
Subscribe
eNewsletter

Ready to get certified?
Free CDCES Coach App
Download
Free Med Pocket Cards

What best describes the difference between a Certified Diabetes Care and Education Specialist (CDCES) and a person Board Certified in Advanced Diabetes Management (BC-ADM)?
Click Here to Test your Knowledge

Topics:
Coach Beverly is excited to share her insights on determining the best certification choice and the pathway to success. She will share her personal journey on achieving both her CDCES and BC-ADM over 20 years ago and how these credentials have impacted her opportunities as a diabetes specialist and president of her own company. We hope you can join us!
Can’t make it live? No worries. We will send post the recorded version to the Online University within 24 hours of the broadcast
Instructor: Beverly Thomassian RN, MPH, CDCES, has been Board Certified in Advanced Diabetes Management for over 20 years. She is an Associate Clinical Professor at UCSF, a working educator, and a nationally recognized diabetes expert. She has a Master’s Degree in Public Health from UCLA, with a focus on behavioral health and education.
All hours earned count toward your CDCES Accreditation Information
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.
JR lives with type 1 diabetes and is excited to eat a stack of blueberry pancakes with a new type of maple syrup sweetened with allulose. The syrup label reads that there are 28 grams of carbs in 2 Tablespoons of Zero Sugar Maple syrup. JR adds up the total carbs in the pancakes and syrup, and takes 6 units of bolus insulin (4 for the pancakes and 2 units for the syrup). Within a half hour, JR realizes their blood sugar is dropping fast and grabs some glucose tabs to treat the sudden low. Trying to figure out what went wrong, JR double confirms the nutrition in the pancakes and then takes a closer look at the Maple Syrup label.
Is the Maple Syrup to blame for the Unexpected Low Blood Sugar?
Looking at the label, JR confirms that there are 28 gm of carbs per serving of this unique maple syrup and 26 of those carb grams come from Allulose. Allulose is a low-calorie sugar that is Generally Recognized As Safe (GRAS) approved by the FDA in 2022. Allulose is considered a rare sugar found naturally in figs, raisins, wheat, maple syrup, and molasses or it can be commercially produced and added to foods. It’s roughly 70% as sweet as sugar and it tastes very similar. Allulose is hardly digested or absorbed, so it provides very few calories – approximately 0.4 calories per gram, compared with 4 calories per gram in table sugar.

Allulose labeling Can Cause Confusion for People Matching Insulin to Carbs
In 2019, US Food and Drug Administration (FDA) issued guidance, allowing food manufacturers to exclude allulose from total and added sugar counts on Nutrition and Supplement Facts labels. Like sugar alcohols and dietary fiber, allulose still counts towards total carbohydrates on the nutrition label.
The fact that allulose hardly raises blood sugar may lead people who match insulin to carbs to take more insulin than needed.
FDA Labeling Rule for allulose:
• Not included in “Total Sugars” or ”Added Sugars”
• Included in Total Carbohydrates
• Calories calculated with 0.4 kcals/gram
• Must be in the ingredient list
Take home message for People Counting Carbs for Accurate Insulin Dosing
Look on labels to see if allulose is listed under carbohydrates or included in the ingredient list. If it is, subtract allulose carbs from the total carbs to get an accurate carbohydrate measurement.
For other people, allulose may be a sweet-tasting alternative to sugar that provides few calories and doesn’t raise blood sugar.

