
Subscribe
eNewsletter

Ready to get certified?
Free CDCES Coach App
Download
Free Med Pocket Cards
How long does glulisine last in pumps? What insulins can people buy without a prescription? What is the longest lasting insulin? If you want to learn the answers to these questions an more, we are here to help!
With the pandemic and ongoing insulin pricing issues, many people are struggling to pay for their insulin. Armed with information, we can help people maximize their insulin use and optimize their choices.
By knowing how long different insulin formulations last when kept at room temperature (temps up to 86 degrees), we can help people use their insulin as long as it is safe and recommended.
We usually say insulin is good for about 28 days. This is correct for many insulins, but not all.
For example, a vial of Human Regular insulin is good at room temp for 42 days. Degludec (Tresiba) is good for 56 days and Novolin 70/30 vial is good for 42 days. Glulisine (Apidra) expires after 2 days in an insulin pump, but lasts for 28 days in a vial.
See our new and exciting Insulin Storage Cheat Sheet for all kinds of important details on storage and more!
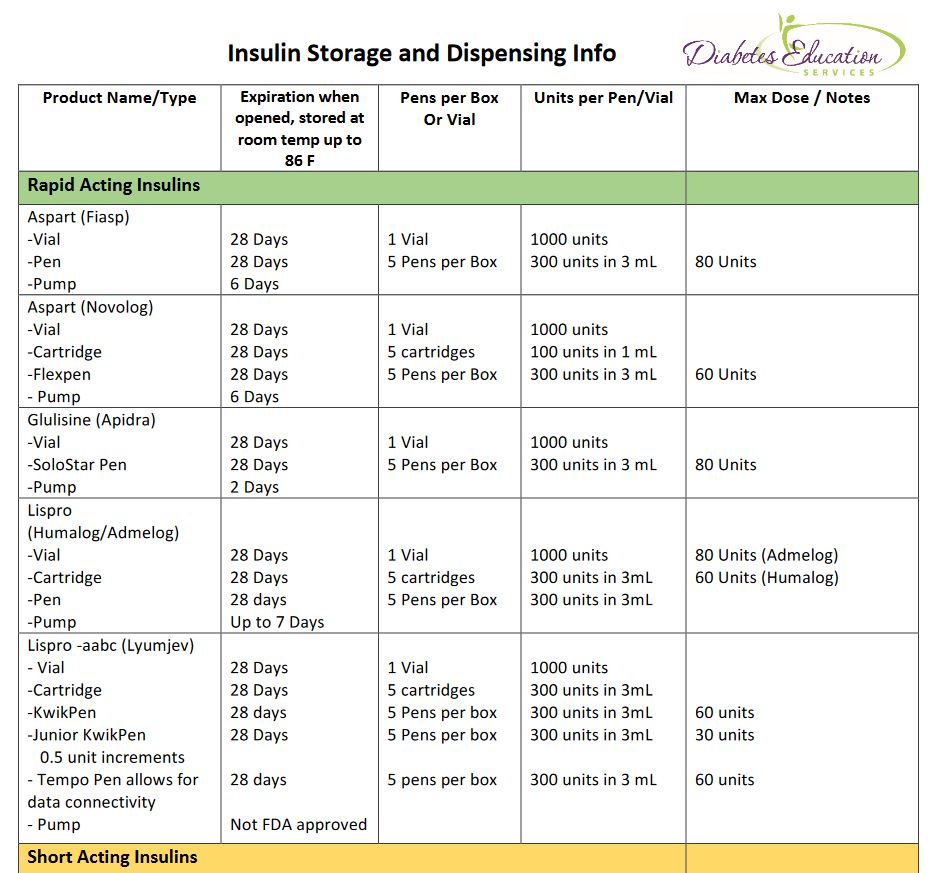
In addition, did you know that there are 3 insulins that do not require a prescription in most states? Regular, NPH and Regular/NPH combo insulins require no prescription.
A recent client ran out of their aspart insulin, was low on cash and out of town. They walked into a local Walmart, without a prescription, and paid $25 cash for a vial of regular insulin. This is incredibly important information to share with clients as a back up in case of emergency.
How many times have you launched into a google search or scoured insulin package inserts to find out the following questions or something like it?
Our Insulin Storage Cheat Sheet answers these questions and more!
Special thanks to Jackson Thomassian for compiling the first drafts of these sheets and to Diana Isaacs, PharmD for her inspiration.
Even though Coach Beverly has reviewed and edited these sheets dozens of times, she knows there is always room for improvement. Please let us know if you see content that needs updating. In appreciation, Beverly


