
Subscribe
eNewsletter

Ready to get certified?
Free CDCES Coach App
Download
Free Med Pocket Cards

eNewsletter

Free CDCES Coach App
Free Med Pocket Cards

About 30% of people with diabetes started on GLP-1’s stop taking this medication before completing a year of therapy.
According to ADA Standards, what results from sudden discontinuation of GLP-1s /GIP like semaglutide and tirzepatide?

Gain fresh insights, practical tools, and a deeper understanding of the latest in person-centered diabetes care. Our expert team brings the ADA Standards of Care to life—covering medications, behavior change, technology, and more! If you’re preparing for the CDCES or BC-ADM exam, this conference—paired with free bonus courses—serves as the ideal study companion!
With interactive co-teaching, we keep sessions engaging, relevant, and fun. Let’s learn and grow together!

Our expert team transforms complex diabetes science into clear, practical insights—keeping it real, engaging, and fun! The faculty includes:
For last week’s practice question, we quizzed participants oAction needed to prevent heart failure. 41% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it below: Answer Question

Question:
Adults with diabetes are at increased risk for the development of asymptomatic or symptomatic heart failure.
According to the ADA 2025 Standards of care, what action is needed to facilitate prevention of heart failure?
Answer Choices:
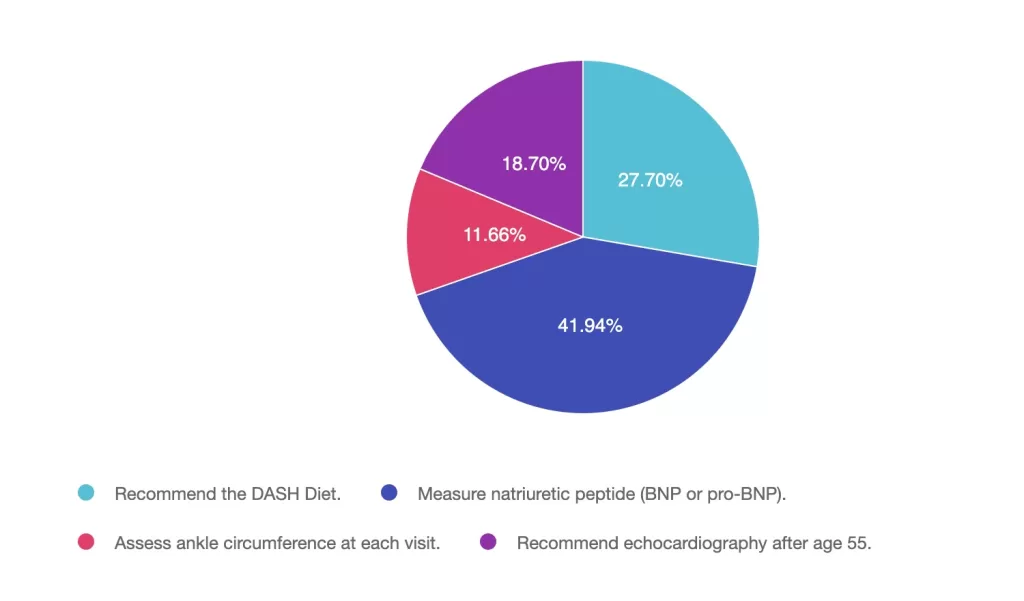
Answer 1 is incorrect. 27% chose this juicy answer. “Recommend the DASH Diet.” Although the DASH Diet with lower sodium content is helpful once someone is diagnosed with heart failure, this dietary approach alone won’t prevent heart failure. In order to prevent heart failure, it needs to first be diagnosed to determine best treatment plan.
Answer 2 is correct. 49% of you chose this answer. “Measure natriuretic peptide (BNP or pro-BNP).” YES, Great JOB. According to the ADA Standard on ASCVD, “Adults with diabetes are at increased risk for the development of asymptomatic cardiac structural or functional abnormalities (stage B heart failure) or symptomatic (stage C) heart failure. Consider screening adults with diabetes by measuring a natriuretic peptide (B-type natriuretic peptide [BNP] or N-terminal pro-BNP [NT-proBNP]) to facilitate prevention of stage C heart failure. In asymptomatic individuals with diabetes and abnormal natriuretic peptide levels, echocardiography is recommended to identify stage B heart failure.”
Answer 3 is incorrect. About 11% of respondents chose this. “Assess ankle circumference at each visit.” Although pedal edema and shortness of breath are both indicators of heart failure, the BNP or NT-proBNP lab test is more definitive.
Finally, Answer 4 is incorrect. 18% chose this answer. “Recommend echocardiography after age 55.” According to ADA standards, we would first check the BNP or NT-proBNP lab test. In asymptomatic individuals with diabetes and abnormal natriuretic peptide levels, echocardiography is then recommended to identify stage B heart failure.”
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!

