
Subscribe
eNewsletter

Ready to get certified?
Free CDCES Coach App
Download
Free Med Pocket Cards

eNewsletter

Free CDCES Coach App
Free Med Pocket Cards
Increasing global temperatures are expected to impact the health of people living with diabetes and lead to worse outcomes, according to an article published in the Journal of Community Hospital Internal Medicine Perspectives,

People with diabetes are at greater risk of experiencing dehydration and cardiovascular events during periods of extreme heat. Several studies reveal that people with diabetes are more likely to need emergency care during heat waves and those with a history of heart disease are most vulnerable.
To keep healthy and reduce risk during heatwaves, we have put a list together of actions people with diabetes can take to stay safe in the heat.
Download PDF Handout of 19 Actions Here

October 9th-11th, 2024

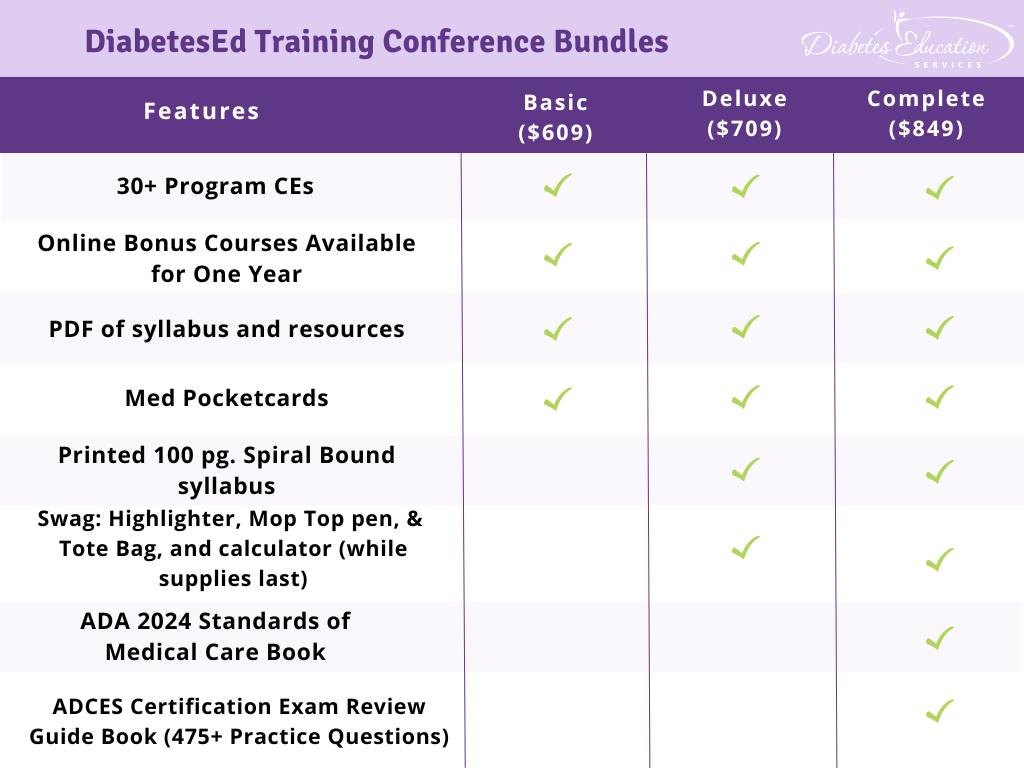
Join Coach Beverly and Team for two and a half days of knowledge-sharing, fun, networking, games with prizes, and “aha” moments in beautiful San Diego on October 9-11, 2024.
You don’t want to miss this one-of-a-kind learning opportunity. Get away from all those daily responsibilities and immerse yourself in a fun and intensive conference with plenty of networking opportunities.
Attendees will leave this conference with new tools and a more complete understanding of the latest advances in diabetes care, from medications to technology to Medical Nutrition Therapy!
Each day, we provide a healthy breakfast, including fresh coffee, to kick off your morning. Our instructors co-teach the content to keep things fresh and lively. Plus, we play DiaBingo to reinforce key content. In addition, we provide plenty of movement breaks led by volunteers from the audience. Did we mention delicious lunches and a conference meeting space just minutes from San Diego Bay?