For last week’s practice question, we quizzed participants on how much does Diabetes Cost the U.S? 69% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it below: Answer Question
Question: According to the recently published ADA report on the 2022 Economic Costs of Diabetes in the U.S., which of the following statements is most accurate?
Answer Choices:
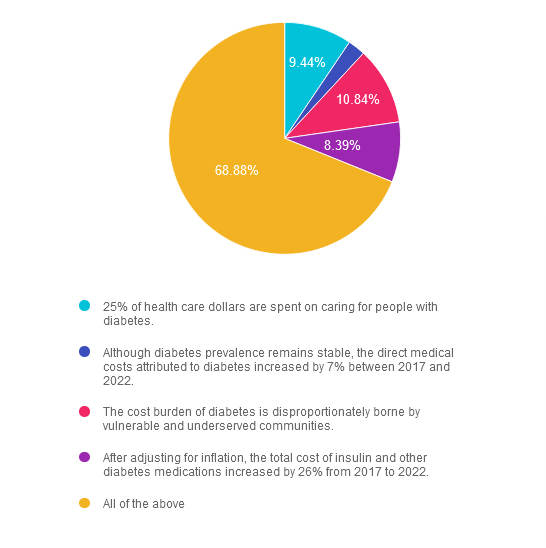
If you are thinking about taking the certification exam, this practice test question will set you up for success. Test writers anticipate possible answers based on the details in the question. They will wave those “juicy answers” right under your nose. Your job is to weed through the particulars, pluck out the most important elements and choose the BEST answer.
Answer 1 is incorrect. 9.44% chose this answer. “25% of health care dollars are spent on caring for people with diabetes.” Yes, a quarter of all health care dollars are spent on diabetes, with the majority of money spent on hospitalizations due to cardiovascular complications and medications. Read more details in the Diabetes Care Article, “Economic Costs of Diabetes in the U.S. 2022.
Answer 2 is incorrect. 2.45% of you chose this answer. “Although diabetes prevalence remains stable, the direct medical costs attributed to diabetes increased by 7% between 2017 and 2022.” The cost of treating diabetes keeps increasing, putting additional financial strain on people living with diabetes. Read more details in the Diabetes Care Article, “Economic Costs of Diabetes in the U.S. 2022.
Answer 3 is incorrect. About 10.84% of respondents chose this. “The cost burden of diabetes is disproportionately borne by vulnerable and underserved communities.” People who earn the least amount of money and live in under-resourced areas, continue to have the highest rates of diabetes and other chronic health conditions. Read more details in the Diabetes Care Article, “Economic Costs of Diabetes in the U.S. 2022.
Answer 4 is incorrect. About 8.39% of respondents chose this. “After adjusting for inflation, the total cost of insulin and other diabetes medications increased by 26% from 2017 to 2022.” Yes, the cost of medications keeps increasing, which may prevent many people from accessing optimal diabetes treatment. Read more details in the Diabetes Care Article, “Economic Costs of Diabetes in the U.S. 2022
Finally, Answer 5 is correct. 68.88% chose this answer. “All of the above” YES, GREAT JOB. Most of you chose the BEST Answer. Thank you for participating in our Question of the Week. All data is based on the Diabetes Care Article, “Economic Costs of Diabetes in the U.S. 2022”, published in November 2023
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!
All data is based on the Diabetes Care Article, “Economic Costs of Diabetes in the U.S. 2022”, published in November 2023