Gain fresh insights, practical tools, and a deeper understanding of the latest in person-centered diabetes care. Our expert team brings the ADA Standards of Care to life—covering medications, behavior change, technology, and more! If you’re preparing for the CDCES or BC-ADM exam, this conference—paired with free bonus courses—serves as the ideal study companion!
With interactive co-teaching, we keep sessions engaging, relevant, and fun. Let’s learn and grow together!

Our expert team transforms complex diabetes science into clear, practical insights—keeping it real, engaging, and fun! The faculty includes:

According to the 2025 ADA Standards of Care, which of the following nutrition behaviors are strongly encouraged for individuals with diabetes?

Gain fresh insights, practical tools, and a deeper understanding of the latest in person-centered diabetes care. Our expert team brings the ADA Standards of Care to life—covering medications, behavior change, technology, and more! If you’re preparing for the CDCES or BC-ADM exam, this conference—paired with free bonus courses—serves as the ideal study companion!
With interactive co-teaching, we keep sessions engaging, relevant, and fun. Let’s learn and grow together!

Our expert team transforms complex diabetes science into clear, practical insights—keeping it real, engaging, and fun! The faculty includes:

Announcements
_________________________
Upcoming Programs
___________________________
February is all about love, 💙 and that spirit shines brightly in diabetes care and education! We speak from the heart as we advocate for evidence-based care that supports well-being and transforms lives.
In recognition of these daily contributions of diabetes care and education specialists, we are delighted to announce our annual “Spreading the Love” Sale! Enjoy 20% off all our online courses, including program extensions through February 16th.
This month’s newsletter includes exciting information on a new “front-of-package” food labeling proposal that aims to provide more accurate and accessible information for consumers, before adding packaged foods to their carts.
We announce the approval of semaglutide as a first-line agent to protect renal function in people living with chronic kidney disease.
Have you ever considered volunteering at a diabetes camp? After reading this article contributed by a camper and later a diabetes nurse educator, you might be inspired to sign up for a camp near you.
DiabetesEd Services is thrilled to announce an exciting milestone—our first-ever offering of 14 Scholarships for healthcare professionals dedicated to serving under-resourced communities. This initiative is part of our Bridge Program, aimed at mentoring 1,000 new diabetes care professionals over the next ten years.
As always, test your knowledge with our Question and Rationale of the week. We hope to see you at our 3-Day Virtual DiabetesEd Training Conference in April or at a future event!
With love,
Coach Beverly, Bryanna, Tiffany, Christine, & Katarina

Gain fresh insights, practical tools, and a deeper understanding of the latest in person-centered diabetes care. Our expert team brings the ADA Standards of Care to life—covering medications, behavior change, technology, and more! If you’re preparing for the CDCES or BC-ADM exam, this conference—paired with free bonus courses—serves as the ideal study companion!
With interactive co-teaching, we keep sessions engaging, relevant, and fun. Let’s learn and grow together!

Our expert team transforms complex diabetes science into clear, practical insights—keeping it real, engaging, and fun! The faculty includes:
For last week’s practice question, we quizzed participants on what defines overbasalization according to 2025 ADA Standards? 60% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it below: Answer Question

