
Subscribe
eNewsletter

Ready to get certified?
Free CDCES Coach App
Download
Free Med Pocket Cards

Our November 24th Question of the week was crazy hard and super simple at the same time. Less than half, 44% of respondents, chose the best answer, We thought that this was an important topic to discuss further, so we can pass on correct info to people living with diabetes.
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer below: Answer Question
Question: JR is going to stay home for Thanksgiving and decided to prepare a fantastic dinner. JR has type 1 diabetes and injects bolus insulin before each meal. JR takes 1 unit of insulin for each 10 gms of carbohydrates.
Using myfitnesspal to calculate JRs carb intake for the following festive meal, how much insulin would JR need to inject?
Answer Choices:
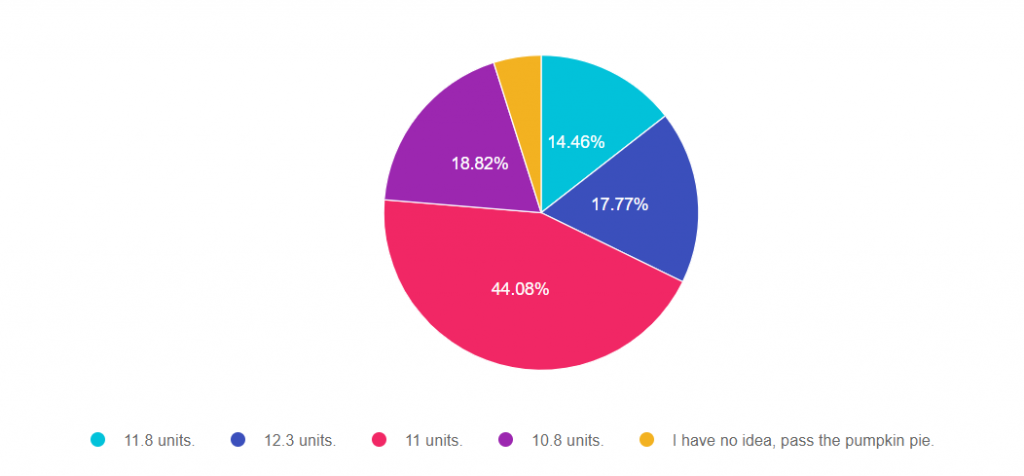
As shown above, the most common choice was option 3, the second most common answer was option 4, then option 2, then option 1, and finally option 5.
If you are thinking about taking the certification exam, this practice test question will set you up for success. Test writers may lure you in to choosing a more complicated answer, when the simplest answer may be the best choice. That is true for this question.
The most important feature of this question is “how much insulin would JR need to inject?” Since he is injecting insulin, no syringe or pen would allow him to inject 1/10th of a unit. Based on this info, the only plausible answer is 11 units or answer 3. But, for fun, here is the carb calculation.
JR will be eating 109 gms of carb. His insulin to carb ratio is 1/10. 109 / 10 = 10.9 units of insulin, then round up to 11 units.

Answer 1 is incorrect. 14.46% chose this answer. “11.8 units .”
Answer 2 is incorrect. 17.77% of you chose this answer. “12.3 units.”
Answer 3 is correct. 44.08% of respondents chose this. “11 units.”
Answer 4 is incorrect. 19.49% chose this answer. “10.8 units.”
Answer 5 is incorrect. 4.88% chose this answer. ” I have no idea, pass the pumpkin pie.”
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!
“This is one of the best review courses I’ve ever taken.”
“I learned so much from the CDCES Exam Prep Toolkit. I now have an assessment after taking the practice exam on the areas I need to focus my studying.”
Student Feedback

Whether you are preparing for the CDCES or BC-ADM exam, this test-taking toolkit is designed to prepare you for success. This toolkit includes two courses with over 200 practice questions to help you prepare and simulate the exam. Plus, we have added a FREE bonus course, Language, and Diabetes – What we say matters. Coach Beverly added this course because she believes it contains critical content for the exam and for our clinical practice!
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.