Topics:
This course discusses common causes of hyperglycemia crises. Topics include hyperglycemia secondary to medications & insulin deprivation. The differences & similarities between Diabetes Ketoacidosis and hyperosmolar Hyperglycemic Syndrome are also covered. Treatment strategies for all situations are included.
Can’t make it live? No worries. We will send post the recorded version to the Online University within 24 hours of the broadcast
Instructor: Beverly Thomassian RN, MPH, CDCES, has been Board Certified in Advanced Diabetes Management for over 20 years. She is an Associate Clinical Professor at UCSF, a working educator, and a nationally recognized diabetes expert. She has a Master’s Degree in Public Health from UCLA, with a focus on behavioral health and education.
All hours earned count toward your CDCES Accreditation Information
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
The use of DES products does not guarantee the successful passage of the diabetes certification exams. CBDCE & ADCES does not endorse any preparatory or review materials for the certification exams, except for those published by CBDCE & ADCES.
The American Association for the Study of Liver Diseases recently announced that they are updating their terms for Non-Alcoholic Steatohepatitis (NASH) and Non-Alcoholic Fatty Liver Disease (NAFLD).
Since NAFLD is considered the “hepatic manifestation of metabolic syndrome,” the organization wants the terminology to better reflect this metabolic inflammation and update the language to remove the stigma associated with the terms “fatty” and “non-alcoholic.”
According to the American Diabetes Association, NAFLD is prevalent in more than 70% of people living with diabetes. Early detection and intervention can decrease fat accumulation in the liver and lead to improved health. As diabetes care and education specialists, we can increase awareness and screenings while promoting lifestyle changes and medication therapy to save lives. One way to start the conversation is to share this updated Liver Nomenclature List with your colleagues.
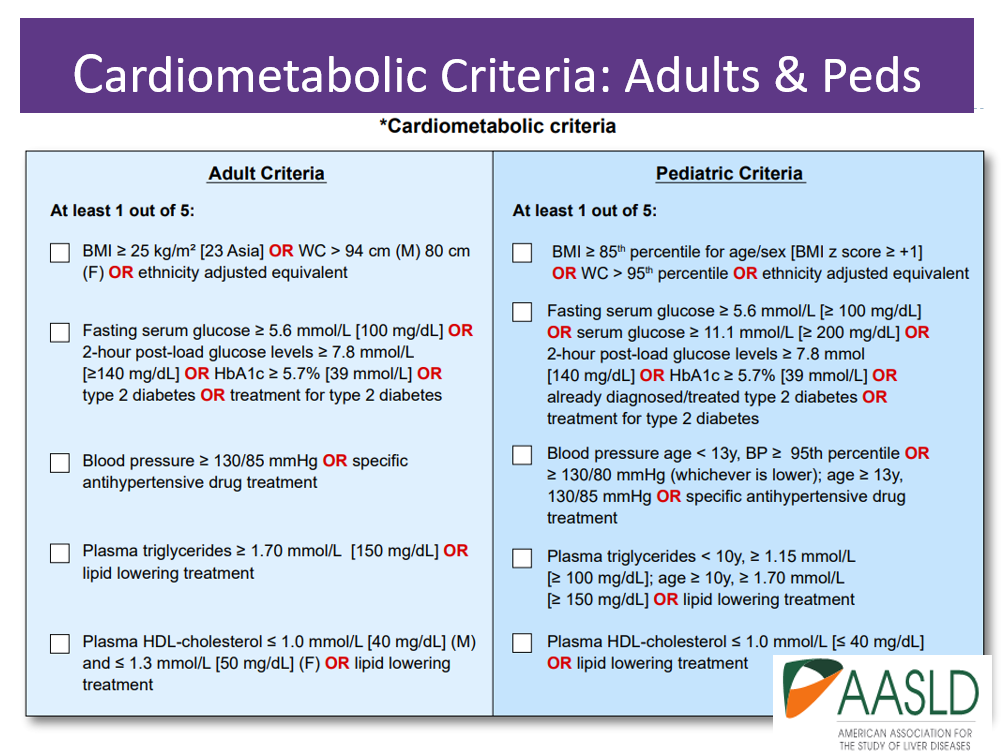
The new names, MASH and MAFLD, take into account the presence of liver disease along with cardiometabolic risk factors such as body weight, glucose levels, blood pressure, triglycerides, and HDL cholesterol levels (see CardioMetabolic table below).
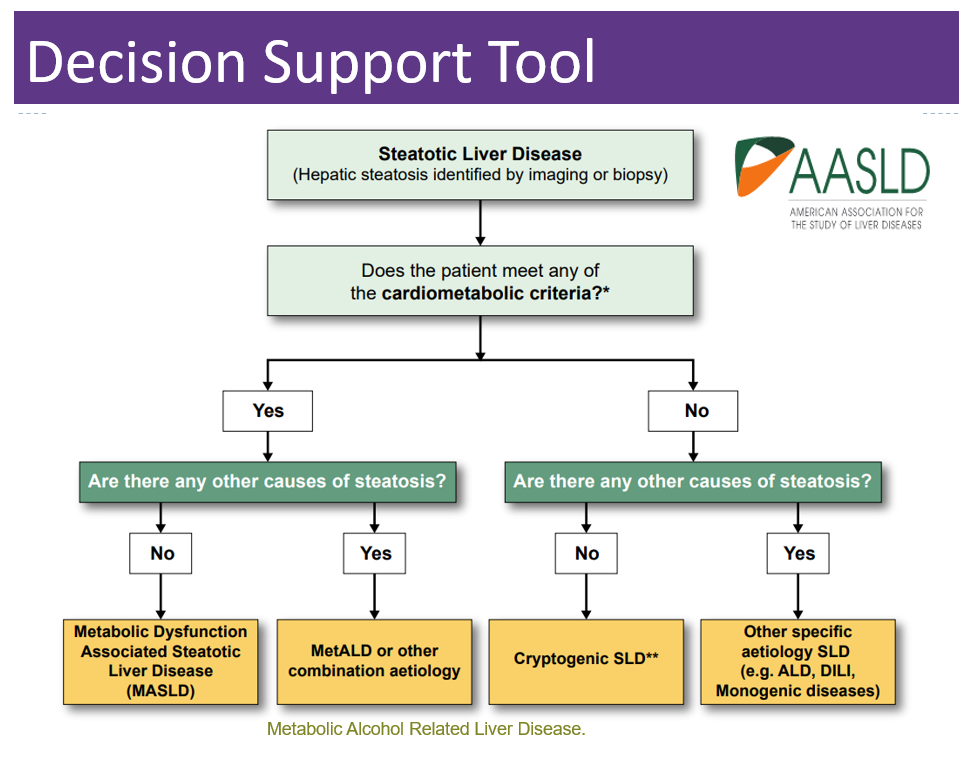
Below is a summary chart from the AADSL that reflects these important changes.

