
Subscribe
eNewsletter

Ready to get certified?
Free CDCES Coach App
Download
Free Med Pocket Cards

eNewsletter

Free CDCES Coach App
Free Med Pocket Cards
For last week’s practice question, we quizzed participants on checkpoint inhibitors triggering hyperglycemia. 34% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it by clicking here.

Betty, a 60-year-old female, is receiving pembrolizumab, an immune checkpoint inhibitor, as treatment for melanoma. She is worried about the potential adverse effects. She is very concerned about the risk of developing diabetes. Her recent lab work shows normal fasting blood glucose and hemoglobin A1c.
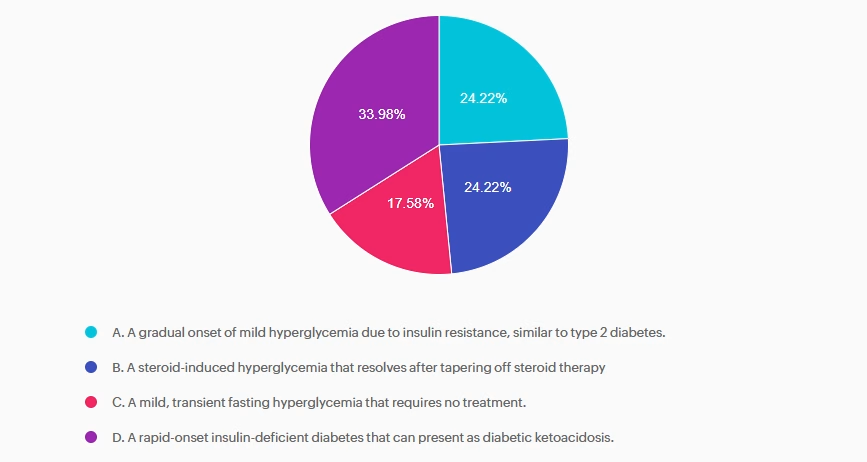
Answer 1 is incorrect. 24.22% chose this answer, “A gradual onset of mild hyperglycemia due to insulin resistance, similar to type 2 diabetes.” This answer is incorrect. Immune checkpoint inhibitor medications do not cause mild hyperglycemia but instead cause significant hyperglycemia and DKA similar to type 1 diabetes.
Answer 2 is incorrect. 24.22% of you chose this answer, “A steroid-induced hyperglycemia that resolves after tapering off steroid therapy.” This answer is incorrect. Though steroid treatment is often needed, hyperglycemia in immune checkpoint inhibitor-associated diabetes is not resolved after tapering off steroids.
Answer 3 is incorrect. About 17.58% of respondents chose this: “A mild, transient fasting hyperglycemia that requires no treatment.” This answer is incorrect. Though steroid treatment is often needed, hyperglycemia in immune checkpoint inhibitor-associated diabetes is not resolved after tapering off steroids.
Finally, Answer 4 is correct. 33.98% chose this answer, “A rapid-onset insulin-deficient diabetes that can present as diabetic ketoacidosis.” This answer is correct. Due to immune checkpoint inhibitor-induced immune system alterations, hyperglycemia and insulin deficiency can rapidly develop, often leading to DKA.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!

Join national experts including Dr. Diana Isaacs (Cleveland Clinic), Beverly Thomassian (30+ years of experience), and Christine Craig for high-impact, virtual learning—no travel required.
✔ Learn from National Experts — Anywhere
Get the same expert-level instruction you’d receive in person, delivered live to your home or office.
✔ Interactive & Flexible

Walk away with tools you can apply immediately in clinical practice or while preparing for CDCES or BC-ADM exams. From insulin dosing protocols to behavior change strategies that work in the real world—this content bridges theory and practice.
Get exam-ready with confidence.
Course credits through AMA PRA Category 1 Credits™, ACPE, ANCC, and CDR!
Full accreditation details are available on the registration page

Our CDCES Boot Camp Online Prep Bundle is a comprehensive, high-impact program built specifically for healthcare professionals preparing for the Certified Diabetes Care and Education Specialist (CDCES) exam who want to level up their clinical knowledge and skills.

This evidence-based study bundle is a comprehensive BC-ADM Boot Camp designed for advanced-level healthcare professionals preparing for the Board Certified in Advanced Diabetes Management (BC-ADM) exam and will also provide you with state-of-the-art information to level up your clinical practice.

In diabetes care, what is the reported percentage
of patients who have missed or not returned for follow-up care due to feelings of shame, blame, or judgment?

