
For last week’s practice question, we quizzed test takers on PZ who is upset by a recent diabetes diagnosis. 64% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it below: Answer Question
Question:
PZ is very upset that they were just diagnosed with diabetes and state “I want to get rid of this diabetes”. PZ has a BMI of 35 and elevated LDL cholesterol levels. Both of PZ’s parents had diabetes and died due to complications.
Based on the newly released ADA/EASD Consensus Statement, which intervention is recommended to get blood sugars to target and possibly lead to type 2 remission?
Answer Choices:
- Start an SGLT-2 Inhibitor plus metformin
- Lose 10-15% of current weight
- Immediately initiate a walking and strength training program.
- Encourage insulin pump therapy to preserve beta cell function.
Getting to the Best Answer
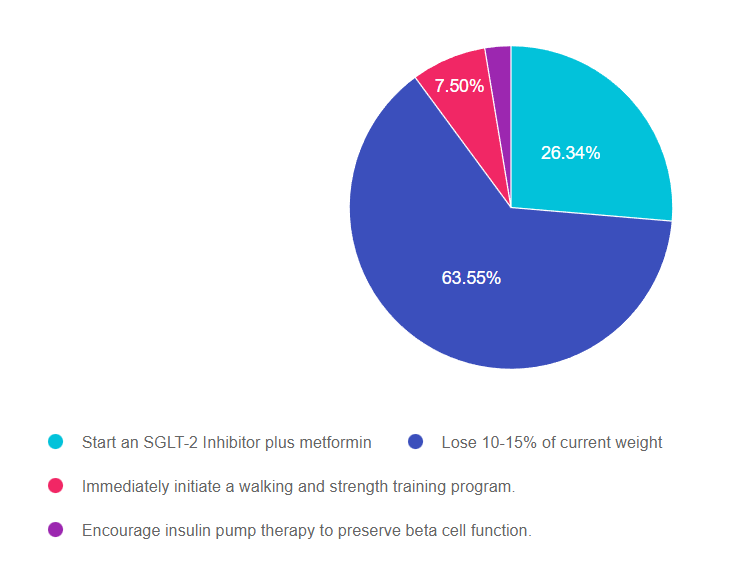
Answer 1 is incorrect. 26.34% chose this answer, “Start an SGLT-2 Inhibitor plus metformin.” This was a juicy answer, but not the best answer. The ADA/EASD consensus statement suggests starting combination therapy for people with an A1C of 8.5% or greater. However, in this case study, there is no information on PZ’s glucose level, therefore we can’t suggest initiating combination diabetes therapy.
Answer 2 is correct. 63.55% of you chose this answer, “Lose 10-15% of current weight.” YES, GREAT JOB. According to the ADA/EASD Consensus Statement, weight reduction as a targeted intervention can dramatically improved outcomes. “Weight loss of 5–10% confers metabolic improvement; weight loss of 10–15% or more can have a disease-modifying effect and lead to remission of diabetes, defined as normal blood glucose levels for 3 months or more in the absence of pharmacological therapy”. Plus, weight loss provides benefits that extend beyond glycemic management to decrease cardiometabolic risk factors and improve quality of life. In addition to referring all people with diabetes to a RD/RDN for MNT and encouraging regular activity, we can also recommend newer pharmacologic agents that not only lower glucose but support weight loss.
Answer 3 is incorrect. 7.50% of respondents chose this answer, “Immediately initiate a walking and strength training program.” While strength training and physical activity are both critical to promote health and improve insulin sensitivity, they will probably not be enough, by themselves, to get PZ’s A1C to target.
Finally, Answer 4 is incorrect. 2.60% chose this answer, “Encourage insulin pump therapy to preserve beta cell function.” While many people with type 2 diabetes are opting to use insulin pump therapy, initiating someone on insulin pump therapy before trying lifestyle and pharmacologic agents is not a recommended approach based on the latest consensus statement.
Thank you so much for reading this “Rationale of the Week”. You can download our Medication PocketCard or join our Webinar below for more information.
Want to learn more about this question? Join us for our
Meds for Type 2 Update; New ADA/EASD Consensus Statement
Level 2 | 1.25 CEs
Airs live on Wednesday, December 15th at 11:30 am PST

Plan on joining this exciting webinar that walks participants through the newly released, “Management of Hyperglycemia in Type 2 Consensus Report by the ADA and EASD”. These updated guidelines will be incorporated into the 2023 ADA Standards of Care, but you can get a early sneak peak by joining Coach Beverly on December 1st, 2022. She will highlight the revised guidelines with a focus on new elements and exciting changes on how we approach medication management for type 2 diabetes. Together, we will explore clinical factors to consider when determining the best strategy to improve glucose management in people with type 2 diabetes and other co-conditions. There will be a special focus on cardiovascular risk reduction and renal protection and addressing clinical inertia.
Objectives:
- Describe the role of Diabetes Care and Education Specialists in advocating for optimal therapeutic approaches.
- Discuss the application of the new ADA/EASD Guidelines to improve glucose and reduce CV and renal risk.
- List strategies to initiate and adjust oral and injectable therapy using a person-centered approach
Intended Audience: A great course for health care professionals seeking evidence-based information that improves the quality of life and outcomes.
Don’t worry if you can’t make it live. Your registration guarantees access to the recorded version in the Online University.
All hours earned count toward your CDCES Accreditation Information
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.




