations. A great course for anyone in the field of diabetes education or for those looking for a new perspective on assessment and coping strategies.
Objectives:
Intended Audience: A great course for healthcare professionals in the field of diabetes education looking for a straightforward explanation of identification and treatment of hyperglycemic crises.
Instructor: Beverly Thomassian RN, MPH, CDCES, BC-ADM is a working educator and a nationally recognized diabetes expert.
All hours earned count toward your CDCES Accreditation Information
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.
What is Diabetes Distress?
At some point, almost everyone with diabetes will experience a degree of diabetes distress. It’s expected and completely understandable, especially for those on intensive medication and insulin regimens. Having diabetes is not just about checking blood sugars, counting carbs, taking medications, and giving insulin. People also have an emotional relationship with their diabetes. These feelings around their diabetes can fluctuate throughout their lifetime.
Sometimes a person might have a great day, when their blood sugars on mostly on target, they don’t miss any of their medications and insulin, plus they made it to the gym. But the next day or week or month may feel like a complete mess, with blood sugars all over the place. These blood sugar swings are due to a variety of different reasons, many of which may be out of the person’s control.
Regardless of where a person is with their diabetes self-care, the emotions that bubble up, need to be acknowledged and recognized both by the person with diabetes and the health care provider.
When diabetes self-care all starts feeling like it’s too much or like it’s out of control, that’s when we might say a person is experiencing diabetes distress.
You can determine if a person is experiencing diabetes distress by observing self-care behaviors and asking questions. Or you can use a standardized assessment tool to determine how much distress a person is experiencing in four different areas of diabetes self-care. Please see this link to download the Diabetes Distress Scale and other psychosocial screening tools.
The four areas of Diabetes Distress include:
Emotional Distress – Feeling like they are not doing enough; like they are failing and out of control.
Physician-related distress – Provider doesn’t understand diabetes.
Interpersonal Distress – Friends and family don’t really get it, or are critical, or don’t want to hear about diabetes. Can often be co-associated with depression.
Regimen-related distress – all the daily stuff a person has to do to self-manage their diabetes. Regimen-related distress is the most common kind of diabetes distress, especially for those living with type 1 diabetes.
Health Care Professionals can take an active role in identifying Diabetes Distress
We can start by asking this question, “What is most driving you crazy about your diabetes right now?” or “How are you doing with your diabetes?” while listening carefully to their response and evaluating their degree of distress.
We can also look at self-care behaviors to identify distress:

Sometimes diabetes distress can lead to burnout or be co-associated with burnout. Sometimes, it may be hard to tell the difference. Don’t worry about figuring out if it’s burnout or distress. What’s most important is to recognize that this person is having trouble coping and to provide active listening and help with problem-solving.
What is diabetes burnout?
Diabetes burnout is an emotional reaction that is usually more intense than diabetes distress. A person in the state of burnout is someone with diabetes who has grown tired of managing their condition, then simply ignores it for a period of time.
Sometimes I refer to burnout as taking a diabetes vacation.
This vacation might be a weekend trip, a week trip, or a long-term sabbatical. Diabetes burnout looks different for everyone. Diabetes burnout is a normal reaction to living with diabetes. I am not saying it is a good thing, or we want people to feel burned out. We want to recognize that managing diabetes is a lot of work and sometimes people just take breaks from diabetes self-management.
As health care providers, we can support people experiencing diabetes distress or burnout. According to Mark Heyman, PhD, CDCES, here is an approach he has found helpful.
As health care professionals, we need to check in with people about their distress on a regular basis and provide support.
We need to reassure them that management of diabetes isn’t easy, but they are not alone. There are lots of other people with diabetes experiencing the same feelings.
We might say something like, “Managing diabetes is hard work, but we believe in your ability to make small changes to get to a safer place. You don’t have to move mountains; you just need to take a baby step.“
Let’s remind them, that having diabetes is like getting a job you didn’t ask for. You have to do the work of a body organ, a pancreas. that requires 24 hours a day of attention, without any pay or vacations. Sincerely focus on their successes, no matter how small, and reinforce our belief in their ability to move forward. We got this.

This presentation will include the latest information on Social Determinants of health, assessment strategies, and approaches. We will explore the psychosocial issues that can discourage individuals from adopting healthier behaviors and provides strategies to identify and overcome these barriers. Life studies are used to apply theory to real-life situations. A great course for anyone in the field of diabetes education or for those looking for a new perspective on assessment and coping strategies.
Objectives:
Intended Audience: A great course for healthcare professionals in the field of diabetes education looking for a straightforward explanation of identification and treatment of hyperglycemic crises.
Instructor: Beverly Thomassian RN, MPH, CDCES, BC-ADM is a working educator and a nationally recognized diabetes expert.
All hours earned count toward your CDCES Accreditation Information
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.

People with type 1 or type 2 diabetes can experience hyperglycemic crises.
Which of the following is true about Diabetes Ketoacidosis (DKA)?
Click Here to Test your Knowledge

This course discusses common causes of hyperglycemia crises. Topics include hyperglycemia secondary to medications and insulin deprivation. The difference and similarities between Diabetes Ketoacidosis and Hyperosmolar Hyperglycemic Syndrome are also covered. Treatment strategies for all situations are included.
Objectives:
Intended Audience: A great course for healthcare professionals in the field of diabetes education looking for a straightforward explanation of identification and treatment of hyperglycemic crises.
Instructor: Beverly Thomassian RN, MPH, CDCES, BC-ADM is a working educator and a nationally recognized diabetes expert.
All hours earned count toward your CDCES Accreditation Information
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.
This course discusses common causes of hyperglycemia crises. Topics include hyperglycemia secondary to medications and insulin deprivation. The difference and similarities between Diabetes Ketoacidosis and Hyperosmolar Hyperglycemic Syndrome are also covered. Treatment strategies for all situations are included.
Objectives:
Intended Audience: A great course for healthcare professionals in the field of diabetes education looking for a straightforward explanation of identification and treatment of hyperglycemic crises.
Instructor: Beverly Thomassian RN, MPH, CDCES, BC-ADM is a working educator and a nationally recognized diabetes expert.

This presentation will include the latest information on Social Determinants of health, assessment strategies, and approaches. We will explore the psychosocial issues that can discourage individuals from adopting healthier behaviors and provides strategies to identify and overcome these barriers. Life studies are used to apply theory to real-life situations. A great course for anyone in the field of diabetes education or for those looking for a new perspective on assessment and coping strategies.
Objectives:
Intended Audience: A great course for healthcare professionals in the field of diabetes education looking for a straightforward explanation of identification and treatment of hyperglycemic crises.
Instructor: Beverly Thomassian RN, MPH, CDCES, BC-ADM is a working educator and a nationally recognized diabetes expert.
All hours earned count toward your CDCES Accreditation Information
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.