
Subscribe
eNewsletter

Ready to get certified?
Free CDCES Coach App
Download
Free Med Pocket Cards

Our September 15th Question of the Week quizzed test takers on figuring out which lab test was most needed based on the case history.
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer below: Answer Question
Question: A 42-year-old woman arrives with an A1c of 10.3%, BMI of 32 and states she is ready to take better care of her type 1 diabetes. She uses a Freestyle Libre Sensor and takes 3-4 injections of insulin a day. Both her parents have type 2 diabetes and she says her diabetes was diagnosed after her third pregnancy. During this pregnancy, she had gestational diabetes and after delivery, her blood sugars never improved. Given this history, which of the following lab tests would clarify the best diabetes treatment plan?
Answer Choices:
As shown above, the most common choice was option 4, the second most common answer was option 2, then option 3, and finally option 1.
If you are thinking about taking the certification exam, this practice test question will set you up for success. Test writers anticipate possible answers based on the details in the question. Many of the test questions are presented as clinical vignettes. Your job is to weed through the particulars, pluck out the most important elements and choose the BEST answer based on the evidence.
Answer 1 is incorrect. 11% of you chose this answer, “A1c and OGTT”. Based on her history, presentation, and A1c of 10.3%, she clearly has established diabetes. So there is no need to verify diagnosis by rechecking her A1c or administering an OGTT.
Answer 2 is incorrect. 9% of you chose this answer, “Transglutaminase”. This blood test is indicated to evaluate if someone has celiac disease. It is true that people with type 1 are at high risks for autoimmune conditions like celiac disease. However, we can only use the information contained in the case study to determine the best answer. Since she is not complaining of any GI issues or exhibiting any symptoms of celiac disease, this is not the best answer.
Answer 3 is incorrect. About 8% of you chose this, “TSH and T4”. These test are used to evaluate the health of the thyroid. It is true that people with type 1 are at high risks for autoimmune conditions like thyroid disease. However, we can only use the information contained in the case study to determine the best answer. Since she is not complaining of or exhibiting any symptoms of thyroid disease in this situation, this is not the best answer.
Finally, Answer 4 is correct. 72% chose this answer, ICA, IAA, GAD”. In chosing this correct answer, we consider her BMI of 32, plus the fact that both her parents have type 2 diabetes and she had gestational diabetes. Plus after delivery, her blood sugars never improved. We are wondering if she might actually have type 2 diabetes? Given her genetic history and weight, we are certainly observing that she is exhibiting signs insulin resistance, and might benefit from the addition of medications (GLP-1 RA, SGLT-2, metformin) approved for people with type 2 diabetes.
To verify that she has type 1 diabetes, we look at lab results to check if there is an autoimmune attack on her pancreas and insulin. If one or more of these tests come back positive, it indicates an autoimmune condition.
ICA – Islet Cell Autoantibodies
IAA – Insulin Autoantibodies
GAD – Glutamic Acid Decarboxylase
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.

AR is a 39-year-old on an insulin pump and CGM. AR’s basal rates are:
AR’s insulin to carb ratio is 1:15 and the correction is 1:50 with a blood sugar target of 100-120.
When looking at AR’s report, they are bolusing for meals at 7 am, 12 pm, and 7 pm. AR is experiencing blood sugars of 60 -70 around 10 am and 3 pm every day.
Based on this data, what is the best recommendation?
Click here to test your knowledge!

In each webinar, either Coach Beverly, Dr. Isaacs, or Ms. Armstrong, highlight the critical content of each topic area, so you can focus your study time most efficiently. They also launch multiple poll questions to help participants focus on key concepts and assess their knowledge while learning the best test-taking strategies.
2020 Boot Camp Live Stream Webinar Schedule with Coach Beverly
All courses air at 11:30 a.m. (PST)
Can’t make it live?
No worries! All video presentations and podcasts will be available now on-demand.
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.
[yikes-mailchimp form=”1″]Today, let’s celebrate Supreme Court Justice Ruth Bader Ginsburg and consider the impact of her legacy on our lives.
In spite of a tough childhood filled with loss and numerous obstacles through her adult life, Ruth Bader Ginsberg (RBG) persevered and became a champion for equality. She believed that equal justice under the law should be applied to every single American, regardless of gender.
As a woman-owned business, I owe a debt of gratitude to this trailblazer. She demonstrated through her actions, that women are equally capable of taking leadership roles, running organizations, and being change agents.