These new terms may not be universally accepted at first and the choice of name may vary by region and among healthcare professionals. Regardless of the name used, the management and understanding of the condition remain crucial to screening, identifying, and treating Steatotic Liver Disease.

Coach Bev invites you to join this 60-minute webinar that covers gastrointestinal health from top to bottom. Topics include; fatty liver disease diagnosis and treatment, intestinal complications associated with diabetes, keeping the microbiome healthy, and more. Join us to explore the magnificent wonders of diabetes and the gut.
Can’t make it live? No worries. We will send post the recorded version to the Online University within 24 hours of the broadcast
Instructor: Beverly Thomassian RN, MPH, CDCES, has been Board Certified in Advanced Diabetes Management for over 20 years. She is an Associate Clinical Professor at UCSF, a working educator, and a nationally recognized diabetes expert. She has a Master’s Degree in Public Health from UCLA, with a focus on behavioral health and education.
All hours earned count toward your CDCES Accreditation Information
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.

According to recent research by the ADA/EASD, about 10% of people admitted to the hospital in diabetes crisis have euglycemic diabetes ketoacidosis.
Since blood sugars are at normal levels or only slightly elevated, which of the following lab tests most accurately evaluate for euglycemic ketosis?
Click Here to Test your Knowledge

Topics:
This course discusses common causes of hyperglycemia crises. Topics include hyperglycemia secondary to medications & insulin deprivation. The differences & similarities between Diabetes Ketoacidosis and hyperosmolar Hyperglycemic Syndrome are also covered. Treatment strategies for all situations are included.
Can’t make it live? No worries. We will send post the recorded version to the Online University within 24 hours of the broadcast
Instructor: Beverly Thomassian RN, MPH, CDCES, has been Board Certified in Advanced Diabetes Management for over 20 years. She is an Associate Clinical Professor at UCSF, a working educator, and a nationally recognized diabetes expert. She has a Master’s Degree in Public Health from UCLA, with a focus on behavioral health and education.
All hours earned count toward your CDCES Accreditation Information
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.
We understand the important work you all do every day to support individuals living with and managing diabetes and prediabetes.

We are so thankful for the differences you all make in the world as you address disparities and improve the health of communities locally and across the nation.
We have been so inspired by our students and are so proud of each achievement. If you have a moment, stop by our CDCES Success Stories page to read about the incredible journeys students have taken to become diabetes educators and advocates.
At Diabetes Ed Services, we work diligently every day to provide diabetes information that is relevant, compassionate and cutting edge. We believe in the potential of all students, from people living with diabetes to health care professionals striving to enhance their knowledge. Thank you for being a part of our lives and community.
We will be closing shop starting today for the holidays. We will open our doors at 7am on Monday, well rested, a few pounds heavier and ready for our Cyber Monday Sale.
On behalf of the entire Diabetes Education Services Team, Happy Thanksgiving!
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.

