
Subscribe
eNewsletter

Ready to get certified?
Free CDCES Coach App
Download
Free Med Pocket Cards

Our October 13th Question of the week quizzed test-takers insulin pump management for an older person with type 1 and dementia. The majority of respondents (82%) chose the correct answer! Great job. Even though most of you got it right, we think it is an important topic to explore and discuss.
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer below: Answer Question
Question: AJ is 89 years old with type 1 diabetes and is a caretaker for a partner with dementia. AJ is on an insulin pump and uses a meter to check blood glucose levels 4-7 times a day. AJ mentions that they were surprised the other morning that their blood glucose was 59 mg/dl and they felt fine.
Based on this, what is the best action?
Answer Choices:
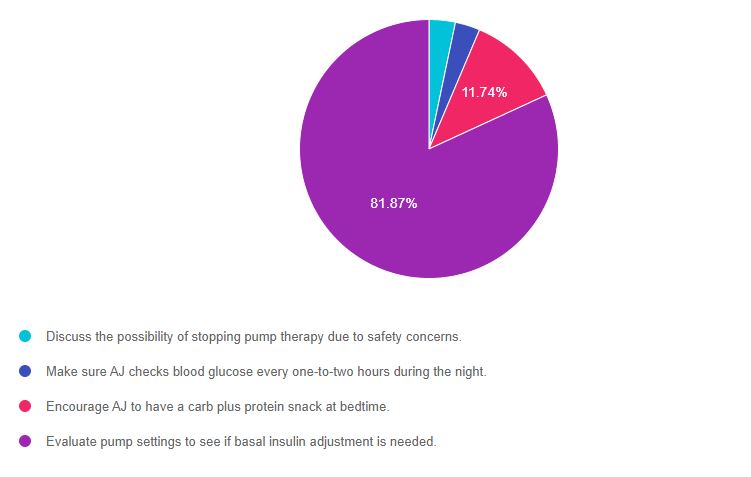
As shown above, the most common choice was option 4, the second most common answer was option 3, then option 1, and finally option 2.
If you are thinking about taking the certification exam, this practice test question will set you up for success. Test writers anticipate possible answers based on the details in the question. They will wave those “juicy answers” right under your nose. Your job is to weed through the particulars, pluck out the most important elements and choose the BEST answer.
Answer 1 is incorrect. 3.28% chose this answer, “Discuss the possibility of stopping pump therapy due to safety concerns”. For older clients, safety is a top priority. However, based on this vignette, there has not been a pattern of lows and AJ is able to check glucose levels on a regular basis. In addition, for people with type 1, insulin pump therapy decreases the ups and downs associated with multiple daily injections and offers more dosing flexibility. So instead of stopping the pump, suggesting the use of continuous glucose monitor could be another option.
Answer 2 is incorrect. 3.11% of you chose this answer, “Make sure AJ checks blood glucose every one-to-two hours during the night”. Safety is a big issue for older adults, but checking every one-to-two hours is not realistic and would be very disruptive to sleep. They could consider a 2-3am glucose check to see if blood sugars are trending down. If blood sugars are trending down, they could decrease the basal rate overnight to protect against morning hypoglycemia.
Answer 3 is incorrect. About 11.74% of respondents chose this, ” Encourage AJ to have a carb plus protein snack at bedtime”. This is not the best answer because we don’t have any information on the level of nighttime glucose. It is true, that for older people on insulin pumps, going to sleep with a glucose of 150 mg/dl or greater is important to protect against nocturnal hypoglycemia. But, if the bedtime glucose was less than 150 mg/dl, AJ would just need a 15-30 gm carbohydrate snack. Studies have found that adding protein doesn’t help prevent hypoglycemia, it is the carbohydrates that protect against falling blood sugars.
Lastly, we don’t want to have to “feed the insulin”. If basal insulin is set correctly overnight, AJ would wake up with glucose on target, even without eating a bedtime snack.
Finally, Answer 4 is correct. 81.87% chose this answer, “Evaluate pump settings to see if basal insulin adjustment is needed”. YES! If basal insulin is set correctly overnight, AJ would wake up with glucose on target.
I encourage people on insulin pumps to write down their basal rates, carb to insulin ratios, and corrections factors, on a piece of paper with a date. Then take a picture of it on their phone, so they can always access it and evaluate if those calculations might need a little tweaking as the body changes over time. And of course, we need to include the support person in all these discussions since AJ is living with dementia.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!
“This is one of the best review courses I’ve ever taken.”
“I learned so much from the CDCES Exam Prep Toolkit. I now have an assessment after taking the practice exam on the areas I need to focus my studying.”
Student Feedback