Friend Discount: 3 or more only $559-$799 (based on registration package) per person. Email us at [email protected] with the name and email of each registrant to get the discount!
Time: The course is Wednesday through Friday. Join us for breakfast at 7:00 a.m. each day. The class begins at 8:00 a.m. and ends at 5:00 p.m. on Wednesday and Thursday and at 3:00 p.m. on Friday.
The use of DES products does not guarantee the successful passage of the certification exam. CBDCE and ADCES do not endorse any preparatory or review materials for the CDCES or BC-ADM exams, except for those published by CBDCE & ADCES.
 Once weekly basal insulin, icodec, failed to be approved for use by people with type 1 diabetes by the FDA’s Endocrinologic and Metabolic Drugs Advisory Committee by a vote of 7-4. The significantly increased risk for hypoglycemia on days two through four after administration outweighed its potential benefits. The committee also noted that icodec’s risk of hypoglycemia is higher than the basal insulin degludec, which is commonly used and has a better safety profile. Other committee members expressed concerns that approving icodec based on inadequate data could discourage further trials that are needed to ensure its safe use.
Once weekly basal insulin, icodec, failed to be approved for use by people with type 1 diabetes by the FDA’s Endocrinologic and Metabolic Drugs Advisory Committee by a vote of 7-4. The significantly increased risk for hypoglycemia on days two through four after administration outweighed its potential benefits. The committee also noted that icodec’s risk of hypoglycemia is higher than the basal insulin degludec, which is commonly used and has a better safety profile. Other committee members expressed concerns that approving icodec based on inadequate data could discourage further trials that are needed to ensure its safe use.
In an effort to secure approval, the applicants for icodec suggested the following actions to improve the safety profile of this novel weekly insulin.
Proposed mitigating actions to reduce hypoglycemia risk by the applicant included;
Even though mitigating actions were suggested to decrease this hypoglycemia risk during this two day peak, the FDA panel members still deferred approval, citing safety concerns due to the significant hypoglycemia risk and need for more data..
Surprisingly, about one third of people living with type 1 diabetes are still managing blood sugars with multiple daily injections. This is especially true for people living in under resourced communities and people of color living with type 1 diabetes. Due to barriers and social determinants of health, in addition to struggling with multiple daily injections, they are also less likely to use continuous glucose monitors or check blood sugars on a regular basis. Although, once a week insulin seems ideal for individuals who may be experiencing a variety of barriers to injecting daily insulin, the main issue is the increased risk of hypoglycemia during days 2-4 when icodec is peaking coupled with limited access to glucose monitoring.
In addition, consistent injected insulin therapy in adults with type 1 diabetes was reported to be relatively low (52.6%, 95% confidence interval[CI]: 37.4 to 67.9%) in data from a meta-analysis of eight clinical trials. The probability of missing at least one daily basal insulin dose over any 14-day period is estimated to be 22% (95% CI: 10 to 40%).
Among individuals with type 2 diabetes, using a daily basal insulin, a once weekly basal insulin would reduce the number of insulin injections from 365 per year to 52 per year. In a recent study, 91% of people with type 2 diabetes and 89% of providers had a positive view of taking basal insulin once weekly.
Among individuals with type 1 diabetes, who rely on a basal bolus regimen, a once weekly basal insulin would reduce the number of insulin injections from approximately 28 per week to 22 per week. For those with type 1 diabetes, there is no research to date that evaluates whether a once weekly basal insulin would be preferred over other basal insulin options, or whether use would result in improved adherence and glycemic control.
In ONWARDS 6, weekly insulin icodec was noninferior (but not superior) to daily insulin degludec and was associated with 48 to 89% more level two and three hypoglycemia at Week 26, depending on the method of analysis. The highest risk period for hypoglycemia with insulin icodec coincides with its peak glucose-lowering effect which occurs on days 2 to 4 following each weekly injection. There were also more hypoglycemia-related serious adverse events reported among patients randomized to insulin icodec compared to insulin degludec.
Thus, in the only study conducted in participants with type 1 diabetes, insulin icodec was observed to have a higher risk of clinically meaningful hypoglycemia, in the absence of a lower A1C. Hypoglycemic episodes reported with insulin icodec and insulin degludec in ONWARDS 6 were of the same nature in terms of duration, management, and recovery.