Our November 17th Question of the week quizzed test takers on COVID-19 and diabetes. Less than half, 48% of respondents, chose the best answer, We thought that this was an important topic to discuss further, so we can pass on correct info to people living with diabetes.
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer below: Answer Question
Question: COVID cases are surging throughout the United States. Providing the best care for people with diabetes is especially important during this crisis. Which of the following statements regarding diabetes and COVID is most accurate?
Answer Choices:
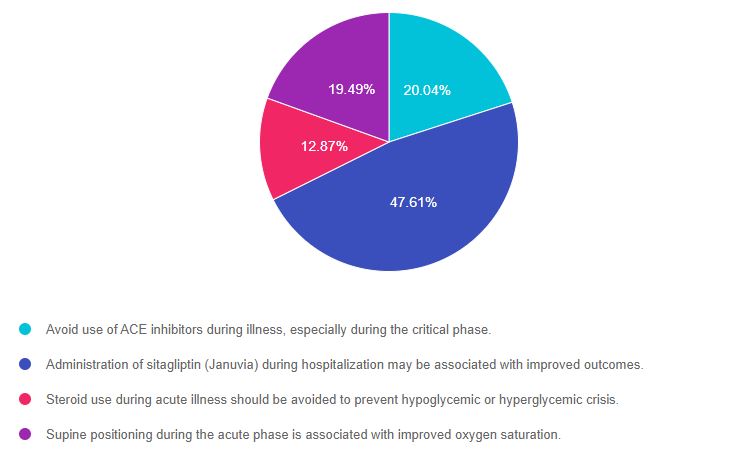
As shown above, the most common choice was option 2, the second most common answer was option 1, then option 4, and finally option 3.
If you are thinking about taking the certification exam, this practice test question will set you up for success. Test writers anticipate possible answers based on the details in the question. They will wave those “juicy answers” right under your nose. Your job is to weed through the particulars, pluck out the most important elements and choose the BEST answer.
Answer 1 is incorrect. 20.04% chose this answer. “Avoid use of ACE inhibitors during illness, especially during the critical phase.” Since the corona virus enters the body via ACE2 receptors, some early recommendations included stopping ACE inhibitors in those with COVID-19. However, scientists quickly discovered that stopping ACE inhibitors did NOT improve outcomes and that ACE inhibitors should be continued.
Answer 2 is correct. 47.61% of you chose this answer. “Administration of sitagliptin (Januvia) during hospitalization may be associated with improved outcomes.” YES. New research demonstrates that people with diabetes and COVID-19 started sitagliptin (Januvia) on hospital admission, experience dramatic decreases mortality and improved outcomes.
See our Blog Post – Sitagliptin Improves Outcomes here
Answer 3 is incorrect. About 12.87% of respondents chose this. “Steroid use during acute illness should be avoided to prevent hypoglycemic or hyperglycemic crisis.” It is true that steroids can contribute to hyperglycemia in people with diabetes. However, since steroids have been shown to be lifesaving for very ill people with COVID, with or without diabetes, research supports administering the steroid while managing resultant hyperglycemia with insulin therapy.
Finally, Answer 4 is incorrect. 19.49% chose this answer. “Supine positioning during the acute phase is associated with improved oxygen saturation.” Research has shown that “prone” positioning (laying on belly) can improve alveolar oxygenation and outcomes. More info here.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!

Purchase recording of our Live Webinar on December 2 | Earn 1.5 CE | $19
With the surge in new COVID cases, what is the essential information health care professionals and Diabetes Specialists need to navigate this overwhelming crisis?
What are the best practices to care for people with diabetes and COVID-19 in the outpatient and hospital setting?
Coach Beverly Thomassian, RN, MPH, CDCES, BC-ADM, has completely updated this critical presentation, to bring health care professionals up-to-date on the current state of COVID and its impact on diabetes care. She summarizes key information including critical teaching points and management strategies for people with diabetes who develop a COVID-19 infection.
Topics Include:
If you miss the live version, your registration guarantees access to the recorded version.
Join us to learn critical information about Diabetes and COVID Management

Instructor: Beverly Thomassian RN, MPH, CDCES, has been Board Certified in Advanced Diabetes Management for over 20 years. She is an Associate Clinical Professor at UCSF and Touro University and a nationally recognized diabetes expert.
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.

