For last week’s practice question, we quizzed participants on Managing Overnight Hypoglycemia: Best Plan? 86% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it below: Answer Question

Question: Your client wants to discuss a concern about overnight hypoglycemia alerts on the CGM. These hypoglycemia alerts have been happening intermittently and only in the overnight hours. The client reports no changes in diet, activity, or insulin doses over the past 2 weeks. These events are asymptomatic, and the client reports that these episodes resolve rapidly before they can get to the kitchen to treat the hypoglycemic event. What is the best plan of action for this client?
Answer Choices:
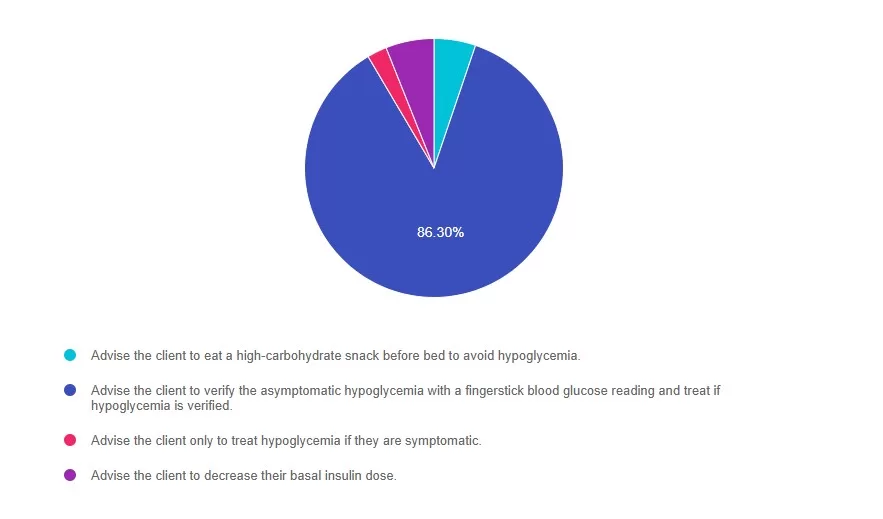
- Advise the client to eat a high-carbohydrate snack before bed to avoid hypoglycemia.
- Advise the client to verify the asymptomatic hypoglycemia with a fingerstick blood glucose reading and treat if hypoglycemia is verified.
- Advise the client only to treat hypoglycemia if they are symptomatic.
- Advise the client to decrease their basal insulin dose.
Getting to the Best Answer
Answer 1 is incorrect. 4% chose this answer, “Advise the client to eat a high-carbohydrate snack before bed to avoid hypoglycemia.” Although tempting, eating a high-carbohydrate snack before bed doesn’t address the need to verify an asymptomatic and unexpected low blood glucose.
Answer 2 is correct. 86% of you chose this answer, “Advise the client to verify the asymptomatic hypoglycemia with a fingerstick blood glucose reading and treat if hypoglycemia is verified.” GREAT JOB! Continuous glucose monitors are susceptible to compression lows. These lows occur when pressure is applied to the sensor/transmitter, which can occur during sleep. This can result in hypoglycemia alerts. Diabetes care and education specialists can help recognize this pattern and coach clients using CGM technology to verify any asymptomatic or unexpected hypoglycemia with a fingerstick blood glucose reading before making a treatment decision.
Answer 3 is incorrect. About 2% of respondents chose this, “Advise the client only to treat hypoglycemia if they are symptomatic.” All clients need to be encouraged to verify any unexpected glucose readings, particularly if they have asymptomatic hypoglycemia, with a fingerstick blood glucose reading before treating.”
Finally, Answer 4 is incorrect. About 5% of you chose this answer, “Advise the client to decrease their basal insulin dose.” The blood glucose readings need to be verified before adjusting the basal insulin dose.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!
ReVive 5 Diabetes Training Program: A Person-Centered Approach to Diabetes Distress & Glucose Management
Join us live on July 15th and July 22nd, 2025 at 9:00 am PST
6+ CEs with Expanded Accreditation!