For last week’s practice question, we quizzed participants on why we celebrate World Diabetes Day on Nov 14th. 39% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it below: Answer Question
Question: In 1923, the Nobel prize in Physiology or Medicine was awarded to Frederick Grant Banting and John James Richard MacLeod “for the discovery of insulin”. 100 years later, we celebrate this life-saving discovery each year on November 14th, a day designated as World Diabetes Day.
Why do we celebrate World Diabetes Day on November 14th? Please choose the best answer.
Answer Choices:
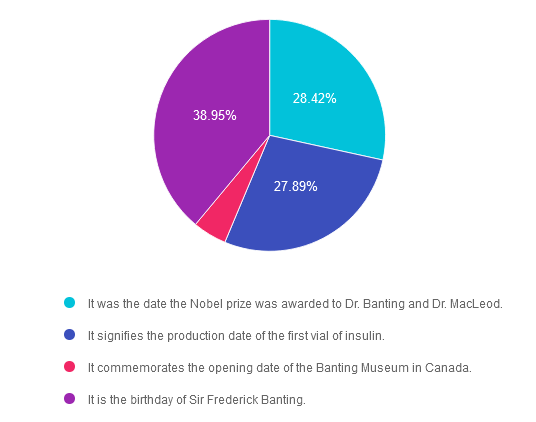
If you are thinking about taking the certification exam, this practice test question will set you up for success. Test writers anticipate possible answers based on the details in the question. They will wave those “juicy answers” right under your nose. Your job is to weed through the particulars, pluck out the most important elements, and choose the BEST answer.
Answer 1 is incorrect. 28.42% chose this answer. “It was the date the Nobel Prize was awarded to Dr. Banting and Dr. MacLeod.” This is not the reason, however it is interesting to note that the Nobel prize for the discovery of insulin was awarded on December 10, 1923 in Stockholm, Sweden.
Answer 2 is incorrect. 27.89% of you chose this answer. “It signifies the production date of the first vial of insulin.” Great guess. However, it wasn’t until 1923 that the first vials of insulin were commercially produced and distributed.
Answer 3 is incorrect. About 4.74% of respondents chose this. “It commemorates the opening date of the Banting Museum in Canada.” The Banting House is a former residence and current museum in London, Ontario, Canada, known as the “Birthplace of Insulin.” It is the house where Sir Frederick Banting woke up at two o’clock in the morning on October 31, 1920 with the idea that led to the discovery of insulin. Since 1984, the house has been a museum dedicated to Banting’s discovery and his life.
Finally, Answer 4 is correct. 38.95% chose this answer. “It is the birthday of Sir Frederick Banting.” YES, this is the best answer. Dr. Banting was born on November 14, 1891. That is why we celebrate World Diabetes Day on November 14th.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!
.png?h=459&iar=0&w=1459&hash=E665292742D2BABAECCFA59A56B88D3C)
November kicks off National Diabetes Month, a time to recognize that over 11% of Americans are living with diabetes and over 35% have prediabetes. Since diabetes results from a combination of genetics plus environment, there is a recognition that social determinants of health play a pivotal role in the development of diabetes and its complications. Through advocacy and education, we can inform individuals on best care for diabetes and support them in taking action to improve the health of their communities to prevent future diabetes. We have put together a list of FREE diabetes resources in English and Spanish to share with people living with prediabetes and diabetes. Thank you for your advocacy and belief that we can make a difference. Coach Beverly
All hours earned count toward your CDCES Accreditation Information
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.

According to the recently published ADA report on the 2022 Economic Costs of Diabetes in the U.S., which of the following statements is most accurate?
Click Here to Test your Knowledge
.png?h=459&iar=0&w=1459&hash=E665292742D2BABAECCFA59A56B88D3C)
November kicks off National Diabetes Month, a time to recognize that over 11% of Americans are living with diabetes and over 35% have prediabetes. Since diabetes results from a combination of genetics plus environment, there is a recognition that social determinants of health play a pivotal role in the development of diabetes and its complications. Through advocacy and education, we can inform individuals on best care for diabetes and support them in taking action to improve the health of their communities to prevent future diabetes. We have put together a list of FREE diabetes resources in English and Spanish to share with people living with prediabetes and diabetes. Thank you for your advocacy and belief that we can make a difference. Coach Beverly
All hours earned count toward your CDCES Accreditation Information
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.