JL has diabetes and injects insulin 2-3 times a day. JL is at a holiday party and is struggling with wanting a holiday spirit. Which of the following is the best approach for JL?

A. JL is on insulin and needs to avoid alcohol.
B. JL needs to take extra insulin to cover alcohol.
C. Wine is a better choice than a margarita.
D. For every alcohol drink, JL needs to eat 15 gms of carb.
E. Both C & D.
Click here to test your knowledge!

Join our Live Webinar on December 2 at 11:30 am PST | Earn 1.5 CE | $19
With the surge in new COVID cases, what is the essential information health care professionals and Diabetes Specialists need to navigate this overwhelming crisis?
What are the best practices to care for people with diabetes and COVID-19 in the outpatient and hospital setting?
Coach Beverly Thomassian, RN, MPH, CDCES, BC-ADM, has completely updated this critical presentation, to bring health care professionals up-to-date on the current state of COVID and its impact on diabetes care. She summarizes key information including critical teaching points and management strategies for people with diabetes who develop a COVID-19 infection.
Topics Include:
If you miss the live version, your registration guarantees access to the recorded version.
Join us to learn critical information about Diabetes and COVID Management

Instructor: Beverly Thomassian RN, MPH, CDCES, has been Board Certified in Advanced Diabetes Management for over 20 years. She is an Associate Clinical Professor at UCSF and Touro University and a nationally recognized diabetes expert.
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]
Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.

As we continue to navigate this long-lasting pandemic there has been so much loss and heartache.
Years ago I went to a conference on preventing burnout in healthcare providers with Dr. J. Bryan Sexton, associate professor in psychiatry and behavioral sciences at Duke’s School of Medicine and an expert in the idea of resilience. He impressed me and I have talked about his conference to many colleagues over the years.
I loved sharing his wisdom with my clients, because of studies that link resilience to better diabetes self management. (1)
Lately, as I have been struggling with overwhelming feelings of sadness, I have remembered to practice some of his tools to cultivate resilience. Cultivating resiliency is something that takes daily focus. To cultivate means to nurture, grow, and encourage resilient behaviors.
Three Good Things
Humans are hard-wired to remember the negative aspects of our day, but flipping around the natural inclination is simple.
Building resilience is possible by focusing on positive emotions – joy, serenity, hope gratitude, inspiration, pride, love, awe, and amusement.
Promoting positive thoughts and building resilience can be as easy as taking notes each night before bed. Think of three things that happened during the day that went well and your role in the positive outcome, then jot down those three things. Best results for this exercise come after 14 consecutive days. Empirical evidence shows that this elevates brain serotonin with positive effects on our mood that last for months. (2)
Show Gratitude