She provides wisdom and guidance for diabetes specialists and advocates.
“Fight for the things that you care about, but do it in a way that will lead others to join you.” – RBG
As a Diabetes Care and Education Specialist for over twenty years, I have personally witnessed the positive changes our community has championed. From making sure recommendations are based on evidence to changing our approach from a compliance model to person-centered education. We have advocated for Medicare Coverage for the Diabetes Prevention Program and won approval.
In the spirit of RBG, we are taking a leadership role in promoting CV disease reduction and bringing technology and resources to underserved communities. We realize the importance of equitable diabetes care delivery and are raising awareness of the social determinants of health. We are breaking down barriers and lifting people up.
We have done all this through careful study, collaboration, research, kindness, and compassion.
Just like RBG, our Diabetes Community realizes we are in it for the long haul and big changes take time.
“Real change, enduring change, happens one step at a time.” – RBG
This determined woman instigated a revolution of thought and legislation. Not overnight, but with slow, methodical determination and intelligence and we are forever indebted to her.
Thank you, Ruth Bader Ginsburg. Even though you have passed, your fire burns brightly.
Coach Beverly
We received dozens of applications for our Making a Difference Scholarship. Even better, an anonymous donor generously contributed two additional scholarships, so we able to award four scholarships in total. Each scholar winner is awarded CDCES Deluxe Online Prep Bundle | 44+ CEs plus additional study tools (a value of over $450) to acknowledge their service.
It was a great personal joy for our team to read these scholarship applications. Each applicant is serving communities with a great need and going “above and beyond” to promote and provide accessible diabetes care and education. It is always a very difficult decision for all of the judges, and we read each application in careful detail considering the financial need, impact, volunteerism, and readiness to take the CDCES exam.
We greatly appreciate the good work of all the applicants and thank them for their service!
Making a Difference Scholarships

We are excited to recognize and reward diabetes advocates who are making a difference in their community while working toward certification (CDCES). In recognition of health disparities, this award considers health care professionals whose daily actions, volunteer activities and advocacy work is making a significant difference in improving the health of their people.
We are excited to announce our “Making a Difference” scholarship winners, Rachel Patton and Mercy Edziah.
Diabetes Educator Flower Scholarships awarded by a generous donor, this new annual Flower Scholarship awards two health care professionals who are taking a leadership role in making significant contributions to under-served communities through their work and volunteer activities. Two of our applicants are living examples of giving back to their communities and are recognized for their hard work, grit, and hope.
We are pleased to announce our Flower Diabetes Educator Scholarship winners, Alexa Guzman and Chinethia Johnson. Learn about the Flower Scholarship here.

Rachel Patton is a trailblazer and fierce advocate for those in need
Rachel works in a non-profit community health center where she serves primarily with people who are un/underinsured, have Medicaid, or Medicare. In her work, she supports people living with diabetes who have barriers in glucose control due to houselessness or depression.
?She has advocated for the accessibility of continuous glucose monitors and other supplies at no or reduced cost for those she works with, even taking the time to call pharmacies to find ways to make supplies more affordable. At community events and health fairs, she has offered her time and expertise to raise awareness about diabetes. She has also created recipe booklets with those in mind who have limited cooking utensils, for example, heart-healthy crockpot recipes that uses items like mugs or spoons to measure ingredients.