Join experts Larry Fisher, Ph.D., ABPP, Susan Guzman, Ph.D., and Coach Beverly Thomassian, RN, MPH, CDCES, BC-ADM, for this transformative two-part training on the ReVive 5 framework—an evidence-based approach that integrates emotional well-being and glucose data into person-centered diabetes care.
Grounded in the results of the EMBARK Trial, this program emphasizes the urgent need to assess and address diabetes distress, now recognized in the ADA Standards of Care as a critical component of care. You’ll gain practical tools and strategies used in the trial to support emotional well-being, meet clinical standards, and empower individuals on their diabetes journey.
Program Objectives:
Upon completion of this activity, participants will be able to:
- Identify the key differences between diabetes distress and depression and explain their impact on self-care behaviors.
- Apply evidence-based communication strategies to respond to diabetes distress screening results.
- Demonstrate how to analyze glucose patterns using meter and sensor data.
- Utilize the ReVive 5-step approach to integrate emotional and glucose management into diabetes care.
Team of Experts:
ReVive 5 is taught by a team of 3 Interdisciplinary Experts:



Lawrence Fisher, Ph.D., ABPP
Professor Emeritus, UCSF
Susan Guzman, PhD
Beverly Thomassian, RN, MPH, CDCES, BC-ADM
CEO of DiabetesEd Services
Faculty Bios & Disclosures
Program Faculty Disclosures:
Partners for Advancing Clinical Education (Partners) requires every individual in a position to control educational content to disclose all financial relationships with ineligible companies that have occurred within the past 24 months. Ineligible companies are organizations whose primary business is producing, marketing, selling, re-selling, or distributing healthcare products used by or on patients.
All relevant financial relationships for anyone with the ability to control the content of this educational activity are listed below and have been mitigated according to Partners policies. Others involved in the planning of this activity have no relevant financial relationships.
Faculy Bios & Disclosures:
 Lawrence Fisher, Ph.D., ABPP, Professor Emeritus, UCSF
Lawrence Fisher, Ph.D., ABPP, Professor Emeritus, UCSF
- Consultant, advisor, and speaker for Eli Lilly
Speaker Interview:
Bio:
Dr. Fisher has been a professor in the Department of Family & Community Medicine at the University of California, San Francisco for over 25 years, and he is the Director of The Behavioral Diabetes Research Group at UCSF.
He has a Diplomate in Clinical Psychology from the American Board of Professional Psychology and is a former Associate Editor of Diabetes Care. He has conducted multiple cross-sectional and longitudinal NIH- and ADA-supported clinical research with adults with diabetes and their families.
His recent work focuses on diabetes distress and depression, disease management, and how adults and families struggle over time to manage chronic health conditions. He has won two major UCSF School of Medicine teaching awards, was nominated for the UCSF Postdoctoral Scholars Association Outstanding Mentorship Award, and has received a certificate from the American Psychological Association in “Recognition for Substantial Contributions to the Field of Family Psychology and Health.”
In 2012 he received the Richard Rubin Award from the American Diabetes Association. He maintains an active clinical practice at UCSF, has published over 190 peer-reviewed articles on diabetes and related topics, and frequently speaks to both professional and lay groups at local, national, and international meetings and workshops.
 Susan Guzman, PhD
Susan Guzman, PhD
- Consultant, advisor, and speaker for Abbot Labratories and Embecta
Dr. Guzman is a clinical psychologist specializing in diabetes. In 2003, Dr. Guzman co-founded the Behavioral Diabetes Institute (BDI), the first non-profit organization devoted to the emotional and behavioral aspects of living with diabetes.
At BDI, she serves as the Director of Clinical Education, developing and leading programs for people with diabetes and healthcare professionals. She has helped develop and facilitate diabetes distress group interventions for two NIH-funded research studies for adults with type 1 diabetes.
Dr. Guzman is passionate about helping to change the conversations in diabetes away from shame, blame, and judgment to those based on facts, empathy, and engagement. She has been part of a joint ADA/ADCES effort to address problematic language and messages in diabetes.