Grab a pen and paper and write a letter of appreciation to someone- anyone. Take five minutes to explain something they did, how it impacted you and the benefits you received. Whether you share the letter or not, Dr. Sexton said it can have lasting impacts, increasing happiness while lowering depressing thoughts because focusing on benefits forces us to linger on positive thoughts.
Rediscover Awe
Through an “awe intervention,” you can create a sense of slowed down time, which offers a calming sensation and a feeling of having more time available.
Awe also helps us to feel inspired. I call awe intervention, “joyful thanksgiving”. It is a practice that I am doing in which I acknowledge and give a little extra gratitude for the many amazing sights, sounds, tastes, relationships, information, and emotions that excite me and create awe right from the moment when I wake up.
I began to feel grateful for this medicinal food. Oats, blueberries, banana, and nuts contain water soluble fiber which slow the absorption of sugar and fat from food, and therefore help prevent spikes in blood sugar and blood fat, possibly reducing the inflammatory response to food. (3)(4)
Fiber is a super food which provides important nutrition for our intestinal bacteria to live and prosper, that’s why fiber is called a pre-biotic. Vegetables, fruit, whole grains, nuts and legumes remain the single best sources of fiber in the diet. High-fiber vegetables include many of the green leafy vegetables like kale, collard greens, chard, arugula, and even lettuces. Whole-grain sources of fiber include oats, quinoa, barley and rye. Legumes include beans like peas, soy, black, pinto and lentils.
Encouraging our clients to consider adding more fiber rich dishes to the holiday meals this season and perhaps telling them about Dr. Sexton’s tools for cultivating resilience may help them to feel happier and more hopeful and contribute to better blood sugar control.
½ cup unsweetened coconut milk beverage
½ cup old-fashioned oats
½ TB chia seeds
½ banana
1 tsp maple syrup
½ cup blueberries
2 TB chopped walnuts
1/8 tsp cinnamon
Combine coconut milk, oats, chia, banana, maple syrup in a pint-sized jar and stir. Top with blueberries and coconut. Cover and refrigerate overnight. Heat up and sprinkle with walnuts and cinnamon in the morning.
285 calories, 6 gm protein, 57 gms carbohydrate, 7 gms fiber 6 gm fat
Meta-Analysis. Nutrients. 2015 Dec; 7(12): 10369-10387p. 1392:8
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]

JR is going to stay home for Thanksgiving and decided to prepare a fantastic dinner. JR has type 1 diabetes and injects bolus insulin before each meal. JR takes 1 unit of insulin for each 10 gms of carbohydrates.
Using myfitnesspal to calculate JRs carb intake for the following festive meal, how much insulin would JR need to take?

Click here to test your knowledge!

Join our Live Webinar on December 2 at 11:30 am PST | Earn 1.5 CE | $19
With the surge in new COVID cases, what is the essential information health care professionals and Diabetes Specialists need to navigate this overwhelming crisis?
What are the best practices to care for people with diabetes and COVID-19 in the outpatient and hospital setting?
Coach Beverly Thomassian, RN, MPH, CDCES, BC-ADM, has completely updated this critical presentation, to bring health care professionals up-to-date on the current state of COVID and its impact on diabetes care. She summarizes key information including critical teaching points and management strategies for people with diabetes who develop a COVID-19 infection.
Topics Include:
If you miss the live version, your registration guarantees access to the recorded version.
Join us to learn critical information about Diabetes and COVID Management

Instructor: Beverly Thomassian RN, MPH, CDCES, has been Board Certified in Advanced Diabetes Management for over 20 years. She is an Associate Clinical Professor at UCSF and Touro University and a nationally recognized diabetes expert.
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.
The winter and holiday seasons can be stressful and wear us down, especially during the pandemic. We tend to spend more time indoors. To help out, we have some suggestions that will not only help with stress management but can also boost your immunity.
Walking outside in nature and drinking in an “oxygen cocktail” feels good, but does it benefit our immunity?
You might be familiar with the term “Forest bathing” or shinrin-yoku. In Japanese, Shinrin means “forest,” and yoku means “bath.” Shinrin-yoku means bathing in a forest atmosphere or taking in the forest through our senses.
Research has demonstrated that trips to the forest can not only make us feel better by lowering muscle tension, boosting sleep, and reducing blood pressure. It turns out being in nature also enhances our immune systems by increasing the number and activity of our lympocytes and killer T cells.
When we walk among trees and plants, we breathe in airborne chemicals from plants called phytoncides.
Plants produce these chemicals to protect themselves from insects, bacterial and fungal infections. Phytoncides help plants fight disease.
These cells kill tumor and virus-infected cells in our bodies. In one study, increased NK activity from a 3-day, 2-night forest bathing trip lasted for more than 30 days.

According to Dr. Qing Li, author of the book, Forest Bathing, the key to unlocking the power of the forest is in the five senses:
To read more, click here.