Insulin icodec is an acylated long-acting human insulin analog produced by a process that includes expression of recombinant DNA in yeast (Saccharomyces cerevisiae), followed by chemical modification. In addition to amino acid sequencing changes, a C20 fatty-acid side chain has been added to the peptide backbone via the amino group in the side chain at Lys(B29). When insulin icodec is injected, the C20 fatty acid sidechain derivative binds strongly, but reversibly, to endogenous albumin, which results in decreased renal clearance and protection from metabolic degradation, and consequently prolonged pharmacodynamic activity.
Insulin icodec is a proposed insulin analog with a prolonged duration of action intended to support once weekly (QW) subcutaneous administration. Thus, insulin icodec reduces treatment burden in type 1 diabetes, by reducing the number of basal insulin injections in comparison to daily basal insulins.
However,basal insulin icodec does not have a peakless time-action profile throughout the dosing interval (see chart below).
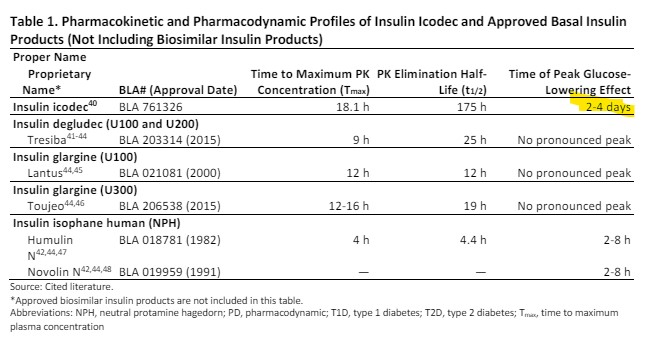
In conclusion, it seems certain that the manufacturers of insulin icodec will be seeking approval for this once weekly insulin for people living with type 1 and type 2 diabetes in the future. Stay tuned for more insulin updates with our monthly newsletter.
Information from this article was obtained from review of the FDA Presentation Document and Slides, May 24, 2024.
Accreditation: The Diabetes Educator Live Course is approved for 26 Contact Hours for nurses and CA Pharmacists and 21 CPE, Level III for RDs. Provider is approved by the California Board of Registered Nursing, Provider # 12640 and Commission on Dietetic Registration (CDR), Provider # DI002. Need hours for your CDCES? We have great news. This program is accredited by the CDR so all hours of instruction can be used to renew your CDCES regardless of your profession. **
The use of DES products does not guarantee the successful passage of the diabetes certification exams. CBDCE & ADCES does not endorse any preparatory or review materials for the certification exams, except for those published by CBDCE & ADCES.
**To satisfy the requirement for renewal of certification by continuing education for the Certification Board for Diabetes Care & Education (CBDCE), continuing education activities must be applicable to diabetes and approved by a provider on the CBDCE List of Recognized Providers (www.cbdce.org). CBDCE does not approve continuing education. Diabetes Education Services is accredited/approved by the Commission of Dietetic Registration which is on the list of CBDCE Recognized Providers.
by Christine Craig, MS, RD, CDCES
LT shared during a recent visit that over the past year, money to purchase food has become tight, and there are times when, by the end of the month, they do not have the resources to purchase more food.
From 2021 to 2022, the prevalence significantly increased by 2.6% within the US population. Food insecurity has racial inequities and has a higher incidence in American or Alaska Native, Black, Hispanic, or multiracial households.1 Children, older adults, individuals with increased diabetes complications, and individuals living in rural and urban areas are among the highest sub-populations at risk.

Food insecurity is defined as “the limited or uncertain availability of nutritionally adequate and safe foods or the inability to acquire foods in socially accepted ways.”2 Food insecurity and diabetes have a bi-directional relationship. Insecurity can lead to poor health, and poor health can reduce food access through loss of work/time at work, increased cost of medical care, and increased burden of disease.
Dietary intake and food access is strongly linked to health outcomes, and adults who experience food insecurity are two to three times more likely to develop type 2 diabetes.3 Reduced consumption of fruits, vegetables, and nutrient-dense foods increases the risk of insulin resistance and type 2 diabetes. For low-income individuals, studies3 have shown increased hospital ER visits and admissions for hypoglycemia during the last week of the month compared to earlier weeks. Financial constraints often force individuals to choose between purchasing medications and buying food.
