
Subscribe
eNewsletter

Ready to get certified?
Free CDCES Coach App
Download
Free Med Pocket Cards
Disclaimer: We always strive to give accurate information with our blogs. For this article, we discovered we need to dig deeper into this topic to make sure we got it absolutely right. If you have any information on this content, please click here to visit our survey to update us.
We have positive news to share for people with diabetes who are on insulin and would like to use a CGM (Continuous Glucose Monitor)!
The Center for Medicare and Medicaid Services (CMS) is relaxing some of their stringent requirements for obtaining a CGM during the COVID-19 pandemic.

“CMS will not enforce certain clinical criteria in local coverage determinations that limit access to therapeutic continuous glucose monitors for beneficiaries with diabetes. As a result, clinicians will have greater flexibility to allow more of their diabetic patients to monitor their glucose and adjust insulin doses at home.”
CMS just announced they would not enforce certain clinical criteria for obtaining a CGM, insulin pump, or associated supplies during the pandemic. For example, in-clinic provider visits, certain lab tests like a C-peptide or antibody testing, and demonstrations of SMBG would not be mandatory.
This is huge for people with diabetes!
It would limit visits to hospitals, clinics, and labs and help reduce exposure to the coronavirus at these public facilities.
Since CGM’s and insulin pumps have the ability to transmit the collected data to a provider for a telehealth consult, providers can now use that data to review during telehealth visits. This can strengthen the relationship during COVID by allowing for data-driven insulin adjustments.
This is a win-win situation and we can hope that private insurance companies will follow the lead of CMS for the benefit of people with diabetes who use insulin.
To learn more read diaTribe’s article and visit CMS.gov.
Written by Catherine Cullinane RN, CDCES, our resident Tech Thursday Content Writer
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.
As Diabetes Specialists, we want to ensure the safety of patients and colleagues, while providing diabetes care to those who may be the most vulnerable and isolated during this pandemic.

According to the CARES Act, Diabetes Self-Management Training (DSMT) can be provided to patients via telehealth during the pandemic. Though the original regulations had many gaps.
Previously, the CARES Act required that telehealth visits must include both audio and video, while many hospital outpatient clinics were running into billing barriers. In addition, under the original guidelines, RNs and Pharmacists were not included in the approved list of telehealth DSMT Providers.
See: ADCES Summary Sheet of DSMT and Telehealth FAQ for more information.
Though as of April 23, 2020 the guidelines have been updated.
Good News – these updates to the CARES Act now expand blanket waivers under the 1135 waiver.
For any of the information below, please check with your compliance team for clarification and share the important resource links below with your billing department.
DSMT services may be billed for audio-only, but only if the video is not available or possible. Make sure to document the mode of instruction and the rationale if using audio-only.
See: COVID-19 Emergency Declaration Waiver for more information.
The ADA and ADCES have been working hard to decipher the language and intent in the updated guidelines. It seems that RN and Pharmacists are now included based on an assessment of the wording in the new documents. CMS continues to expand the definition of providers eligible to furnish telehealth services during the COVID-19 public health emergency.
As DSMT programs bill as an entity, rather than at the individual provider level, the American Diabetes Association is seeking confirmation that DSMT programs that are eligible through Medicare Part B, are considered distant site practitioners approved to furnish telehealth services.
See: Blanket Waivers for HealthCare Providers Fact Sheet for more information.
Hospital-Based Programs Can Bill for Telehealth DSMT on the UB-04 (Medicare Claims) Form
Hospitals may now bill for education and management services (i.e. DSMT) as if they were furnished in the hospital and consistent with any specific requirements for billing Medicare in general, including any relevant modifications in effect during the COVID-19 PHE.
In summary:
See: CMS Hospitals Without Walls Initiative for more information.
Important to note: Please consult with your organization’s billing department and compliance team if you have questions.
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.

LS is a 16-year-old with type 1 diabetes for the past 3 years. The most recent A1c is 9.3%. LS covers carbs using a 1:15 carb/insulin ratio and takes basal insulin at night. After the parents leave the room, LS tells you they are so tired of checking blood sugars and taking insulin four times a day, sometimes they just “fake it.”
What is the most appropriate action?
Click here to test your knowledge!
Join Diana Isaacs, PharmD, BCPS, BC-ADM, BCACP, CDCES, and ADCES 2020 Diabetes Educator of the year as she reviews these important topics. As Diabetes Specialists, we are tasked with taking a leadership role in technology and cardiovascular risk reduction. Dr. Isaacs will address these topics with clinical insight and expert knowledge during these two virtual courses.
Session 1 | CV Risk Management with Pharmacology and Intensive Insulin Therapy | Recorded & Ready for Viewing!
Session 2 | Continuous Glucose Monitoring and Insulin Pump Therapy | Recorded & Ready for Viewing!
Objectives:
$69 | Earn 4 CEs
These sessions are also included in our Virtual Conference.
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.

