
Subscribe
eNewsletter

Ready to get certified?
Free CDCES Coach App
Download
Free Med Pocket Cards
An educational tool to increase knowledge of diabetes self-management terms and goals of care. In Spanish and English.
Players learn about diabetes management while having fun! A must have for support groups and in the classroom setting.
Perfect for Diabetes Awareness Activities. Up to 30 Can play! English on one side, Spanish on the other.
. DiaBingo is now available to download for free in English and Spanish!
Simply print out the player cards and choose items to use as markers to get started.
The questions are designed by our experts to help players become informed about diabetes and self-care in an upbeat and entertaining way. You are welcome to customize these questions as needed to make it relevant to your group.
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]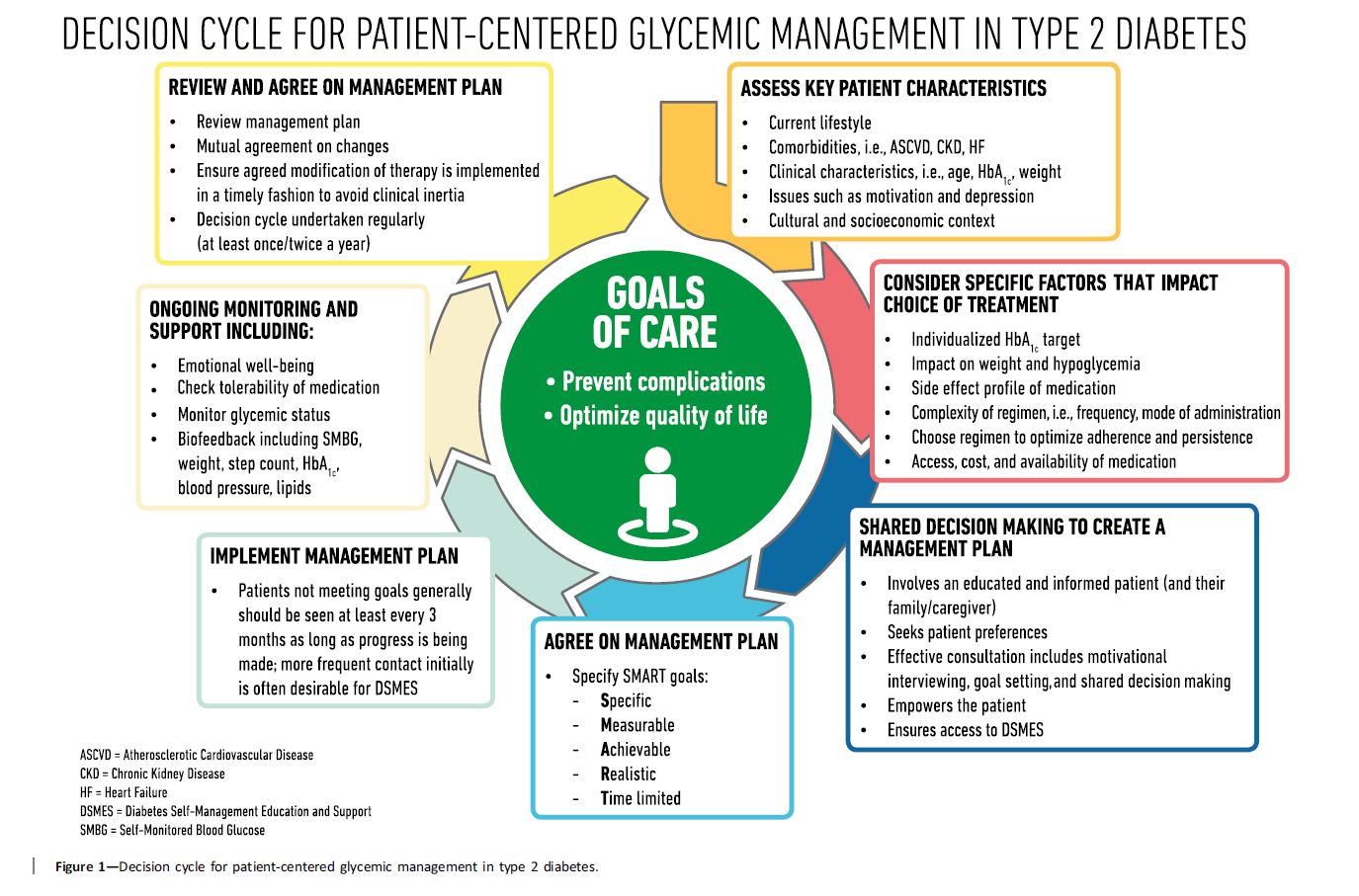
Management of Hyperglycemia in Type 2 Diabetes, 2018. https://doi.org/10.2337/dci18-0033
A Consensus Report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD).
This new consensus statement is a summary of findings based on a comprehensive literature search of peer reviewed articles published from 2014 to February 2018.