The holiday season can also be stressful and throw us off our normal routine. This can compromise our sleep and our overall eating habits.
To help everyone feel their best during this holiday season, we have ten strategies for you and your patients. And even if you can’t do all ten, just pick one or a few that you feel you can commit to and succeed with most of the time.
We have created a 10 Steps to Survive the Holidays PDF – a handout that includes the info below to print and share with your friends, patients, and colleagues!

Recorded & Ready for Viewing
Coach Beverly Thomassian, RN, MPH, CDCES, BC-ADM, has completely updated this critical presentation, to bring health care professionals up-to-date on the current state of COVID and its impact on diabetes care. She summarizes key information including critical teaching points and management strategies for people with diabetes who develop a COVID-19 infection.
Topics Include:
Join us to learn critical information about Diabetes and COVID Management

Instructor: Beverly Thomassian RN, MPH, CDCES, has been Board Certified in Advanced Diabetes Management for over 20 years. She is an Associate Clinical Professor at UCSF and Touro University and a nationally recognized diabetes expert.

See Full Free Resource Catalog
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.

Our November 10th Question of the week quizzed test takers on intestinal bacterial health and diabetes. 40% of respondents chose the correct answer, while 60% did not. We thought that this was an important topic to discuss further, so we can pass on correct info to people living with diabetes.
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer below: Answer Question
Question: Intestinal health and diabetes are co-related. Which of the following statements is true?
Answer Choices:
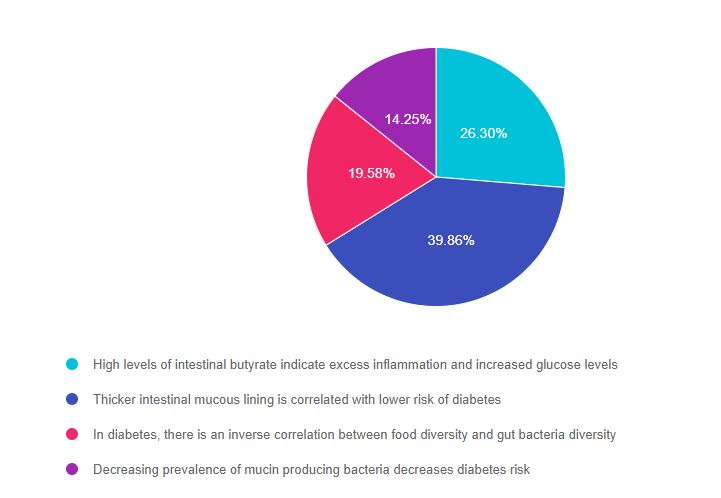
As shown above, the most common choice was option 2, the second most common answer was option 1, then option 3, and finally option 4.
If you are thinking about taking the certification exam, this practice test question will set you up for success. Test writers anticipate possible answers based on the details in the question. They will wave those “juicy answers” right under your nose. Your job is to weed through the particulars, pluck out the most important elements and choose the BEST answer.
Answer 1 is incorrect. 26.30% chose this answer. “High levels of intestinal butyrate indicate excess inflammation and increased glucose levels.”
Butyrate is one of the main metabolites produced in the colon by bacterial fermentation of dietary fiber. When it comes to gut health, higher levels of butyrate, a short-chained fatty acid, indicate higher fiber consumption and overall gut health and happiness.
Answer 2 is correct. 39.86% of you chose this answer. “Thicker intestinal mucous lining is correlated with a lower risk of diabetes”.
The image to the right is a great illustration. You can see that the thicker the mucus lining in the intestinal lumen, the less overall inflammation and leaky gut. A diet high in fiber feeds the microbiota in charge of maintaining a thick and healthy mucous lining.
Answer 3 is incorrect. About 19.58% of respondents chose this. “In diabetes, there is an inverse correlation between food diversity and gut bacteria diversity”
There is actually a direct correlation between food diversity and gut bacterial diversity. Enjoy a rainbow of foods, with lots of veggies, seeds, legumes, nuts, fruit, and whole grains.
Finally, Answer 4 is incorrect. 14.25% chose this answer. “Decreasing the prevalence of mucin-producing bacteria decreases diabetes risk.”
Mucin producing bacteria, like Akkermansia Muciniphila, help maintain a healthy mucus lining in the intestinal lumen. This is associated with less overall inflammation and leaky gut. A diet high in fiber feeds the microbiota in charge of maintaining a thick and healthy mucous lining.
We hope you appreciate this week’s rationale!
To learn more about this exciting topic, please join our
“This Webinar is filled with Bev’s energy, knowledge, and passion for diabetes that she replicates in all her teachings. She puts a demand on herself to be a mentor to all. Her information is well organized, full of current/relevant research, and helps CDCES’ view into the future as a changing world impacts diabetics. I find her to be the most exciting and engaging educator and … OUTSTANDING teacher!!” – recent participant
New Webinar topics:
This one-hour complimentary journey will expand your view of how the trillions of bacterial hitchhikers profoundly influence our health. We will discuss how foods, the environment, and our medical practices have impacted our gut bacteria over time and strategies we can take to protect these old friends.
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.
Rationale of the Week | Hyperglycemia and Cystic Fibrosis [yikes-mailchimp form=”1″]
The COVID-19 Pandemic is taking a toll on people with diabetes.
Although people with diabetes are not more likely than the general population to be infected by COVID-19, they have much higher mortality rates than people without diabetes once infected with the virus.