Written by Diana Isaacs, PharmD, BCPS, BC-ADM, BCACP, CDCES & ADCES 2020 Diabetes Educator of the year
The cost of insulin is a real problem. It can lead to insulin rationing and at its worst, people have died due to a lack of insulin.
A recent survey reported that 26% of respondents living in the US rationed insulin at last once in the last year.
The retail price for a box of insulin pens is about $500. Many people need more than one box of pens per month. Even with health insurance, people struggle to afford this. I remember one of my patients telling me she was only taking half of her prescribed dose of insulin glargine because her daughter was taking the same insulin and they both needed it. This just broke my heart!
Fortunately, the Food and Drug Administration (FDA), as well as drug companies, have heard the outcries from people who require insulin to live. In response, there are some helpful new programs that make insulin more affordable. However, it can be difficult to navigate all of the new information. To help make navigation easier, we have created an ADCES Access & Affordability page with Insulin Cost-Savings Resource Guide.
Insulin is considered a Biologic Drug, which makes it more expensive to produce.
Insulin is made from recombinant DNA technology, making it a biologic drug. Biologic drugs depend on unique manufacturing conditions that are proprietary and difficult to exactly replicate. Therefore, when the drug brand name patent expires, other companies can’t make true generics.
Until recently, the pathway for approval was called a follow-on biologic. This is how Basaglar (insulin glargine) and Admelog (insulin lispro) are classified. In March 2020, the FDA announced that regulatory requirements would change allowing for biosimilar products. This may ultimately increase market competitiveness in hopes to further reduce insulin prices. Basaglar and Admelog offer about a 15-20% discount from their reference products of Lantus and Humalog, respectively. Many argue these cost savings is just not enough.
Because insulin is a biologic drug, a true generic must come from the same manufacturer. Recently Lilly and Novo Nordisk have created generic insulins.
Lilly offers generics of insulin lispro, insulin lispro mix 75/25, and insulin lispro junior kwik pen.
Novo Nordisk offers generics of their insulin, which they are calling a “follow on Brand” and includes insulin apart and insulin aspart mix 70/30.
Both Lilly and Novo offer approximately a 50% cost savings from the original insulin product and the pharmacist can make an automatic substitution if you ask.
Walmart and some other pharmacies also offer ReliOn insulins. These include Novolin R, Novolin N, and Novolin 70/30. These are slower acting insulins that may predispose people to more hypoglycemia, but they are only $25/vial or $44/5 pack of pens and do not require a prescription in most states. Access to these insulins can be truly life-saving in some circumstances. Every person with diabetes needs to be aware that they can purchase these insulins without a prescription if they are ever out of insulin.
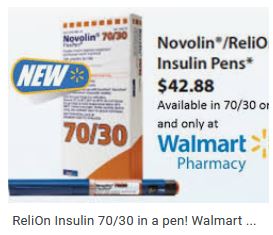
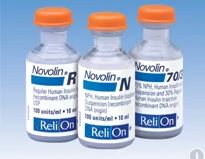
Lilly announced a program capping insulin co-pays at $35/month for those paying with cash or commercial insurance. This will dramatically lower monthly costs for many people with diabetes.
Sanofi has a Valyou program that allows up to 10 vials or 10 boxes of insulin pens for a maximum of $99/month. Of note, Sanofi’s program will only work for those without insurance.
Novo Nordisk recently started the My $99 insulin program. What’s unique about this program is that it will work for those with commercial insurance or government plans like Medicare. Most other programs exclude people with Medicare. This program covers up to 3 vials or 2 packs of pens.
Most insulins offer a co-pay card which can bring down the price of insulin most commonly to $0 to $25/month depending on the manufacturer and type of insulin. For any person with a commercial insurance plan, it’s good to check if a co-pay card is available for the insulin before picking it up from the pharmacy.
The things to be aware of about these cards are that they have maximum savings and sometimes that is much less than the total cost of the insulin. Also, they only work for people with commercial insurance meaning they won’t for people without health insurance or that have a government insurance plan like Medicare. They also do not always work if the drug is not covered on the insurance plan. In that case, it would be preferable to switch to an insurance-covered on the insurance plan.
These are programs offered through pharmaceutical companies for people without health insurance or that have Medicare but still struggle to pay for medications. There are various income requirements to be eligible, but depending on the program it can be 250-400% above the Federal poverty line. Many people are surprised to find that they are eligible, so this is a good option to look into which can make the insulin completely free. There is typically a packet of information that needs to be completed and then if eligible, the insulin is shipped to the prescriber’s office for the patient to pick up.
In summary, It can be challenging to keep all of this information straight. This is why I worked with a team of amazing diabetes care and education specialists at ADCES to create the ADCES Access & Affordability page with Insulin Cost-Savings Resource Guide. We update this resource frequently and it includes links to patient assistance programs, co-pay cards, and other cost savings programs. We hope you find it useful and that your patients with diabetes will benefit.
Conner F, Pfiester E, Elliott J, Slama-Chaudhry A. Unaffordable insulin: patients pay the price. The Lancet Diabetes & Endocrinology 7 (10), 748,2019.
For a summary of all this information, see the ADCES Insulin Cost Savings Resources Page.
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.
Click here to read our entire May Newsletter