The co-occurrence of diabetes and food insecurity is influenced by nutritional, mental health, and behavioral factors, according to the Weiser et al.2 conceptual framework. At the individual level, interventions targeting food security and diabetes should focus on these interconnected pathways, especially considering the impact of competing demands on self-care prioritization. People living with diabetes and food insecurity often experience increased diabetes distress, depression, and higher A1c levels. Additional challenges such as cost-of-living, transportation, and medication costs further exacerbate these outcomes. Addressing behavioral barriers may involve providing transportation assistance, social work case management, and comprehensive medical care, and ensuring a review of medication costs. Mental health interventions could involve integrating food access programs with mental health screening and referral services in addition to problem-solving and coping strategies to reduce diabetes distress. The most helpful nutrition interventions aim to improve food accessibility, offer person-centered and budget-friendly nutrition counseling, and address policies and programs that reduce diabetes risk and complications.
In 2023, the Department of Health and Human Services (HHS) developed the Food Is Medicine initiative, understanding that “access to nutritious food is critical to health and resilience.”3 The initiative focuses on developing strategies to reduce nutrition-related chronic disease and food insecurity while improving health and racial equity in the US.3 Food is Medicine can encompass many different programs, such as medically tailored meals, groceries, or produce prescription programs. Although A1C reduction results are mixed, each of these programs has shown an increase in fruit and vegetable consumption, food security, and quality of life measures.4
For individuals with diabetes, medically tailored meals result in the most evidence for improved diet quality, increased food security, improved diabetes self-management, and reduced hypoglycemic events.4 The programs are associated with lower health care utilization and cost for individuals with complex care needs. Medically tailored meals are designed by an RDN to meet the needs of the individual, are delivered directly to the home, and maybe a covered benefit if medical criteria are met. Seniors may access medically tailored and delivered programs through Medicare Advantage, Medicaid, or Area on Aging programs. Individuals who have chronic conditions and are post-hospital discharge have the highest likelihood of coverage. In California, Medi-Cal may provide up to three meals per day for twelve weeks for individuals with chronic health conditions (such as diabetes) who were recently discharged from a hospital or nursing home or require extensive care coordination. The Food is Medicine Coalition is a resource for additional information regarding Food is Medicine programs and can link individuals and providers to local participating agencies.
Interventions begin with screening and knowing that more individuals with diabetes will experience food insecurity compared to just one year ago. We can utilize risk assessment tools, including the hunger vital signs, at least annually during our visits and, with patient collaboration, provide referrals to assistance programs. The most extensive federal food assistance programs include the Supplemental Nutrition Assistance Program (SNAP) and the Special Supplemental Nutrition Program for Women, Infants, and Children (WIC). These programs are effective in increasing food security while also improving health outcomes. Reviewing eligibility and assisting in the coordination of services for Food Is Medicine programs, Nutrition Assistance Programs, and resources such as local food pantries, Meals on Wheels, or Area on Aging Agencies programs. www.Findhelp.org is a tool that can help individuals and providers find free or reduced- resources, from food to housing and more. Through assessment, understanding patient priority needs, and linking to resources, we can create a more supportive and therapeutic environment for individuals managing diabetes while experiencing food insecurity.

In our rural clinic, we are starting more and more individuals on glucose sensors. People’s response to using a CGM device has garnered mixed reactions. Most individuals are thrilled that they can see their blood sugars are at a glance with fewer finger pricks. They feel empowered with this play-by-play blood sugar report.
However, others experience a sense of overwhelm in response to the sudden onslaught of glucose data on their screen. This stress becomes more acute as they hone in on sugar spikes or sudden lows that don’t seem to have a rhyme or reason. In addition, many people are confused by the discrepancy between the meter and sensor glucose, causing even more upset.
These individuals may experience an understandable amount of confusion, frustration, and distress.
This newsletter provides a range of tools and resources to assist you in addressing these distress points, detailed in the following featured articles.
Our first article explores the reasons behind the gap between CGM and meter readings. We also provide a CGM Troubleshooting Cheat Sheet that you can share with your colleagues and clients.