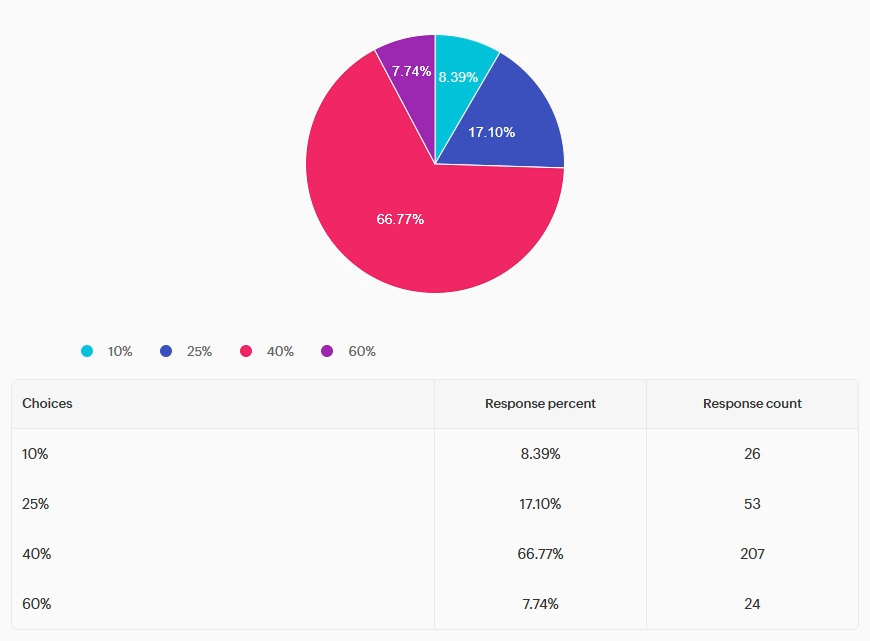
Answer A is incorrect: 8.39% chose this answer, “10%.” This answer underestimates the problem. Research indicates that approximately 40% of patients with diabetes may miss or avoid follow-up appointments because they experience feelings of shame, blame or judgment related to their condition or care. This highlights the importance of delivering diabetes care with stigma-free, supportive communication approaches as a means to improve engagement and outcomes
Answer B is incorrect: 17.10% chose this answer, “25%.” This answer underestimates the problem. Research indicates that approximately 40% of patients with diabetes may miss or avoid follow-up appointments because they experience feelings of shame, blame or judgment related to their condition or care. This highlights the importance of delivering diabetes care with stigma-free, supportive communication approaches as a means to improve engagement and outcomes.
Answer C is correct: 66.77% chose the correct answer, GREAT JOB. “40%.” Per the 2026 ADA Standards of Care, bone health needs to be assessed in men aged ≥50 years with type 2 diabetes and an A1c >8%. He is also on pioglitazone, a thiazolidinedione, which is another risk factor for low bone density.
Answer D is incorrect: 7.74% chose this answer, “60%.” This answer overestimates the problem. Research indicates that approximately 40% of patients with diabetes may miss or avoid follow-up appointments because they experience feelings of shame, blame or judgment related to their condition or care. This highlights the importance of delivering diabetes care with stigma-free, supportive communication approaches as a means to improve engagement and outcomes.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!

All hours earned count toward your CDCES Accreditation Information
The use of DES products does not guarantee the successful passage of the certification exam. CBDCE and ADCES do not endorse any preparatory or review materials for the CDCES or BC-ADM exams, except for those published by CBDCE & ADCES.

Betty, a 60-year-old female, is receiving pembrolizumab, an immune checkpoint inhibitor, as treatment for melanoma. She is worried about the potential adverse effects. She is very concerned about the risk of developing diabetes. Her recent lab work shows normal fasting blood glucose and hemoglobin A1c.
Get exam-ready with confidence.
Course credits through AMA PRA Category 1 Credits™, ACPE, ANCC, and CDR!
Full accreditation details are available on the registration page

Our CDCES Boot Camp Online Prep Bundle is a comprehensive, high-impact program built specifically for healthcare professionals preparing for the Certified Diabetes Care and Education Specialist (CDCES) exam who want to level up their clinical knowledge and skills.

This evidence-based study bundle is a comprehensive BC-ADM Boot Camp designed for advanced-level healthcare professionals preparing for the Board Certified in Advanced Diabetes Management (BC-ADM) exam and will also provide you with state-of-the-art information to level up your clinical practice.

Join national experts including Dr. Diana Isaacs (Cleveland Clinic), Beverly Thomassian (30+ years of experience), and Christine Craig for high-impact, virtual learning—no travel required.
✔ Learn from National Experts — Anywhere
Get the same expert-level instruction you’d receive in person, delivered live to your home or office.
✔ Interactive & Flexible

Walk away with tools you can apply immediately in clinical practice or while preparing for CDCES or BC-ADM exams. From insulin dosing protocols to behavior change strategies that work in the real world—this content bridges theory and practice.