The Corona Virus appears to have two portals of entry in humans.
In a recent study released in September in Diabetes Care, “Type 2 Diabetes and COVID-19: A Multicenter, Case-Control, Retrospective, Observational Study by Solerte et al”, the researchers demonstrated reduced mortality, improved clinical outcomes, and a greater number of hospital discharges for those started on sitagliptin on admission.
The COVID-19 virus seems to bind to the DPP-IV enzyme and the enzymatic activity of DPP4 causes overexpression of inflammatory cytokines, exaggerating the inflammatory response.
Since sitagliptin is a DPP-IV inhibitor, the researchers believe that the medication inhibited the virus’s ability to bind to DPP-IV. This had a net effect of decreasing the intense inflammatory response, often termed the “cytokine storm” associated with COVID-19 infections.
This Multicenter, Case-Control, Retrospective, Observational Study followed 338 consecutive patients with type 2 diabetes and COVID-19 admitted to Northern Italy hospitals.
Included in this study were 169 patients on sitagliptin and 169 on the standards of care. All patients had pneumonia and exhibited oxygen saturation <95% when breathing ambient air or when receiving oxygen support.
RESULTS: Treatment with sitagliptin at the time of hospitalization was associated with:
Sitagliptin contributed to a lowered risk and progression of acute respiratory complications for people with type 2 diabetes and COVID-19.
This research suggests that DPP-4 inhibitors can help decrease COVID-19-related immune overreaction in people with diabetes and dramatically improve outcomes.
Read article here >> Sitagliptin Treatment at the Time of Hospitalization was Associated with Reduced Mortality in Patients with Type 2 Diabetes and COVID-19: A Multicenter, Case-Control, Retrospective, Observational Study, Solerte et al. Diabetes Care 2020, Sept

Recorded & Ready for Viewing
Coach Beverly Thomassian, RN, MPH, CDCES, BC-ADM, has completely updated this critical presentation, to bring health care professionals up-to-date on the current state of COVID and its impact on diabetes care. She summarizes key information including critical teaching points and management strategies for people with diabetes who develop a COVID-19 infection.
Topics Include:
Join us to learn critical information about Diabetes and COVID Management

Instructor: Beverly Thomassian RN, MPH, CDCES, has been Board Certified in Advanced Diabetes Management for over 20 years. She is an Associate Clinical Professor at UCSF and Touro University and a nationally recognized diabetes expert.
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]
Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.