Next, we outline a step-by-step communication approach designed to help individuals adjust to sensor data overwhelm using a person-centered approach.
Finally, we address diabetes distress by interviewing expert Susan Guzman, PhD. You are invited to join Dr. Guzman and Larry Fisher, PhD, who will share their expertise on this topic in June, during our highly popular ReVive 5 training program.
Our last article recognizes the healing relationship we have with our pets. Challenge yourself with our Question and Rationale of the Week and please keep in touch.
Sending notes of joy and health, Coach Beverly, Bryanna, and Christine |
Featured Articles
Upcoming Webinars
This two-session training provides the essential steps to address diabetes distress combined with an innovative approach to helping people make sense of their glucose data.
The first session is team-taught by experts in the field of diabetes distress and effective communication approaches. Dr. Larry Fisher kicks off the program by describing the difference between depression and distress and interpreting Diabetes Distress screening results. Dr. Susan Guzman uses a case study approach and step-by-step communication strategies to address responses from the Diabetes Distress screening tool. This session includes an abundance of evidence-based approaches that you can apply in your clinical setting.
Coach Beverly leads the second session. During this three-hour program, Beverly describes insulin dosing strategies, meter and sensor data interpretation, and common issues encountered by people using diabetes technology. Case studies include tools to help individuals discover what changes are needed to get glucose to target, coupled with the communication skills discussed in the first session. In conclusion, the team of instructors review a case study that pulls together all the ReVive 5 elements.
Can’t join live? That’s okay. Your registration guarantees you access to the recorded version of the series, along with podcasts and resources for one full year.
Accredited Training Program:
Join us to gain the confidence and learn the skills needed to support people with diabetes to move forward in their self-management and discover the expert within.
Team of Experts:
ReVive 5 is taught by a team of 3 Interdisciplinary Experts:
Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and our CPEU courses have received Prior Approval* from the Commission of Dietetic Registration (CDR), Provider DI002. Since our CPEU courses received Prior approval* from the CDR, these CPEU courses satisfy the CE requirements for the CDCES /BC-ADM regardless of your profession!
The use of DES products does not guarantee the successful passage of the certification exam. CBDCE and ADCES do not endorse any preparatory or review materials for the CDCES or BC-ADM exams, except for those published by CBDCE & ADCES.

RD is 82 years old, on basal insulin with bolus insulin at breakfast and dinner if need. RD just started using a sensor to track their daily blood sugars. After using the sensor for a few weeks, they share that they are feeling anxious and don’t know what to do with all this information. They even took extra bolus insulin yesterday to try and get blood sugars down. RD’s time in range is over 70%.
Which of the following is the most appropriate intervention?
This two-session training provides the essential steps to address diabetes distress combined with an innovative approach to helping people make sense of their glucose data.
The first session is team-taught by experts in the field of diabetes distress and effective communication approaches. Dr. Larry Fisher kicks off the program by describing the difference between depression and distress and interpreting Diabetes Distress screening results. Dr. Susan Guzman uses a case study approach and step-by-step communication strategies to address responses from the Diabetes Distress screening tool. This session includes an abundance of evidence-based approaches that you can apply in your clinical setting.
Coach Beverly leads the second session. During this three-hour program, Beverly describes insulin dosing strategies, meter and sensor data interpretation, and common issues encountered by people using diabetes technology. Case studies include tools to help individuals discover what changes are needed to get glucose to target, coupled with the communication skills discussed in the first session. In conclusion, the team of instructors review a case study that pulls together all the ReVive 5 elements.
Can’t join live? That’s okay. Your registration guarantees you access to the recorded version of the series, along with podcasts and resources for one full year.
Accredited Training Program:
Team of Experts:
ReVive 5 is taught by a team of 3 Interdisciplinary Experts:
Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and our CPEU courses have received Prior Approval* from the Commission of Dietetic Registration (CDR), Provider DI002. Since our CPEU courses received Prior approval* from the CDR, these CPEU courses satisfy the CE requirements for the CDCES /BC-ADM regardless of your profession!
The use of DES products does not guarantee the successful passage of the certification exam. CBDCE and ADCES do not endorse any preparatory or review materials for the CDCES or BC-ADM exams, except for those published by CBDCE & ADCES.