Mercy Edziah combines culture, food and cooking classes
Mercy volunteers at a local hospital where she is passionate about increasing her cultural intelligence while working with people living with diabetes from diverse backgrounds. There she leads group classes, peer-to-peer support groups, along with individual sessions.
?Mercy also brings her experience with agriculture and food service to support the hospital’s greenhouse that provides fresh produce for the hospital’s weekly farmer’s market and cooking classes offered in the hospital’s wellness center. In her practice, she individualizes her care plans that match each individual’s access and needs. She is an advocate and pillar of support for people living with diabetes within her community.
Alexa Guzman uses Food Pharmacy Prescriptions to promote health.
Alexa volunteers with her local church and other local health centers to empower her community through education on diabetes management and prevention. In her practice, she works with people who have poor social determinants of health, and little to no access to care.
She is passionate about food accessibility and has adopted the concept of a “Food Pharmacy.” In this practice philosophy, she prescribes food plans that anchor on individual access and that are culturally sensitive. She believes her recommendations should not be confined to only an ”American diet.” Her goal of becoming a CDCES will allow her to expand her impact of providing a high level of care that is realistic and obtainable to those within her community.
Chinethia Johnson is a volunteer extraordinaire.
For Chinethia, diabetes is a disease that holds a personal significance in her heart. Because of her experience with the first-hand impacts of diabetes, she is driven to provide education and support the those she holds dear.
Each month she spends over 40 hours volunteering her time and knowledge either in person, over Zoom or the phone, to people living with diabetes or those who want to learn more about prevention. Outside of the inspiring number of hours she spends each month volunteering, she also juggles being a case manager, a mother, and a grandmother, all while being in school working to obtain her masters in nursing.

Please enjoy these FREE resources that we have put together for you:
See Full Free Resource Catalog

Our September 8, 2020, Question of the week quizzed test takers on a complicated case study that asked what was the most important information to share with a person starting on a GLP-1 Receptor Agonist. Although 55% of respondents chose the correct answer, 45% did not. We thought that this was an important topic to discuss further, so we can pass on correct info to people living with diabetes.
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer below: Answer Question
Question: AJ takes 85 units of basaglar at bedtime and 10 -12 units of glulisine (Apridra) at meals, plus metformin and empagliflozin at maximum dose. Fasting blood sugars are 130 or greater and the rest of the day, AJs blood sugars are in the 200s. AJ has a BMI of 32 and an A1c of 9.3%. The diabetes specialist recommends adding semaglutide (Ozempic) 0.5 mg to the regimen. What teaching information is most important given the addition of this new medication?
Answer Choices:
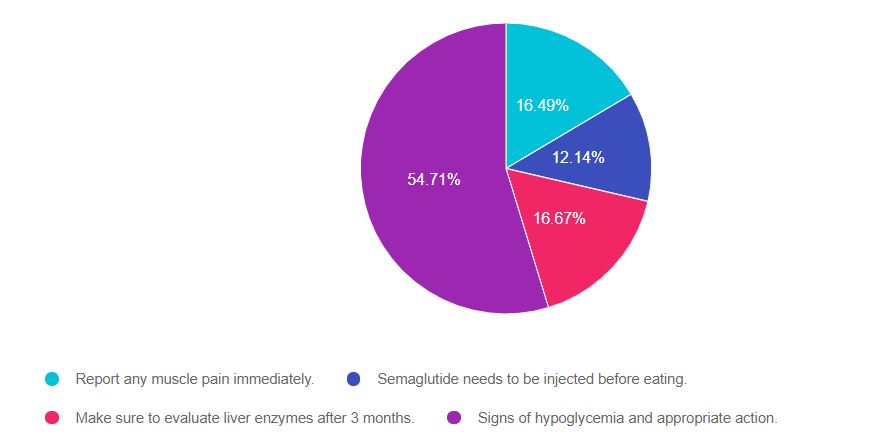
As shown above, the most common choice was option 4, the second most common answer was option 2, then option 3, and finally option 1.
If you are thinking about taking the certification exam, this vignette practice test question will set you up for success. Test writers anticipate possible answers based on the details in the question and common knowledge. They will wave those “juicy answers” right under your nose. Your job is to weed through the particulars, pluck out the most important elements, eliminate false answers and choose the BEST answer.
And you may want to Download our Medication PocketCards for detailed info on the available diabetes meds.
Answer 1 is incorrect. 17% chose this answer, “Report any muscle pain immediately”. This is a juicy answer. It is true that statins, the medication class used to manage lipids in diabetes, can cause muscle pain. But, the medication being added, semaglutide (Ozempic), is a GLP-1 Receptor Agonist, not a statin. Its main side effects includes nausea and loss of appetite, but muscle pain is not a common side effect of GLP-1 Inhibitors. This answer is false.
Answer 2 is incorrect. 12% of you chose this answer, “Semaglutide needs to be injected before eating”. This is another juicy answer. There are 2 forms of semaglutide. One is Ozempic, it is a once a week injection. People taking this injectable version, do not need to inject on an empty stomach. However, the oral form of semaglutide (Rybelsus), does need to be taken on an empty stomach with only a sip of water (See our Medication PocketCard for more details).
Answer 3 is incorrect. About 17% of respondents chose this, “Make sure to evaluate liver enzymes after 3 months”. It is true that we monitor liver enzymes for people with diabetes if they are on statins or to help screen for fatty liver disease. However, this GLP-1 Receptor Agonist has no indication to monitor liver enzymes after starting treatment.
Finally, Answer 4 is correct. 55% chose this answer, “Signs of hypoglycemia and appropriate action”. Yes, this is the BEST answer and it was a little tricky. Semaglutide (Ozempic), is a GLP-1 Inhibitor and does not cause hypoglycemia. However, this person is on a 85 units of basal insulin daily, plus 10 -12 units of bolus insulin at meals. With the additional glucose lowering impact of the GLP-1 Receptor Agonist, they are at risk of hypoglycemia from the insulin. Many people actually require a decrease in their insulin dose when adding on or increasing the dose of a GLP-1 RA.
Download our Medication PocketCards for detailed info on the available diabetes meds.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!

