
Not having our basic needs met, like limited access to food, has a dramatic impact on our mental health.
The pandemic has significantly impacted our mental health due to the trauma, social isolation, and economic instability which has led to an increase in food insecurity.
Since the start of the pandemic, the number of families experiencing food insecurity has increased dramatically, from 8.1% to 10.0% from March to June 2020.
As Diabetes Care & Education Specialists, we realize how important access to healthy, nutritious foods are for diabetes self-care and mental health. Addressing food insecurity and providing resources to fill in gaps, can be a lifeline and improve mental health for people living with diabetes.
A recent study led by Jason M. Nagata, MD, MSc, who works in the Division of Adolescent and Young Adult Medicine, Department of Pediatrics, at UCSF dove into the correlation between food insecurity and mental health.
“Food insecurity is associated with diets high in low-cost, energy-dense packaged foods, but low in fruits and vegetables, which may lead to chronic medical conditions such as diabetes and hypertension, both of which are known to be associated with a higher risk for severe COVID-19 illness” the study states.
The study highlights how different populations are more at risk of experiencing food insecurity with lower-income, single individuals or large families, people of color, those recently unemployed, and people younger in age being the most affected.
Food access disparities that disproportionately affect people of color and low-income individuals and families have been an ongoing public health concern, even before the pandemic.
The study by Dr. Nagata and team cites the term “food apartheid” which activist Dara Cooper describes as the “blatantly discriminatory corporate-controlled food system that results in [communities of color] suffering from some of the highest rates of heart disease and diabetes of all time.”
Food shortages due to border closures, essential workers falling ill, school closures that provided meals to over 35 million children pre-pandemic, and the overall economic crisis, have exasperated food insecurity.
“Food insecurity may lead to poor mental health through chronic stress, stigmatization, and perceived powerlessness. Conversely, people experiencing poor mental health symptoms may be less able to work, generate income, or manage financial resources, which could exacerbate food insecurity.”
The study used cross-sectional data from the U.S. Census Household Pulse Survey that was collected and analyzed in 2020 across 63,674 participants. Those who experienced food insufficiency in the past 7 days were more likely to experience mental health outcomes such as anxiety, worry, anhedonia, and depression.
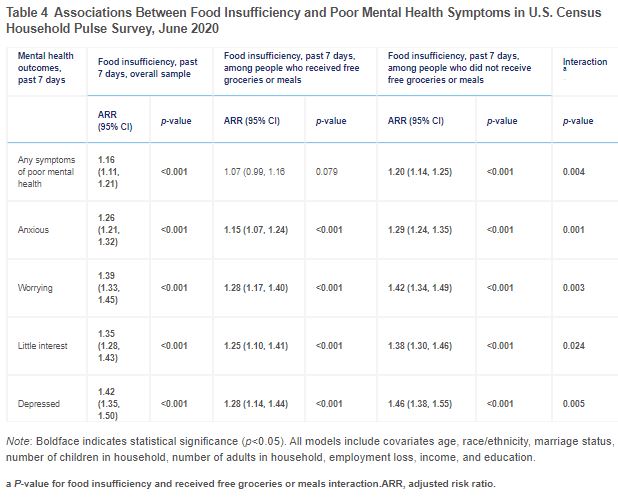
A decrease in mental health symptoms was noted for those who received free groceries within the past 7 days.
The study concludes that assistance programs that provide free meals, financial assistance, paid sick leave, mental health resources, and stimulus funding can help decrease the cycle of food insecurity and improve mental health outcomes.
To read more, click here to view the study.
Click here to read more about food apartheid.
Written by Bryanna, our Director of Operations & Customer Happiness
More Resources for Health Care Providers
The National CLAS Standards website (https://thinkculturalhealth.hhs.gov) offers a number of resources and materials that can be used to improve the quality of care delivery to non–English-speaking patients
The ADA provides a list of mental health providers who have received additional education in diabetes at the ADA Mental Health Provider Directory (professional.diabetes.org/mhp_listing).
Join Coach Beverly for her annual- Recorded and Ready for Viewing
Level 2 – Standards of Care Update!
This course is an essential review for anyone in the field of diabetes. This course summarizes the 2021 updates to the American Diabetes Association’s Standards of Medical Care in Diabetes and provides critical teaching points and content for health care professionals involved in diabetes care and education.
Earn 2.0 CEs and get ready to lead the charge to implement best care practices for the New Year.
Topics Include:
- A review of changes and updates to the 2021 ADA Standards of Medical Care
- Identification of key elements of the position statement
- Discussion of how diabetes educators can apply this information in their clinical setting
Sign up for Diabetes Blog Bytes – we post one daily Blog Byte from Monday to Friday. And of course, Tuesday is our Question of the Week. It’s Informative and FREE! Sign up below!
[yikes-mailchimp form=”1″]
Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and Commission on Dietetic Registration (CDR), Provider DI002. Since these programs are approved by the CDR it satisfies the CE requirements for the CDCES regardless of your profession.*
The use of DES products does not guarantee the successful passage of the CDCES exam. CBDCE does not endorse any preparatory or review materials for the CDCES exam, except for those published by CBDCE.