In celebration of Earth Day, we are excited to highlight the role of native plants in supporting wildlife and resilient environments.
By choosing plants that originated from your geographic area, we can help support regional ecosystem and offer pollinators, birds, butterflies and other healthy critters needed food, pollen and building materials for their survival. It’s good for humans too. We thrive in healthy ecosystems and experience improved quality of life.

When Coach Beverly first moved to her house 24 years ago, she just planted flowers and grasses that she found visually appealing and could tolerate the heat of our region. Her house and office are situated on an acre of land, so there was lots of space to plant a wide variety of foliage and trees to provide shade and beauty. But, she wasn’t yet tuned-in to the native plant and animal habitats of our new home.
Over time, Coach Beverly started learning about the impact habitat loss for creatures and pollinators. She researched which plants support the local area and found a nearby native nursery. Now, she and husband are working hard to make their land a nourishing and welcoming space for pollinators, birds, amphibians, lizards and more. With the help of a few great websites and a visit to the local native nursery, they incorporate plants that support their community of animals and are drought tolerant.
In addition to plants, providing a water source can be a game changer for thirsty pollinators, birds and others animals too. Simply placing a bowl of water, bird bath or even creating a small pond can make a big difference in supporting a variety of wild life. Last year, Coach Beverly dug a frog pond and within a few short weeks, frogs, toads and birds arrived to enjoy a drink, take a swim or a bath. A year later, our pond is teaming with tadpoles, mosquito fish, water beetles, dragonflies and lots of microscopic creatures. This lively pond brings family and visitors an abundance of joy and wonderment. Plus, they notice how connecting with nature improves mental health and helps with stress management and well being.
For people with diabetes or other chronic health issues, caring for plants and living beings can be very therapeutic and gratifying, and it doesn’t have to be complicated. Just take one step at a time. Start with potted herbs, plants, vegetables or flowers. Or through some wildflower seeds on a patch of untended earth and see what happens. For the more adventurous, planting a native garden is great excuse to get outside, bend, shovel and keep active. Plus, there is nothing like a fresh tomato warm from the vine that you have nurtured to frutition.
To get started, check out the article, Audubon – 20 Common Types of Native Plants, which includes a helpful list of 20 different native plants that support wildlife in the United States. You can cross-reference plants with your zip code finder above to see if these would be a good addition to your neighborhood. For example, in Chico, California, the California Christmas-Berry is a great food source for local birds and is drought tolerant.
In general, consider adding these native plants to your wish list:
Trees: Oaks, Pines, Dogwoods and Willows.
To bring color to your yard, porch or planters try planting Sunflowers or Coneflowers.
Treats for you and our bird friends include Blueberries, Elderberries, or Service berries.
The National Wildlife Federation (NWF) also provides a wonderful website, Native Plant Finder – NWF, to determine by zip code, native plants for your area. You can create and save your own personalized plant list too.
The Plant Native website, provides a listing of native nurseries throughout the U.S.
I also encourage you to visit www.Earthday.org and Project Regeneration for other great ideas to improve the health of our planet.
Many of us feel discouraged about what is happening to our planet, but there is a rising awareness of our impact and also a rising belief in our ability to protect this beautiful earth. Each action matters. Your action matters. And you can just start by planting one bush, flower, tree, plant or another acting on another idea that is meaningful to you. Thank you in advance for your action.

Each action, no matter how small, matters. We can do this!
With wishes for improved planetary health,
DiabetesEd Services Team
Accreditation: Diabetes Education Services is an approved provider by the California Board of Registered Nursing, Provider 12640, and our CPEU courses have received Prior Approval* from the Commission of Dietetic Registration (CDR), Provider DI002. Since our CPEU courses received Prior approval* from the CDR, these CPEU courses satisfy the CE requirements for the CDCES /BC-ADM regardless of your profession!
The use of DES products does not guarantee the successful passage of the certification exam. CBDCE and ADCES do not endorse any preparatory or review materials for the CDCES or BC-ADM exams, except for those published by CBDCE & ADCES.
Are you a diabetes health care professional or person with diabetes who is ready to get on track with your diabetes?
We want to encourage you to let your community know about an exciting research opportunity.