AL was recently started on an insulin pump. AL’s insurance company will only cover glulisine (Apidra) insulin for the pump. Before starting pump therapy, AL thought they only needed to change the pump site every three days. AL is frustrated to find out that since they are using glulisine (Apidra), they will need to change the insulin cartridge and site every 2 days.
What is the best solution to AJ’s frustration?
Click here to test your knowledge!
Try our Test Taking Toolkit!
$49 | 220+ Questions
In this course, Coach Beverly details the content of the exam and test-taking tips. Plus, she reviews a sampling of the questions, and explains how to dissect the question, eliminate the wrong answers and avoid getting lured in by juicy answers.
Enroll Now!
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.
The InPen smartpen, by Companian Medical, is now FDA approved for all ages!
The Inpen is a reusable battery-powered insulin pen that uses insulin cartridges. It is approved for use with three different insulins; Novolog, Humalog, and Fiasp. It can deliver insulin in half-unit doses plus it monitors insulin temperature. The battery lasts for a year and requires no charging.
“We are excited that we can help younger children and even more parents navigate the challenges associated with Type 1 diabetes. Now anyone can safely use InPen to help make decisions around insulin dosing, no matter what their age,”
Sean Saint, CEO and co-founder of Companion Medical.
In addition to all these features, the InPen Bluetooth enabled software allows users to connect to a FREE app on their Apple iOS or Android mobile device to track and share insulin dosing and glucose levels.
New users enter their insulin to carb ratios and insulin sensitivity along with target glucose into the app settings. Based on that data, the software helps to calculate the insulin dose needed and alerts users to insulin on board to prevent stacking (which can help reduce hypoglycemia.)
People can use Inpen in combination with CGM or traditional glucose monitoring and reports can be shared with providers and caretakers
Here is what InPen users can track on the app dashboard:
The InPen requires a prescription and is covered by many insurance companies in the United States. Most InPen users pay a $35 copay. Companion Medical has a co-pay assistance program for people without insurance coverage – more info here.
As a Diabetes Specialist, I am excited to share information on these new and emerging options to deliver insulin therapy that reduce the burden of diabetes self-management and improve connections to caregivers and providers.
Thanks for reading our Tech Thursday Blog! More info on InPen Here .
Can cinnamon help maintain glucose in those with prediabetes?

There have been several studies over the past decade to determine the efficacy of using cinnamon supplements to regulate blood sugars. Most of the studies found either no significant change or slight changes.
For example, a 2013 study of 70 different participants found that those who took 1 gram of cinnamon daily showed no significant changes over 30 or 60 days.
However, a recent study found that cinnamon supplements may be beneficial over time for improving glucose homeostasis in prediabetes.
This study, conducted by Giulio R. Romeo, MD, from the Joslin Diabetes Center in Boston, and Dr. Romeo’s colleagues spanned over 12 weeks across 45 participants who met the criteria for prediabetes. These participants, who were not taking a placebo, took 500mg of cinnamon supplements a day to see the impact on glucose control.
From a similar baseline, FPG rose after 12 weeks with placebo but remained stable with cinnamon, leading to a mean between-group difference of 5 mg/dL (P<0.05). When compared to the respective baseline, cinnamon, but not placebo, resulted in a significant decrease of the AUC PG (P<0.001) and of the 2-hr PG of the OGTT (P<0.05). There were no serious adverse events in either study group.
Their study found that fasting plasma glucose (FPG) rose for those who took the placebo. For those who took cinnamon supplements, their area over the curve (AUC) plasma glucose (PG) decreased along with their 2 hour PG by oral glucose tolerance test (OGTT).
The results suggest that over time, a cinnamon supplement of 500mg a day may help blood glucose levels for those with prediabetes.
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.

RJ is 67 years old with a 40+ year history of type 1 diabetes. GFR is 62, UACR is < 30, A1c is 6.7%, B/P is 132/72, LDL cholesterol is 98, his BMI is 28.6. RJ uses multiple daily injections and CGM to manage his diabetes.
RJs other medications include: Levothyroxine 100mcg daily, atorvastatin 40mg daily, Aspirin 81 mg daily and a multivitamin.
Based on your assessment, which of the following interventions would improve RJs outcome?
Click here to test your knowledge!
Here at Diabetes Education Services, we are excited to celebrate World Breastfeeding Week!