In each webinar, either Coach Beverly, Dr. Isaacs, or Ms. Armstrong, highlight the critical content of each topic area, so you can focus your study time most efficiently. They also launch multiple poll questions to help participants focus on key concepts and assess their knowledge while learning the best test-taking strategies.
2020 Boot Camp Live Stream Webinar Schedule with Coach Beverly
All courses air at 11:30 a.m. (PST)
Can’t make it live?
No worries! All video presentations and podcasts will be available now on-demand.
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.
[yikes-mailchimp form=”1″]Over 50% of people living with diabetes have fatty liver disease.
Over the next 20 years, non-alcoholic steatohepatitis (NASH) and type 2 diabetes will account for 65,000 transplants, 1.37 million cardiovascular-related deaths, and 812,000 liver-related deaths.
These statistics are from a 2020 article in Diabetes Care, Economic and Clinical Burden of Non-alcoholic Steatohepatitis in Patients With Type 2 Diabetes in the U.S.
Fatty liver disease is increasingly recognized as the hepatic manifestation of metabolic syndrome. Currently, there is no effective approved medical therapy to fix the fatty liver disease, management depends on lifestyle changes, such as weight loss and increased exercise.
About 34 million people in the U.S. have type 2 diabetes. Of those, over half are also living with liver disease.
In the U.S. in 2019:
Given the high rate of liver disease in people with diabetes, I have been paying more attention to our client’s liver enzymes levels, including alanine aminotransferase (ALT) or aspartate aminotransferase (AST). Elevated levels of these liver enzymes indicate inflammation and a potential pathway to liver disease progression.
After discovering elevated enzymes, we send them for further diagnostic testing to evaluate the extent of liver disease. The question is, should we make liver health screening a part of our usual diabetes practice?