 Coach Beverly Thomassian RN, MPH, CDCES, BC-ADM
Coach Beverly Thomassian RN, MPH, CDCES, BC-ADMBeverly Thomassian has no financial disclosures
Speaker Interview:
Bio:
Expanded Accreditation
Activity Start and End Date: 7/15/2025 to 7/22/2027
Estimated time to complete the activity: 6 hours and 15 minutes
Jointly provided by Partners for Advancing Clinical Education and Diabetes Education Services
![]()
![]()
Joint Accreditation Statement:
 In support of improving patient care, this activity has been planned and implemented by Partners for Advancing Clinical Education (Partners) and Diabetes Education Services. Partners is jointly accredited by the Accreditation Council for Continuing Medical Education (ACCME), the Accreditation Council for Pharmacy Education (ACPE), and the American Nurses Credentialing Center (ANCC), to provide continuing education for the healthcare team.
In support of improving patient care, this activity has been planned and implemented by Partners for Advancing Clinical Education (Partners) and Diabetes Education Services. Partners is jointly accredited by the Accreditation Council for Continuing Medical Education (ACCME), the Accreditation Council for Pharmacy Education (ACPE), and the American Nurses Credentialing Center (ANCC), to provide continuing education for the healthcare team.
Physician Continuing Education:
Partners designates this enduring material for a maximum of 6.25 AMA PRA Category 1 Credit(s)™. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Nursing Continuing Professional Development:
The maximum number of hours awarded for this Nursing Continuing Professional Development activity is 6.25 contact hours.
Pharmacy Continuing Education:
Partners designates this continuing education activity for 6.25 contact hour(s) (.625] CEUs) of the Accreditation Council for Pharmacy Education.
(Universal Activity Number – UAN JA4008073-9999-25-198-H01-P)
Type of Activity: Application
For Pharmacists: Upon successfully completing the activity evaluation form, transcript information will be sent to the NABP CPE Monitor Service within 4 weeks.
Dietitian Continuing Education:
This program offers 6.25 CPEUs for dietitians.
Interprofessional Continuing Education:
![]() This activity was planned by and for the healthcare team, and learners will receive 6.25 Interprofessional Continuing Education (IPCE) credit for learning and change.
This activity was planned by and for the healthcare team, and learners will receive 6.25 Interprofessional Continuing Education (IPCE) credit for learning and change.
Disclosure of Unlabeled Use:
This educational activity may contain discussion of published and/or investigational uses of agents that are not indicated by the FDA. The planners of this activity do not recommend the use of any agent outside of the labeled indications. The opinions expressed in the educational activity are those of the faculty and do not necessarily represent the views of the planners. Please refer to the official prescribing information for each product for discussion of approved indications, contraindications, and warnings.
Disclaimer:
Participants have an implied responsibility to use the newly acquired information to enhance patient outcomes and their own professional development. The information presented in this activity is not meant to serve as a guideline for patient management. Any procedures, medications, or other courses of diagnosis or treatment discussed or suggested in this activity should not be used by clinicians without evaluation of their patient’s conditions and possible contraindications and/or dangers in use, review of any applicable manufacturer’s product information, and comparison with recommendations of other authorities.
Instructions for Credit
Participation in this self-study activity should be completed in approximately 6 hours and 15 minutes. To successfully complete this activity and receive CE credit, learners must follow these steps during the period from 7/15/2025 to 7/22/2027.
- Review the objectives and disclosures
- Study the educational content in Online University
- After review of content, a module within the course in the Online University will list a link to Partners for Advancing Clinical Education’s website
- Visit Partners for Advancing Clinical Education website listed in course in the Online University
- Complete the activity evaluation through Partners for Advancing Clinical Education website
For additional information about the accreditation of this activity, please visit https://partnersed.com.
The use of DES products does not guarantee the successful passage of the certification exam. CBDCE and ADCES do not endorse any preparatory or review materials for the CDCES or BC-ADM exams, except for those published by CBDCE & ADCES.