Whether you are preparing for the CDCES or BC-ADM exam, this test-taking toolkit is designed to prepare you for success. This toolkit includes two courses with over 200 practice questions to help you prepare and simulate the exam. Plus, we have added a FREE bonus course, Language, and Diabetes – What we say matters. Coach Beverly added this course because she believes it contains critical content for the exam and for our clinical practice!
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.

JR has had prediabetes for several years, with A1c’s of 6.0-6.4%. JR is now experiencing sudden hyperglycemia and an A1c is 9.2%, GAD is positive, transglutaminase is negative and TSH is 1.4.
What is the most likely diagnosis?
Click here to test your knowledge!

Beverly has custom designed this deluxe course bundle to prepare you for your CDCES (formerly known as CDE) or BC-ADM Exam.
This Deluxe Prep Bundle includes:
Use code “SUCCESS10” by October 31st to receive 10% off.
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.
With everything going on in the world, I thought today we would move gently into Monday with a poem by Lucille Clifton.

may the tide
that is entering even now
the lip of our understanding
carry you out
beyond the face of fear
may you kiss
the wind then turn from it
certain that it will love you back
may you
open your eyes to water
water waving forever
and may you in your innocence
sail through this to that
~ Lucille Clifton (at St. Mary’s)
View OnDemand FREE Webinar Now

Being a diabetes educator can be challenging. This one-hour presentation by Heather Nielsen, MA, LPC, CHWC will provide diabetes educators with helpful hands-on strategies to incorporate mindfulness and self-compassion into our daily lives and professional practice. As a counselor and a certified wellness coach, Heather has an abundance of wellness wisdom to share with educators who provide lifesaving diabetes education and support to people living with diabetes.
Objectives:
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]
Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.
Our October 6th Question quizzed test takers on the Transtheoretical Behavior Change Model. 50% of respondents chose the correct answer, while 50% did not. Since this is an important topic for the exam and our clinical practice, we want to explore this topic further.
Before we dive into the rationale, let’s do a quick review of this model and the stages of change included in the Transtheoretical Model. The slide below, created by Diane Pearson, RN, MPH, CDCES, provides a quick visual view of the model including the different stages of change.
Take a minute to look through:

Now that you have studied the model and you are ready to try the question, click here: Answer Question. If you have already answered the question, keep scrolling down for the rationales.
Question: JR has type 2 diabetes and an A1c of 9.4%. He is on 3 medications for diabetes and now needs to start insulin. JR says, “I just don’t know if insulin would help me. My brother took insulin and he had all kinds of problems.”
What best describes JR’s stage of change using the transtheoretical model?
Answer Choices:
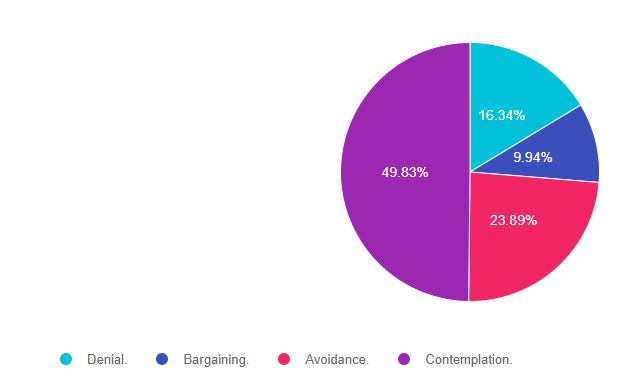
As shown above, the most common choice was option 4, the second most common answer was option 3, then option 1, and finally option 2
If you are thinking about taking the certification exam, this practice test question will set you up for success. Test writers anticipate possible answers based on the details in the question. They will wave those “juicy answers” right under your nose. Your job is to be familiar with the most common behavior change theories and taking a person-centered approach. Then weed through the particulars, pluck out the most important elements, the cross of false answers, and choose the BEST answer.
Answer 1 is incorrect. 16.34% chose this answer, ” Denial”. There are 5 stages of change in the transtheoretical model, and denial isn’t one of them. It is true that the person in the vignette may be experiencing some degree of denial, but denial is not one of the stages of change in this model. To throw test-takers off a little, I used terms from the “Stages of Grief” model, by Kubler Ross. This was intentional on my part, to lure you in with juicy, but incorrect, answers.
Answer 2 is incorrect. 9.94% of you chose this answer, “Bargaining”. There are 5 stages of change in the transtheoretical model, and bargaining isn’t one of them. As with answer 1, “Denial,” I used terms from the “Stages of Grief” model, by Kubler Ross. This was intentional on my part, to lure you in with juicy, but incorrect, answers.
Answer 3 is incorrect. 23.89% chose this answer, “Avoidance”. There are 5 stages of change in the transtheoretical model, and avoidance isn’t one of them. It is true that the person in the vignette may be experiencing some degree of avoidance, but avoidance is not one of the stages of change.
Finally, Answer 4 is correct, “Contemplation” 49.83% chose this answer. YAY. Almost half of you chose the correct answer. Based on the content, we can tell that JR is “thinking about it” or contemplating making a change. As educators, we will explore this ambivalence and focus on past successes to increase feelings of self-confidence in achieving the new behavior.
“I just don’t know if insulin would help me. My brother took insulin and he had all kinds of problems.”
Educators might then say, I hear what you are saying. You are not sure if insulin would help you since your brother had all kinds of problems. Can you tell me more about this?
As the story unfolds, it provides opportunities to honestly explore some of the benefits and drawbacks of insulin therapy and gives space for JR to talk about their experience with insulin.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!

Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]This time of year is my favorite. Seeing the beautiful colors of the fall harvest soothes and invigorates me. Being outdoors with my community is especially healing during this unusual and stressful time of isolation due to the pandemic.

I especially adore shopping and gathering fresh produce and other goodies from our local Farmers’ Market!
The farmer’s market is also a special place for me because my daughter works there. Her booth is overflowing with all the pumpkins and winter squash they have harvested. Last week, at the market, my daughter introduced me to her friend as they were talking about a pumpkin pie he had made from the pumpkin that he had purchased from her.
“Unfortunately, I can’t eat the pumpkin pie anymore because I was just diagnosed with having Type-2 Diabetes,” he explained.
I couldn’t help but tell him that I was a Dietitian and Diabetes Specialist.
We started talking about modifying the recipe using sugar substitutes or low carbohydrate crusts. We discussed portion control and going for a walk after eating a piece of the pie. He was intrigued.
Pumpkin and other winter squash do contain carbohydrates but are nourishing food. Benefits include:
It is important to take away the judgment around food choices, to encourage thoughtful choices, and find joy in our food. At this difficult time, every effort to empower ourselves with choice and joy is highly recommended.
Choose a pie pumpkin and wash it’s exterior. Cut in half lengthwise and remove the seeds and pulp. Roast in your oven for about 45 minutes at 350 degrees F.
Simply peel away the skin from the flesh and toss the pumpkin pulp into your food processor or blender.
Ingredients:
In a large bowl, whisk eggs and pumpkin puree together. Add the rest of the ingredients and whisk together while slowly pouring in the evaporated milk.
Pour mixture into pie crust.Bake in the oven for 20 minutes at 390 degrees, reduce oven to 350 degrees and bake for another 45 – 60 minutes until inserted toothpick comes out clean. Store in the refrigerator overnight.
Written by Dawn DeSoto RD, CDCES, our resident Nutrition Content Writer