As a Diabetes Nurse Specialist in a local clinic, I am providing telehealth once a week. During these visits, I am checking in with people about their food and medications.
Do you have enough food and insulin to last? Most of them answer, “yes, for now”.
Many of them may run out of insulin and supplies in the near future, some as a result of the costs that make essential medications in-affordable. If this is the case, what can we offer them?
We are excited to thank our guest contributor and Diabetes Educator of the Year, Dr. Diana Isaacs, who has provided us with helpful information and a multitude of resources for people in need of low-cost insulin.
In light of the COVID-19 emergency, the Centers for Medicare & Medicaid Services (CMS), has expanded opportunities to provide remote care to people with diabetes. We have highlighted some recent updates and provided links to helpful resources for your billing team.
Lastly, we are looking towards the future with salivary glucose testing and insights into a past Question of the Week.
I am grateful to be a part of this amazing community of diabetes specialists. Thank you for your care, concern and advocacy.
Be well! Coach Beverly
Click here to read our entire May Newsletter
Join Diana Isaacs, PharmD, BCPS, BC-ADM, BCACP, CDCES, and ADCES 2020 Diabetes Educator of the year as she reviews these important topics. As Diabetes Specialists, we are tasked with taking a leadership role in technology and cardiovascular risk reduction. Dr. Isaacs will address these topics with clinical insight and expert knowledge during these two virtual courses.
Session 1 | CV Risk Management with Pharmacology and Intensive Insulin Therapy | Recorded & Ready for Viewing!
Session 2 | Continuous Glucose Monitoring and Insulin Pump Therapy | Recorded & Ready for Viewing!
Objectives:
$69 | Earn 4 CEs
These sessions are also included in our Virtual Conference.
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.

“Scientists have been in search of a more cost-effective, non-invasive, and accurate diabetes monitoring alternative to blood sugar testing.”
Is there a better way to check blood glucose than uncomfortable fingersticks?
For people with diabetes who use self-management of blood glucose (SMBG) to monitor diabetes progress, fingersticks can wear on one’s fingertips, emotional well-being, and bank account.
Even continuous glucose monitors (CGMs) that provide around-the-clock glucose information and reduce the need for fingersticks, help with finger fatigue. But for many, they are not an affordable option.
Is there another option to check one’s glucose that is less painful and accurate?
“Lab tests of the saliva process have shown promising results with an accuracy rate of 95.2%. The research has been published in the journal PLOS ONE,” wrote Dr. Kamal Kant Kohli for Medical Dialogues.
Currently, companies like iQ Group Global and GBS inc. are developing Saliva Glucose Biosensors. This biosensor is a small strip that once matched with someone’s saliva offers an immediate glucose check and sends the results to an app on one’s phone.
Once these new systems are approved, it will be a game-changer.
Though saliva-based glucose testing has not yet hit the markets, for the millions of people that continue to perform finger sticks, we hope that saliva glucose testing will be available soon.
To read more, click here or visit iQ Group Global and GBS Inc websites.
Written by Catherine Cullinane RN, CDCES, our resident Tech Thursday Content Writer
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.

As a very sick patient in his 20s, Pope Francis, has personally experienced the importance of nurses. “You are there all day and you see what happens to the patient. Thank you for that!” he continued, “many lives, so many lives are saved thanks to you!”
He emphasized the importance of the nursing profession and their unique relationships with all members of the healthcare team – patients, families, and colleagues. Pope Francis stated that nurses are at “the crossroads” of all these relationships.
The Pope described the sensitivity nurses acquire from “being in contact with patients all day,” and acknowledged the healing power of listening and touch. Calling touch an important factor for demonstrating respect for the dignity of the person.
Nurses provide care despite the patient’s societal status. The Pope described the nurse’s care as particularly important in situations that may often leave weaker people on the margin.
Furthermore, Pope Francis acknowledged the “truly irreplaceable” role nurses play in the lives of their patients. “Like no other, the nurse has a direct and continuous relationship with patients, takes care of them every day, listens to their needs and comes into contact with their very body, that he tends to,” stated Pope Francis.
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]
JR is 49 with type 2 diabetes and is admitted to the hospital for congestive heart failure. His home diabetes medication includes metformin 2000 mg daily. GFR is 53 and JR’s A1c is 8.1%.
Upon discharge, which class of medication is recommended, according to the AACE Guidelines, in addition to the metformin to improve outcomes?
Click here to test your knowledge!
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]