Q: What do you see as the most common misconceptions healthcare professionals have about people who don’t engage effectively with diabetes self-management behaviors?
A: The most common misconceptions are that people who don’t engage with diabetes management are unmotivated, not scared enough, and don’t care about their health.
We asked our favorite diabetes psychologist, Susan Guzman, PhD, to share her insights on how to engage most effectively when providing care to people with diabetes. Keep reading for more expert insights.
Q: How do these misconceptions lead to further problems for people with diabetes and further frustrations for the HCPs?
A: Not understanding the actual barriers to effective engagement leads to responses that don’t help. If you think someone is unmotivated, you might encourage someone to try harder or offer advice that doesn’t meet the person’s needs. If you think someone isn’t taking action because they must not be scared enough, you might try to warn them of all the terrible complications that could happen if they don’t make changes. If you believe someone doesn’t engage with diabetes self-management because they don’t care about their health, you may stop suggesting changes thinking they won’t do it anyway.
Because these are misconceptions, these corresponding tactics are ineffective, often leading people to feel more disengaged and misunderstood, immobilized with fear and hopelessness. In turn, HCPs too can end up feeling more frustrated and hopeless about helping patients reach treatment targets.
Q: What are some of the actual reasons people may not engage with diabetes self-management?
A: There are many common barriers that can result in someone seeing that needed changes as not worth the effort required or seem unachievable. When you begin to see the “good reasons” for people feeling disengaged from diabetes care, you can start to spot solutions that better fit the problem. For example, someone might actually feel doomed (scary complications and early death are unavoidable) and are hopeless that their efforts will have a positive impact. Instead of a scary lecture, this person could really benefit from some “evidence-based hope”, learning that there is good evidence that with targeted effort as a team to reach target, it is possible to have a long and healthy life with diabetes.
Q: Are there quick ways to identify these common barriers to effective diabetes management and brief interventions to help?
A: Yes! There are simple evidence-based ways to identify common behavioral obstacles and address them in routine clinical care. In our one-day workshop, “Engaging the Disengaged: Innovative Strategies for Behavior Change in Diabetes” we will help participants gain confidence in using these tools, having more productive conversations and collaborating with patients in generating more engaging and effective treatment plans.
Q: Are there any upcoming trainings available to explore these techniques and strategies?
A: Yes! Dr. William Polonsky and myself are facilitating a 6-hour conference in San Diego designed to bring these concepts life. This course isn’t a lecture — it’s an immersive, skills-building experience. Using a collaborative, person-centered approach, participants will practice real communication strategies that enhance motivation, build patient confidence, and make self-management feel doable. From diabetes distress to action planning to long-term adherence, every skill you gain is immediately applicable in your practice.
Sign-up today, since we are limiting enrollment to 50 people!

Dr. Susan Guzman is a clinical psychologist specializing in diabetes. In 2003, Dr. Guzman co-founded the Behavioral Diabetes Institute (BDI), the first non-profit organization devoted to the emotional and behavioral aspects of living with diabetes.
At BDI, she serves as the Director of Clinical Education, developing and leading programs for people with diabetes and healthcare professionals. She has helped develop and facilitate diabetes distress group interventions for two NIH-funded research studies for adults with type 1 diabetes.
Dr. Guzman is passionate about helping to change the conversations in diabetes away from shame, blame, and judgment to those based on facts, empathy, and engagement. She has been part of a joint ADA/ADCES effort to address problematic language and messages in diabetes.


Dr. William H. Polonsky, PhD, CDCES
In addition to being the Co-Founder of the Behavioral Diabetes Institute, Dr. Polonsky is Associate Clinical Professor in Medicine at the University of California San Diego.
A licensed clinical psychologist, certified diabetes care and educational specialist (CDCES), and highly-cited research scientist with more than 150 peer-reviewed publications in the field of behavioral diabetes.
His most recent research projects have focused on quality of life in diabetes, diabetes-related distress, hypoglycemic fear, glucose monitoring behavior and attitudes in people living with diabetes, group-based behavior change programs, the influence of continuous glucose monitoring on quality of life, and the development of new methods for enhancing diabetes education. In addition, he continues to maintain a small clinical practice where he works with his patients to help alleviate the stresses, strains and aggravations of living with diabetes.
Of note, he has authored several books for the lay audience (e.g., Diabetes Burnout: What to Do When You Can’t Take it Anymore) and co-edited several others for health care professionals (e.g., A CORE Curriculum for Diabetes Education).