Meet Dawn Desoto, our resident Nutrition content expert. Dawn has specialized in diabetes care for over twenty years.
As a diabetes specialist, Dawn provides individual and group coaching. Dawn launched a Diabetes Prevention Program in her community and provided plant-based cooking classes coupled with take-home recipes. The participants loved the helpful, delicious, easy-to-understand food demonstrations and recipes. But, a big motivation to keep coming to classes, was the fact that they felt celebrated and supported by the kind wisdom of Dawn’s approach.
In addition to her diabetes and nutrition expertise, Dawn loves to garden, cook, swim, bike and hike with her son and daughter. She also enjoys reading, traveling, and star gazing!
Please join me in welcoming my friend and colleague, Dawn Desoto, RD, CDCES

AJ is 89 years old with type 1 diabetes and is a caretaker for a partner with dementia. AJ is on an insulin pump and uses a meter to check blood glucose levels 4-7 times a day. AJ mentions that they were surprised the other morning that their blood glucose was 59 mg/dl and they felt fine.
Based on this, what is the best action?
Click here to test your knowledge!

Are you interested in learning about diabetes care for the frail and elderly? Then consider attending this all-day conference that synthesizes exciting findings and new elements that you can incorporate into your daily practice. Through dynamic presentations and case studies, we will provide you with creative strategies to take your practice to the next level. In addition, small group activities allow participants to network and share problem-solving strategies. The goal of this program is to provide cutting edge information that has real-life application. We want each participant to leave the seminar feeling more empowered and confident advocating for excellence in diabetes care.
Registration Price:
$20 for ADCES members – $40 for non-ADCES members – 6.5 CEs
Click here to register. – Download flyer here.
Who Should Attend?
This course is designed for all health care professionals including providers, nurses, dietitians, pharmacists, and educators who want to:
Requirements for Successful Completion: Participants should try to be in attendance for all three webinars, complete and submit the program evaluation at the conclusion of each webinar. Partial CE hours (2.25 CE hours) can be awarded per webinar if participants complete and submit the program evaluation. The three webinars will be recorded for later viewing but NO CE hours will be awarded for viewing of the recorded webinars.
Registration Price:
$20 for ADCES members – $40 for non-ADCES members – 6.5 CEs
Click here to register. – Download flyer here.
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.
Last year, during our campus tour at Santa Clara University, the docent took a moment to recognize and thank the Indigenous Peoples’ for the use of the land that we were gathered on.
“We pause to acknowledge that Santa Clara University sits on the land of the Ohlone and Muwekma Ohlone people. We remember their continued connection to this region and give thanks to them for allowing us to live, work, learn, and pray on their traditional homeland. We offer our respect to their Elders and to all Ohlone people of the past and present. “
Santa Clara University
I found this statement and acknowledgment to be very moving. It was the first time I had experienced a “Land Acknowledgment”. Since that time, I have heard it more frequently at events and gatherings.
Land Acknowledgement is defined as a formal statement that recognizes and respects Indigenous Peoples as traditional stewards of this land and the enduring relationship that exists between Indigenous Peoples and their traditional territories.
To perform a Land Acknowledgment, first, find out the history of the land you’re on.
In our town, Chico, CA, we acknowledge the land of the Mechoopda tribe.
As of today, 14 States and 130 cities celebrate Indigenous Peoples’ Day. Keep reading to find out other ways to recognize this important day.
The Smithsonian National Museum of the American Indian has compiled wonderful ideas on taking a moment to celebrate the lives and traditions of our lands’ first inhabitants.
Read more about this exciting and important topic on the Smithsonian Website.
Thank you for being a part of the diabetes community.
Coach Beverly and Bryanna
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]