Question:
According to ADA 2025 Standards, more intensive preventive approaches should be considered in individuals who are at particularly high risk of progression to diabetes, including individuals with BMI ≥35 kg/m2 who:
Answer Choices:
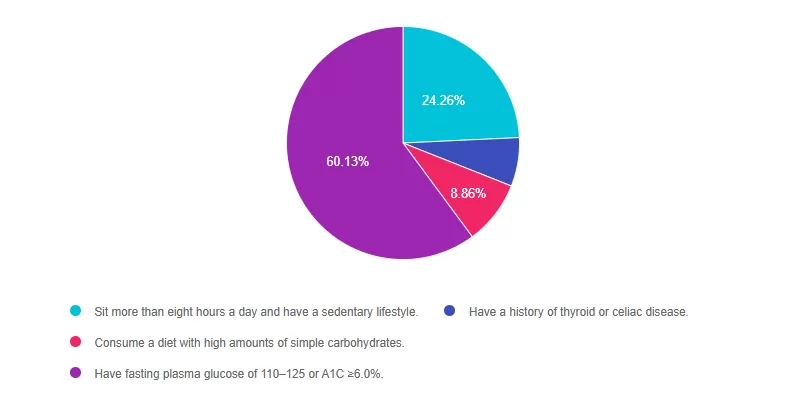
Answer 1 is incorrect. 25% chose this answer, “Sit more than eight hours a day and have a sedentary lifestyle”. Although the ADA Standards recommend getting up and moving every half-hour, they don’t specify that eight hours of sitting a day qualifies a person as higher risk to progressing to diabetes.
Answer 2 is incorrect. 7% of you chose this answer “Have a history of thyroid or celiac disease”. These autoimmune conditions are more closely associated with immune mediated type 1 diabetes and do not place a person as higher risk for progression to type 2 diabetes.
Answer 3 is incorrect. About 9% of respondents chose this, “Consume a diet with high amounts of simple carbohydrates.” While eating foods rich in fiber and a variety of nutrients is important to decrease risk of diabetes, the ADA does not state that eating simple carbohydrates puts individuals in a higher risk category of progressing to diabetes.
Finally, Answer 4 is correct 60% chose this answer, “Have fasting plasma glucose of 110–125 or A1C ≥6.0%.” Great job. This is the BEST answer. According to ADA 2025 Standards, “More intensive preventive approaches should be considered in individuals who are at particularly high risk of progression to diabetes, including individuals with BMI ≥35 kg/m2, those at higher glucose levels (e.g., fasting plasma glucose 110–125 mg/dL [6.1–6.9 mmol/L], 2-h post challenge glucose 173–199 mg/dL [9.6–11.0 mmol/L], and A1C ≥6.0% [≥42 mmol/mol]), and individuals with a history of gestational diabetes mellitus.”
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!

Gain fresh insights, practical tools, and a deeper understanding of the latest in person-centered diabetes care. Our expert team brings the ADA Standards of Care to life—covering medications, behavior change, technology, and more! If you’re preparing for the CDCES or BC-ADM exam, this conference—paired with free bonus courses—serves as the ideal study companion!
With interactive co-teaching, we keep sessions engaging, relevant, and fun. Let’s learn and grow together!

Our expert team transforms complex diabetes science into clear, practical insights—keeping it real, engaging, and fun! The faculty includes:
by Jeannie Hickey, RN, CDE


In 1965, when I was just 12 years old, my parents dropped me off at Bearskin Meadows, a two-week camp for kids with Type 1 diabetes. It was shortly after I had been diagnosed, and I was still adjusting to my new reality. I remember the daily routines vividly—carrying my cup of urine to the “lab,” lining up for my Regular and NPH injections twice a day, and using meal cards that followed the exchange system for servings.
But even with all that, there were moments of pure joy. I recall playing, singing around the campfire, and yes—roasting marshmallows for s’mores! (A sugary snack at a diabetes camp? Go figure!)
By the time I returned home, I felt much more comfortable with my condition and, more importantly, I felt hopeful. That experience gave me a sense of community and confidence that would shape my relationship with diabetes for years to come.
Fast forward 35 years. Now a Registered Nurse and Certified Diabetes Educator (RN, CDE), I found myself at a “Back to School” conference for parents of children with Type 1 diabetes, hosted by Diabetes Youth Families (DYF). During the event, camp counselors were leading the kids’ activities, and I recognized familiar images from the very same camp I had attended as a child. They invited me to return as a volunteer RN, offering insulin dose adjustments for a group of campers and helping with daily education alongside endocrinologists and other diabetes professionals. (And yes, there were CEUs too!)



That opportunity was life-changing. What started as a one-time volunteer experience quickly turned into a 21-year, part-time summer job. From my initial role as a volunteer, I eventually became the Assistant Medical Director, overseeing the medical care for kids, teens, and families during the two-month camp season. The work I did with Diabetes Youth Families was incredibly rewarding, and I continue to be inspired by the campers and their families each year.
I am thrilled to share my story and encourage you to consider signing up for this unique opportunity of volunteering at T1D camp. You get to learn about and support kids navigating type 1 while diabetes while they are having fun at camp.
Many states have camps, both independent, ADA, or through the Lions. Some offer state CEUs for your volunteer hours and the medical education presented by MDs, other RNs, RDs or Mental Health. DECA – Diabetes Education & Camping Association has a list of accredited camps to consider.
Jeannie Hickey RN, CDE (past Asst Med Dir for Bearskin Meadow Camp through Diabetes Youth Families)
T1D 60 yrs this July!!
If this is an experience you’d like to explore, there are many accredited camps and conferences available. Check out resources like Diabetes Youth Families to find a camp near you and make lasting connections with others living with Type 1 diabetes. Teen Ed Day Sponsorship Packet

While volunteering at camp your learning objectives are:
If new to camp, you will be partnered with a physician or RN until you feel comfortable with the protocol. There will be pump savvy RNs to support & assist your learning. You will not be on your own.
You can also support your Families by learning more about camp and encouraging them to attend as a family, or send their kids (and get a week free from diabetes). See the helpful resources below.