Here are some key statements from the Principles of Care Section that really stood out. In addition, the Decision Cycle Chart below, is an excellent summary of person centered considerations to determine the best path to take when deciding upon lifestyle and medication therapy.
Key concepts that I found intriguing and helpful from this section:
Therapeutic inertia, also called clinical inertia, refers to the lack of action even when blood glucose targets are above target. This is something I have frequently seen in my diabetes practice. A common example of this is a PWD on two to three different diabetes medication and basal insulin, with an A1c is greater than 9%, yet no changes in therapy are made for months or years. The causes of this inertia may complex, but can be a result of the provider, person with diabetes or the health care system.
To avoid or stop Clinical inertia, here are recommended strategies:
 Remission of type 2 diabetes: Mission Not Impossible.
Remission of type 2 diabetes: Mission Not Impossible.In the Management of Hyperglycemia in Type 2 Diabetes, 2018.A Consensus Report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD), on page 12 and 18, they reference the results of the DiRECT study below. They recommend that all overweight and obese PWD be advised of the health benefits of weight loss and encouraged to engage in an intensive lifestyle program to achieve weight loss reduction.
The DiRECT study, published in the Lancet in February 2018, aimed to assess whether intensive weight management within routine primary care would achieve remission of type 2 diabetes.
Goals of the study were weight loss of 15 kg or more and remission of diabetes, defined as A1c less than 6·5%, after at least 2 months off all antidiabetic medications, from baseline to 12 months.
To evaluate if this was possible, the research team initiated an open-label, cluster-randomised trial (DiRECT) at 49 primary care practices in Scotland and the Tyneside region of England. They recruited individuals aged 20-65 years who had been diagnosed with type 2 diabetes within the past 6 years, had a body-mass index of 27-45 kg/m2, and were not receiving insulin.
All diabetes and hypertension medications were stopped and very low calorie diet was started.
For 12 months, two groups consisting each of 149 participants were followed. The intervention group received weight management support and the control group received no weight loss intervention.
At end of study (12 months), diabetes remission was achieved in 68 (46%) participants in the intervention group and six (4%) participants in the control group
Diabetes remission rates associated with weight status at 12 months:
Other interesting observations:
Nine serious adverse events were reported by seven (4%) of 157 participants in the intervention group and two were reported by two (1%) participants in the control group. Two serious adverse events (biliary colic and abdominal pain), occurring in the same participant, were deemed potentially related to the intervention. No serious adverse events led to withdrawal from the study.
The results show that, at 12 months, almost half of participants in intervention group achieved, with a mean weight loss of 10%, experienced remission to a non-diabetes state without diabetes medications.
The authors conclude that remission of type 2 diabetes through a structured weight loss intervention is a practical target for primary care
Want to read more?
Lancet. 2018 Feb 10;391(10120):541-551. doi: 10.1016/S0140-6736(17)33102-1. Epub 2017 Dec 5.
 Increased knowledge of how gut bacteria ratios change as a marker of inflammation could help delay the development of Type 1 Diabetes. Researchers from the University of Queensland proposed that monitoring the microorganisms living in the gut may aid in understanding the disease better as a whole.
Increased knowledge of how gut bacteria ratios change as a marker of inflammation could help delay the development of Type 1 Diabetes. Researchers from the University of Queensland proposed that monitoring the microorganisms living in the gut may aid in understanding the disease better as a whole.
Participants in the study were all newly diagnosed with Type 1 Diabetes and were asked to provide a stool sample. The researchers analyzed these samples and found that, “certain proteins can be used to differentiate risk levels.”
UQ Diamantina Institute Senior Research Fellow Dr Emma Hamilton-Williams said: “By studying the stool samples of participants, we found that changes in gut bacteria weren’t just a side effect of the disease, but are likely related to disease progression.”
Research on the topic is new and fairly undeveloped. However, there are plans to carry out further research on the bacteria associated proteins, analyzing why they may signify an increased risk of Type 1 Diabetes expression.
The researchers are hoping to use this microbial information to monitor disease progression or develop therapies aimed at restoring a healthy microbiota in people at risk of type 1 diabetes.
For more information, Join our FREE Getting to the Gut, Meet Your Microbiome –
Live Webinar November 14th, 2018 at 11:30am PST
Read original article in Diabetes Care – Intestinal Metaproteomics Reveals Host-Microbiota Interactions in Subjects at Risk for Type 1 Diabetes –
And visit Monitoring gut changes could help delay type 1 diabetes.
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]
 As diabetes educators, having eye contact and listening carefully without distraction, is a critical part of our assessment. This initial meeting helps us sort out what is working with the person’s diabetes and what barriers might be getting in the way. The words we use, our body language, and how we engage in this encounter sets the stage for our ongoing working relationship. Plus, it can influence the self-perception of the person sitting across from us.