We are inviting people diagnosed with type 2 diabetes less than 5 years ago, who live anywhere in the U.S., with a most recent A1C of 7.5% or higher to click this link below to see if they qualify for the study.
If so, the Behavioral Diabetes Institute is conducting a research study examining how innovative new approaches to diabetes education might help to improve glucose outcomes and quality of life outcomes. Participants will be randomly assigned to take part in one of two different live, online, group education programs. Each group program will be lively and informative, and will meet once weekly for 5 weeks in a row.
Also, half of the participants will receive a continuous glucose monitor and free testing supplies.
To find out more and see if you might qualify, click below to apply. Or for more information, email them at [email protected] or call us at 858-336-8693.
People with diabetes experience a myriad of feelings as they utilize new technologies and try to make sense of all the data and new information. As diabetes healthcare providers, we can learn to address these feelings through person centered coaching and help individuals take steps to get to their best health. This approach not only acknowledges the individual’s feelings but also empowers them to take steps towards their optimal health.
This article equips healthcare professionals with a dozen practical coaching strategies. These strategies are designed to instill confidence in individuals with diabetes, fostering their belief in their ability to successfully self-manage their condition.

Using a person-centered approach, we can identify the individual’s strengths and expertise and then leverage this information to open a door of possibilities. Our choice of communication techniques can spark behavior change in people living with diabetes.
Adopting a person-centered approach may require a significant adjustment for some healthcare providers. In traditional care, the provider assumes the role of the captain, steering the ship, providing the fuel, and plotting the course. However, in person-centered coaching, the provider becomes the rudder, guiding the individual while they steer their own course towards better health.
For this conversation, we imagine someone struggling with technology-related diabetes distress after switching from checking blood sugars using a meter to trying to make sense of the data being generated by their new CGM.
DO: Mindfully Listen to the individuals’ problems and fears.
The first strategy is carefully listening to the person’s fears and concerns. If someone struggles with nutrition, meds, or behavioral changes, listen to the struggle and try not to push, advise, or fix it. Listen and reflect on what you think is happening for the first few minutes.
For example, reflecting back could go something like this:
“Taking insulin each meal is hard for you because you are worried about taking too much.” OR
“It’s hard not to constantly check your blood sugar on your CGM because you are worried that it is going above range.” OR
“It sounds like you blame yourself for having blood sugars that are above target.”
Listening and reflecting on the individual’s struggles is the first phase of energizing the visit.
DO: Focus on curiosity before exploring possible changes in behavior.
With a person-centered approach, spend more time in the “curiosity” phase before moving to the “action” phase.”
We might ask the person who feels worried about elevated blood sugars, “I am curious to learn more about your feelings when blood sugars go above target.”
As care providers, we may be slightly overanxious to get to the “action” phase, which involves action, planning, goal setting, and looking at specific foods and exercise prescriptions. It can be disorienting for providers to delay the “action” phase and spend most of the time exploring the “curiosity” phase, and there’s a perception that it takes longer. In fact, it’s probably more efficient with time. It’s a redistribution of the provider’s time in that more time is spent listening to the individual’s barriers and fears and responding to them.
Curiosity can provide comfort and open the door to insights.
DO: Listen for individual insights and ideas.
After reflecting on the person’s struggles and feelings, the next phase is the “building change” talk. It combines having the person express how a behavior change would benefit them and realistic ways to move to the action phase.
As genuinely curious providers, we ask, “What are your ideas about how you can improve this situation?” Then, the provider listens carefully to what the person shares.
Along with the struggles and barriers, the individual might say,
“I will try only to check my blood sugar levels before meals and two hours after a meal instead of twenty times a day” or
“I could try adjusting my insulin dose for a week to see how that affects my blood sugars.”
We want to fine-tune our listening skills so that we can pick up the scent of the trail. People often allude to what they’re willing to do and drop crumbs when they feel safe and heard during the conversation. All we need to do is pick up on the hints and encourage them down the path.
DO: Ask Questions and Collaborate.
Once the individual has identified their motivation and begins brainstorming ways to change behavior, the door is open for respectful collaboration. You’ll want to explore how much change the individual is willing and able to make at that time.