Gain fresh insights, practical tools, and a deeper understanding of the latest in person-centered diabetes care. Our expert team brings the ADA Standards of Care to life—covering medications, behavior change, technology, and more! If you’re preparing for the CDCES or BC-ADM exam, this conference—paired with free bonus courses—serves as the ideal study companion!
With interactive co-teaching, we keep sessions engaging, relevant, and fun. Let’s learn and grow together!

Our expert team transforms complex diabetes science into clear, practical insights—keeping it real, engaging, and fun! The faculty includes:

Adults with diabetes are at increased risk for the development of asymptomatic or symptomatic heart failure.
According to the ADA 2025 Standards of care, what action is needed to facilitate prevention of heart failure?

Ready for your certification exams? Our Level 3 course series is the final step in your exam prep, complementing our Level 1, 2, or 4 bundles. Designed for healthcare professionals preparing for diabetes certification exams in 3-6 months, this master-level series covers key topics like pharmacology, technology, MNT, and person-centered care, all based on the latest ADA Standards of Care.
Each course includes a video, podcast, practice test, and additional resources—available immediately for one full year. Boost your knowledge and confidence to succeed in your certification!
 Given my seven-time experience taking the CDCES exam, I can say with complete conviction that being familiar with the American Diabetes Association (ADA) Standards of Care is one of the most important and essential strategies to prepare for exam success. More importantly, this evidence-based guidebook is crucial for providing the best clinical and person-centered care, with close attention to the Social Determinants of Health.
Given my seven-time experience taking the CDCES exam, I can say with complete conviction that being familiar with the American Diabetes Association (ADA) Standards of Care is one of the most important and essential strategies to prepare for exam success. More importantly, this evidence-based guidebook is crucial for providing the best clinical and person-centered care, with close attention to the Social Determinants of Health.
If you are taking the exam in January or February 2025 and you have already read the 2024 ADA Standards cover-to-cover, you are all set. It takes at least a year for the exam writers to include new questions culled from the ADA Standards. Having said that, if there are any critical new guidelines that impact clinical care, education, or treatment of diabetes, that content can be included in the exam that same year. From my review of the 2025 Standards, there are no critical new clinical guidelines that need immediate adoption into practice. One important caveat to consider: if you are relying on last year’s standards, make sure to read through the Summary of Revisions section included in the Standard of Care, so that you that latest information under your belt.
On the other hand, if you are taking the exam in 2025 and haven’t reviewed the ADA Standards in the past, I recommend a thorough review of the most recent ADA Standards. You can access the ADA Standards on our CDCES Coach App and the ADA Website at www.diabetes.org.
In case of emergency, there is a shorter version of the ADA Standards called the Abridged version for Primary Care Providers that highlights critical clinical content. The abridged version is usually released in February by the ADA. It can also be used as a quick review after you have read the document in full. Again, after successfully passing the exam seven times, my advice is to be familiar with the ADA Standards of Care in its entirety.

Below is an excerpt from the CBDCE Exam Handbook regarding what hours count towards this 1000-hour DSME requirement:
To help you keep track of your hours, we created the Diabetes Management Hours Tracker. The column “Remaining Hours Needed” is a formula that is tied to “Hours Completed” so be sure to only put numbers in the hour’s column so the formula automatically deducts those hours to get the remaining hours you need. Make sure you let your supervisor know you are tracking your hours, since they will need to attest and verify DSME hours completed.
Tracking your activities and hours consistently is key and this Hours Tracker excel sheet can help you tally your hours, while working toward your goal of becoming a CDCES.
Meeting the 1,000-hour requirement for the Certified Diabetes Care and Education Specialist (CDCES) exam is achievable with a variety of approaches. The hours needed can include volunteer or paid hours. Below are some practical ways to accumulate hours if you are not able to accrue enough hours in your current work environment.
As part of our Bridge Program, Coach Beverly wants to support YOUR efforts to mentor a new generation of Diabetes Care and Education Specialists. If you are a mentor, we are offering significant discounts off of our Diabetes Boot Camp or Virtual 3 Day Program for groups of mentees who are practicing in underserved regions of our country. Please email us for more information at [email protected]

This webinar provides a comprehensive breakdown of the ADA Standards of Care, focusing on essential content for clinical practice and exam success.
This webinar is designed for healthcare professionals aiming to deepen their understanding of the ADA Standards for improved practice or preparing for the BC-ADM or CDCES certification exams.