Breastfeeding reduces the risk of future diabetes for mom and baby alike. Studies show that mothers who nursed babies for at least six months were 48 percent less likely to develop diabetes. Yet many mothers, who want to breastfeed, aren’t able to due to a variety of obstacles.
There are myriad benefits to breastfeeding, a fact that’s well-endorsed by upcoming World Breastfeeding Week. This event, which is sponsored by the World Alliance For Breastfeeding Action, focuses on promoting, protecting, and supporting breastfeeding around the globe.
“There could be greater health benefits for women from breastfeeding than previously recognized,” said lead study author Erica Gunderson of the Kaiser Permanente Division of Research in Oakland, California.
Each year, a new adjacent cause is championed; this year, the climate impact of formula feeding is central to the week-long event. Wisely, the organization makes a point to reflect on breastfeeding inequality as a series of obstacles that must be overcome in order to truly reap the ecological benefits of making this switch.
Below is an infographic that describes the critical issues surrounding breastfeeding inequalities that bring to light an often under-discussed issue. Blog also continues below.
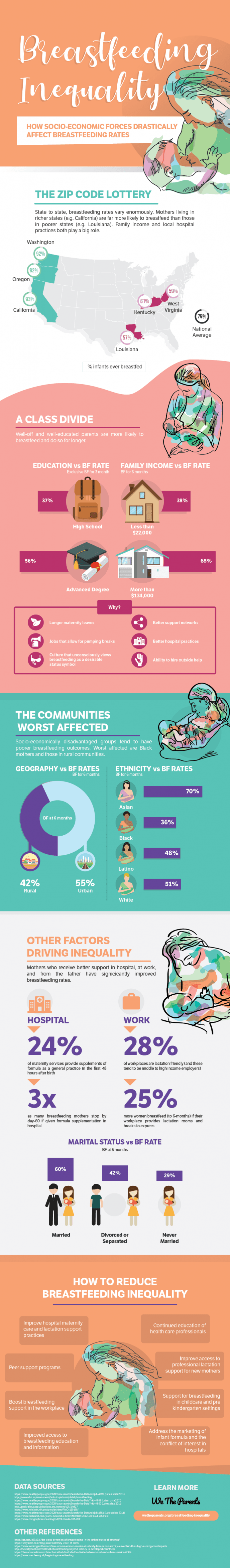
Breastfeeding inequality refers to the disparity in breastfeeding rates that can be observed in socioeconomically disadvantaged areas. Even in developed countries like the United States, demographic areas that fall beneath the poverty line often reveal dismal statistics when it comes to breastfeeding. This visualization breaks down the impact of income, education, and other lifestyle factors on breastfeeding inequality:
For those who’ve simply been watching moms go back and forth online about choosing breast or bottle, learning that some mothers are at a legitimate disadvantage when it comes to breastfeeding can be shocking. Factors like income and partner support play a direct role in the home, but there are other reasons why breastfeeding rates in economically disadvantaged areas are low.
Optimum nourishment at no cost, improved parental bonds, and the possible prevention of future allergies, asthma, obesity, and type 2 diabetes are but a few of the reasons that breastfeeding equality is essential for all families. Though the fight is hard-fought, the health of a generation is a goal worth uniting for.
Written by Guest Writer, Neve Spicer, Founder & Director at Wetheparents.org
Resources

A committee of experts provides recommendations for healthy eating twice every decade. These final recommendations are sent to the US Department of Health and Human Services and the US Department of Agriculture, which use them to create the final 2020 dietary guidelines for Americans.
For the first time ever, the panel is including nutrition guidelines for infants 2 years and younger, with a pointed focus on reducing sugar consumption.
On average, infants consume a teaspoon of added sugar a day while toddlers consume about 6 teaspoons a day.
“Nutritional exposures during the first 1,000 days of life not only contribute to long-term health but also help shape taste preferences and food choices.”
2020 Dietary Guidelines Report
The committee also recommended further reductions in sugar intake for those age 2 and beyond. They also suggested less alcohol for men.
Read more about the 2020 Dietary Recommendations

Visit our Joy of Six Resource Page which has handouts and other helpful info on strategies to decrease sugar intake.

As a Diabetes Specialist in a rural clinic, you are asked to consult on a 49-year-old female with type 2 diabetes and a BMI of 27. Blood pressure is 132/74 with the following lab values; A1c of 7.6%, LDL of 97 mg/dl, triglycerides 138, and GFR of 69. Her medications include:
Metformin 850 mg three times a day, levothyroxine 100 mcg a day, and cetirizine 10mg daily.
According to the ADA Cardiovascular Standards of Care, what other medication therapy needs to be added?
Click here to test your knowledge!