As diabetes educators, having eye contact and listening carefully without distraction, is a critical part of our assessment. This initial meeting helps us sort out what is working with the person’s diabetes and what barriers might be getting in the way. The words we use, our body language, and how we engage in this encounter sets the stage for our ongoing working relationship. Plus, it can influence the self-perception of the person sitting across from us.
However, many providers and educators may rely on computers to review notes and labs and to document the visit. This means there may be moments spent looking at the screen instead of the person sitting across from us.
Unfortunately, people with diabetes may feel that the computer is a distraction and a barrier to effective two-way communication.
Good news! There are strategies to compassionately engage with people with diabetes during the visit, while using the computer.
At the American College of Physicians Internal Medicine Meeting, speaker Wei Wei Lee MD, assistant professor of medicine at the University of Chicago, said utilizing the mnemonic HUMAN LEVEL provide guidance on how to succeed with electronic charting.
The mnemonic HUMAN LEVEL stands for:
H stands for honoring the golden minute. “The first minute of the visit with the patient should be completely technology free. Greet the patient, start with what’s on their mind, what their agenda is and then transition into using the computer,” she said.
U – Use the triangle of trust by placing the computer so that you and the patient can see the screen at the same time.
M – Maximize interaction by engaging the patients as much as possible, as you work on the computer.
A – Acquaint yourself with the patient’s chart before entering the examination room.
N – Not focusing exclusively on the screen during the visit, especially when the patient is talking about sensitive subjects.
For the complete mnemonic and more info on establishing a collaborative relationship, here is the article by Healio – “Doctors, patients benefit when the ‘eyes’ have it”
We have also created a resource page called the ABCs of Language Use in Diabetes, which provides insights on using strength-bases language in the clinical setting.
Within the medical community, we often use the terms “good cholesterol” and “bad cholesterol.” HDL, or high density lipoprotein cholesterol, is most often viewed as “protective from cardiovascular disease and death,” or the “good cholesterol” However, a recent study by the Emory University School of Medicine in Atlanta found that high levels HDL may actually be considered harmful.
The study assessed 60,000 men and women and tracked their cholesterol levels and risk for heart disease over the course of four years. HDL levels ranged, “from a low, less than 30 mg/dL to a high, greater than 60 mg/dL of blood.” Over the duration of the study, about 13% of test subjects either suffered from a heart attack or died.
“Specifically, patients with HDL levels exceeding 60 were found to have a 50 percent greater risk of heart disease death or heart attack, compared with those in the middle-range, the investigators reported.”
At the study’s end, the researchers concluded that patients with HDL levels in the middle-range of the spectrum — meaning between 41 to 60 mg/dL of blood — fared the best, having the lowest risk for heart attack or death from heart disease.
Allard-Ratick, head researcher on this study says concerned patients with high HDL cholesterol, “should continue to address other modifiable risk factors such as high blood pressure, smoking, and obesity to reduce cardiovascular disease”.
To read more about this study, visit Could too much HDL cholesterol be bad for your heart?
To learn more about cholesterol management, visit Cholesterol 101: An introduction.
 A study conducted by the Canadian Medical Association has found that common household disinfectants may increase the risk of obesity in children. The chemicals present in cleaning products we use every single day may alter the gut flora of children in their first few months of life. However, the children in households that used eco-friendly cleaners were less likely to be overweight.
A study conducted by the Canadian Medical Association has found that common household disinfectants may increase the risk of obesity in children. The chemicals present in cleaning products we use every single day may alter the gut flora of children in their first few months of life. However, the children in households that used eco-friendly cleaners were less likely to be overweight.
Researchers from across Canada looked at data on microbes in infant fecal matter among children enrolled in the Canadian Healthy Infant Longitudinal Development (CHILD) birth cohort. The study assessed 757 infants from the ages of three-four months. Their gut flora and BMI were recorded for the purpose of this research. Researchers found that, “infants living in households with disinfectants being used at least weekly were twice as likely to have higher levels of the gut microbes Lachnospiraceae at age three to four months.” said principal investigator Anita Kozyrskyj, a professor of pediatrics at the University of Alberta.
Lachnospiraceae is a common bacteria in the gut that is non-pathogenic. The children who were not exposed to disinfectants at an early age had lower BMIs than those with frequent exposure.
“When they were three years old, their body mass index was higher than children not exposed to heavy home use of disinfectants as an infant,” she added.
In contrast, the study found that babies living in households that used eco-friendly cleaners had different microbiota and were less likely to be overweight as toddlers.
No exact evidence has been found that changes of the microbiome may actually be linked to obesity. However, they call for further studies “to explore the intriguing possibility that use of household disinfectants might contribute to the complex causes of obesity through microbially mediated mechanisms.”
“Cleaning products have the capacity to change the environmental microbiome and alter risk for child overweight,” write the authors.This is particularly important during the developmental stages of life.
For more information on household cleaners and gut flora, visit Household cleaners may alter kid’s gut flora and contribute to being overweight.
Contributed By: Sofia Sepulveda