To keep it real and achievable, we start with a tiny step by saying,
“So, you think you could limit checking your blood sugars to about eight times a day?” or
“You think you could adjust your insulin dose for a week to see if that lowers post-meal blood sugars?” Let that sit; let the person describe their thoughts and feelings.
Then we might say, “How, if at all, do you see this plan fitting into your life?” We are careful to avoid any prescription or declaration and stick with asking questions.
If they volunteer—”I will limit checking my blood sugars on my CGM to eight times a day.” Or
“I will adjust my insulin dose to see if it lowers my post-meal blood sugars.”
We would absolutely reinforce and support these choices.
AVOID: Pressure, fix, or control.
A person-centered approach energizes individuals to take the lead in managing their condition, in step with their providers and supporters. We are careful to avoid forced solutions or controlling language. As providers, we feel we have these great ideas that will fix the person, if only…. However, the truth is, our job is to help the person with diabetes find their own answers and solutions.
Let’s stop “Shoulding” on people.
It’s time to let go of terms like “You must, you should, you have to, it’s better, it’s important, do it for me” since they fall under the category of “controlling motivation”—which can be hurtful and lead to the individual becoming defensive or shutting down. We avoid controlling language because it elicits resistance and defiance. The literature is quite clear about people doing something because someone made them feel guilty, ashamed, or pressured them. The long-term prognosis for behavior change using this approach is underwhelming.
DON’T employ Scare Tactics.
As providers, we genuinely care about people’s health and may try to energize behavior change using fear. Such as, “If you don’t get your A1C down, you are heading for dialysis or amputation.” or “Don’t you want to see your kids grow up?” We don’t generally motivate people by scaring them since research shows it is ineffective, and they may never return for that follow-up appointment.
In the short term, people are usually willing to make changes when they’re terrified—when they first get diagnosed—but that willingness wanes in a relatively short period. The question is how to energize the person when the initial fear has worn off.
In conclusion, Celebrate and Recognize Each Person’s Efforts.
Making behavior changes, like losing weight or adjusting lifelong eating habits, can be extremely difficult.
Find a way to recognize and affirm their efforts even if there is no or little change in clinical measures.
If someone’s A1C has not moved, but they decreased their CGM checks to eight times a day or adjusted their mealtime insulin, we can say, “Wow, I want to recognize the effort you put into this.”
Respond kindly and compassionately to their disappointment, frustration, and fear. It won’t fix the immediate problem but will help the person feel that their effort was well spent. It will help them feel heard instead of us just “fixing it.” Over time, your empathy will build bridges and trust, leading to long-term collaboration and better health.
Download a PDF of this Person Centered Step-By-Step Approach
About the author – Coach Beverly has been fine-tuning her guilt-free approach to diabetes education for over 30 years and has witnessed its impact on improving well-being and building connections.
Learn more about these effective communication approaches in our ReVive 5 Training Program.
Inspired by https://www.niddk.nih.gov/health-information/professionals/diabetes-discoveries-practice/motivational-interviewing-dos-dont

This two-session training provides the essential steps to address diabetes distress combined with an innovative approach to helping people make sense of their glucose data.
The first session is team-taught by experts in the field of diabetes distress and effective communication approaches. Dr. Larry Fisher kicks off the program by describing the difference between depression and distress and interpreting Diabetes Distress screening results. Dr. Susan Guzman uses a case study approach and step-by-step communication strategies to address responses from the Diabetes Distress screening tool. This session includes an abundance of evidence-based approaches that you can apply in your clinical setting.
Coach Beverly leads the second session. During this three-hour program, Beverly describes insulin dosing strategies, meter and sensor data interpretation, and common issues encountered by people using diabetes technology. Case studies include tools to help individuals discover what changes are needed to get glucose to target, coupled with the communication skills discussed in the first session. In conclusion, the team of instructors review a case study that pulls together all the ReVive 5 elements.
Can’t join live? That’s okay. Your registration guarantees you access to the recorded version of the series, along with podcasts and resources for one full year.
Accredited Training Program:
Team of Experts:
ReVive 5 is taught by a team of 3 Interdisciplinary Experts:
The use of DES products does not guarantee the successful passage of the certification exam. CBDCE and ADCES do not endorse any preparatory or review materials for the CDCES or BC-ADM exams, except for those published by CBDCE & ADCES.