According to a recent article in Gastroenterology, screening for non-alcoholic fatty liver disease (NAFLD) followed by lifestyle modification among people with type 2 diabetes can be cost effective.
In a recent study, a team of researchers used a hypothetical cohort of people age 55 years with type 2 diabetes and developed a model that compared screening and treatment with no such protocol.
For the virtual intervention group, they measured ALT or AST and provided an ultrasound scan. If these tests came back positive for NAFLD, the participants underwent further screening with liver biopsies and transient elastography.
People found to have NASH with Stage 2 entered a year-long behavior program to help them with weight loss and lifestyle changes. They found the for participants with stage 2 fibrosis or higher, the screening and lifestyle intervention was just as cost-effective compared to the group with no screening.
“Our results indicate the potential value and cost-effectiveness of NAFLD screening” in people with type 2 diabetes, wrote the study authors. “Given the increasing burden of NAFLD/NASH and the expected rapid increase in approved medications, we recommend screening patients with type 2 diabetes for NAFLD.”
Click this link to read more about Screening People with Type 2 for Liver Disease.

People with cancer often experience hyperglycemia secondary to treatment, which can increase risk of infection and compromise their nutritional status. In addition, recent research has identified the link between diabetes and cancer. Join us to learn more about this unexpected link and treatment strategies for steroid-induced hyperglycemia using a case study approach.
Topics Include:
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.
[yikes-mailchimp form=”1″]
A 42-year-old woman arrives with an A1c of 10.3%, BMI of 32 and states she is ready to take better care of her type 1 diabetes. She uses a Freestyle Libre Sensor and takes 3-4 injections of insulin a day. Both her parents have type 2 diabetes and she says her diabetes was diagnosed after her third pregnancy. During this pregnancy, she had gestational diabetes and after delivery, her blood sugars never improved.
Given this history, which of the following lab tests would clarify the best diabetes treatment plan?
Click here to test your knowledge!

In each webinar, either Coach Beverly, Dr. Isaacs, or Ms. Armstrong, highlight the critical content of each topic area, so you can focus your study time most efficiently. They also launch multiple poll questions to help participants focus on key concepts and assess their knowledge while learning the best test-taking strategies.
2020 Boot Camp Live Stream Webinar Schedule with Coach Beverly
All courses air at 11:30 a.m. (PST)
Can’t make it live?
No worries! All video presentations and podcasts will be available now on-demand.
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.
[yikes-mailchimp form=”1″]We are excited to announce the new Diabetes Flower Scholarship. We are awarding one of these scholarship this year, valued at $1000. This scholarship is available due to the generous contribution of an anonymous colleague, friend, co-instructor, and mentor.
Our donor worked as a Nurse Practitioner and Diabetes Specialist, serving her community, plus mentoring health care professionals about diabetes for over 30 years.
With the Flower Diabetes Educator Scholarship, she wants to keep investing in the health of our future by supporting future diabetes educators.
Her vision is to increase diversity in the diabetes education workforce by supporting diabetes nurse educators who come from under-served communities. By increasing the number of diabetes educators who represent the population demographics of those living with diabetes, we can make more meaningful connections on an individual and community level while promoting best care.
To be eligible for these scholarships, the U.S. health care professional is a diabetes nurse educator who comes from an under-served community and is providing care and education to communities that lack access to Diabetes Specialists and health care resources. Applicants will also be working toward certification (CDCES) within the next year and preference is given to those facing financial hardships that are interfering with their ability to pursue this dream.
The Flower Scholarship is valued at $1000 and includes:

The Flower Scholarship is a tribute to our donor’s last name, which translates to flower. The flower is a perfect symbol for this scholarship that aims to support the growth of novice diabetes educators into Certified Diabetes Care and Education Specialists.
Flowers are a symbol of hope and can be found growing in the most unexpected places, including harsh cities and forgotten spaces. With just a little sunlight and water, they have the ability to thrive in even the most difficult situations and shine their fierce beauty. Given a chance, as these flowers are tended to and nurtured, they grow stronger and brighter, spreading their beauty to new places to give people hope. These resilient flowering seeds perpetuate the opportunity for a future generation of diabetes specialists.