
In a recent study published in Circulation, large, multisite produce prescription programs were associated with significant improvements in fruit and vegetable intake, food security, and health status for adults and children. At the conclusion of the food prescription program, participants experienced clinically relevant improvements in A1C, blood pressure, and body weight.
However, for this food-is-medicine strategy to work, it’s clear that the people will need long-term support.
The idea of food as medicine dates back to the ancient Greek doctor Hippocrates, and this new study adds to the evidence that a diet full of fruits and vegetables can help improve heart health.
Researchers evaluated the impact of “produce prescriptions,” which provide free fruits and vegetables to people with diet-related diseases including diabetes, obesity, and hypertension. The study included nearly 4,000 people in 12 states who struggle to afford healthy food. They received vouchers, averaging $63 a month, for up to 10 months, which could be redeemed for produce at retail stores or farmers markets, depending on the location.
Many people with diabetes struggle not only with food insecurity but also with nutrition insecurity. Improving nutrition security is about providing the right food to prevent or decrease the prevalence of chronic conditions like diabetes, heart disease and hypertension.
By providing adults with hypertension with access to healthy fruits and vegetables using a prescription program, this study demonstrated a systolic blood pressure decrease of 8 mm Hg and diastolic blood pressure decrease of about 5 mm Hg. In addition, among people with diabetes, A1C levels also declined significantly, by about 0.6 percent.
“Anything that lowers hemoglobin A1C and improves blood pressure control is beneficial,” says Dr. Dariush Mozaffarian, a cardiologist and professor at the Friedman School of Nutrition at Tufts University, where the research was conducted. The challenge is to maintain these reductions.
The research clearly indicates that food prescription programs are an effective strategy to improve health outcomes, but long-term funding for these programs is difficult to secure.
More research is needed to establish which individuals and communities will most benefit from which food assistance programs. Options include medically tailored meals, produce prescriptions, and community-based programs. The ultimate goal is to get to a place where these programs cover long-term benefits for people who need them most.
Resources and Related Articles
Wholesome Wave – partnering with community organizations to provide the right food to people at risk.
White House Conference on Hunger, Nutrition and Health
7 Ideas to Eat Healthier in the U.S.
Want to learn more about how nutrition can support people living with diabetes?
Join us LIVE in San Diego for our DiabetesEd Training Conference with Ashley LaBrier MS, RD, CDCES as she reviews MNT & Meal Planning

Two Registration Options
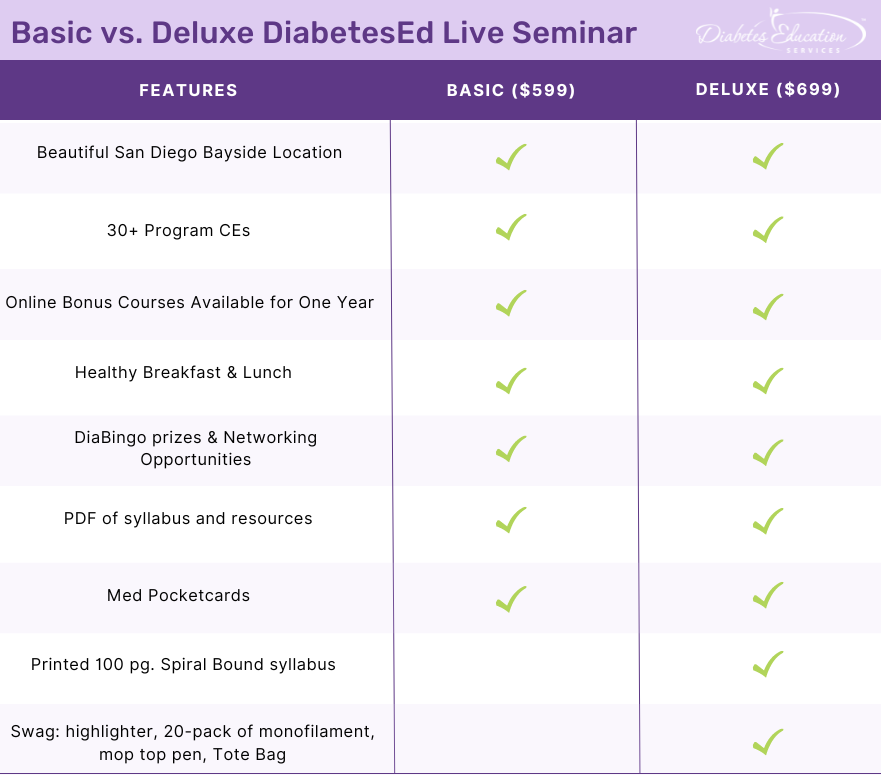
Join Coach Beverly and Team for two and a half days of knowledge-sharing, fun, networking, games with prizes, and “aha” moments in beautiful San Diego.
You don’t want to miss this one-of-a-kind learning opportunity. Get away from all those daily responsibilities and immerse yourself in a fun and intensive conference with plenty of networking opportunities.
Attendees will leave this conference with new tools and a more complete understanding of the latest advances in diabetes care, from medications to technology to Medical Nutrition Therapy!
Bring your colleagues and enjoy our friend discount.
Our team expertly translates the complex science of diabetes into understandable terms while keeping it real, practical, and fun.
Team of expert faculty includes:
- Diana Isaacs, PharmD, BCPS, BC-ADM, BCACP, CDCES – Educator of the Year, 2020
- Coach Beverly Thomassian, RN, MPH, CDCES, BC-ADM
- Ashley LaBrier, MS, RD, CDCES, Diabetes Program Coordinator
All hours earned count toward your CDCES Accreditation Information
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.




