
Subscribe
eNewsletter

Ready to get certified?
Free CDCES Coach App
Download
Free Med Pocket Cards

eNewsletter

Free CDCES Coach App
Free Med Pocket Cards

The American Diabetes Association estimates that over 8 million people in the United States depend on insulin therapy for survival.¹ Multiple daily injections (MDI) of insulin can be challenging to manage. Diabetes care and education specialists understand that complex medication regimens often lead to difficulty achieving medication adherence and worsening glycemic control.²
CeQur Simplicity is a unique alternative to MDI therapy. It redefines insulin delivery with a wearable device that administers insulin with just a few clicks. By simplifying insulin delivery, CeQur can support successful insulin management and improve glycemic control without the hassle of multiple daily injections.
The CeQur Simplicity patch is a wearable insulin delivery device for adults aged 21 and older, approved for individuals with type 1 or type 2 diabetes who require insulin. This thin patch can hold up to 200 units of either U-100 lispro (Humalog) or U-100 aspart (Novolog) insulin. The patch can be used for up to 4 days on any approved insulin injection site. It is usually worn on the abdomen, thigh, or upper arms, as these areas are more accessible for reaching the CeQur device.³
Pressing the buttons on the sides of the device delivers two units of insulin. Each press produces an audible click to announce delivery. Over the 4-day wear period, this wearable insulin device replaces up to twelve meal bolus injections. The ease of use and ability to dose without carrying and storing insulin or injecting it can be freeing for many people living with diabetes. Research has found that when using the CeQur patch, users were more satisfied with the device, experienced less diabetes-related burden, and missed fewer insulin boluses.
CeQur is not an automated insulin delivery system. This device operates independently and does not connect to continuous glucose monitors. The CeQur Simplicity is not approved for basal insulin and does not replace the need for basal insulin.
Diabetes healthcare professionals can help identify clients who may benefit from the CeQur Simplicity insulin patch. An ideal CeQur candidate may be those who:
The healthcare professional’s (HCP) role starts with explaining the CeQur Simplicity device and how it differs from traditional insulin pumps and insulin pens. Besides identifying those who may benefit from CeQur, the HCP also provides training and troubleshooting for CeQur. CeQur training includes demonstrating how to apply and remove the device, using the click-based bolus feature, and performing site care and rotation procedures. This hands-on education helps clients build confidence in their new insulin delivery device. HCP’s can also assist in exploring cost, insurance coverage, and manufacturer support programs.
Here are other considerations for the diabetes healthcare professional:
✅ Assess the ability to count by 2s as the device only delivers doses in increments of 2 units.
✅ Fill the CeQur device with insulin just before use and never prefilled in advance.
✅ Do not apply a CeQur insulin patch near the area where basal insulin is injected.
✅ Avoid applying the insulin patch to areas that will be irritated by clothing, accessories, or a seat belt.
✅ Use the ‘Change By’ sticker provided with each device as a reminder of when the device needs to be changed.
✅ Avoid submerging the patch more than 3 feet 3 inches (1 meter). Also, do not squeeze the dosing buttons while the patch is underwater.³
Diabetes healthcare professionals work to identify and address barriers to insulin therapy. Collaborating with clients can boost their confidence, foster effective diabetes self-management, and improve their psychological outcomes. For those who are frustrated with their current MDI therapy but are also leery of AID systems, the CeQur Simplicity insulin patch may offer fewer injections, freedom from carting around meal-time insulin, and an improved quality of life.
References

RT has type two diabetes and has been maintaining a time and range of 70% or greater. However, when they show up at the office, the last week’s time in range dropped to 30%. You ask what was different this week from the previous few months. RT tells you they went on a five day fishing trip and forgot their insulin.
What’s the best response?

Level 5 | Beyond Blood Glucose: Empowering Health Through a Holistic Lens with:
Speaker Nick Kundrat, BS, CEP, CDCES, LMT
For last week’s practice question, we quizzed participants on FIB-4 of 2.83. 48.09% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it below: Answer Question

AR lives with type 2 diabetes, and their waistline is 41 inches. Since their ALT and AST levels are elevated, you know they are at risk for steatosis (MASH). You quickly calculate their Fibrosis-4 Index (FIB-4), by plugging in AR’s Age, AST, ALT, platelet count into the FIB-4 calculator. AR’s result is 2.83.
According to the ADA Standards, with a FIB-4 value of 2.83, which action is required?
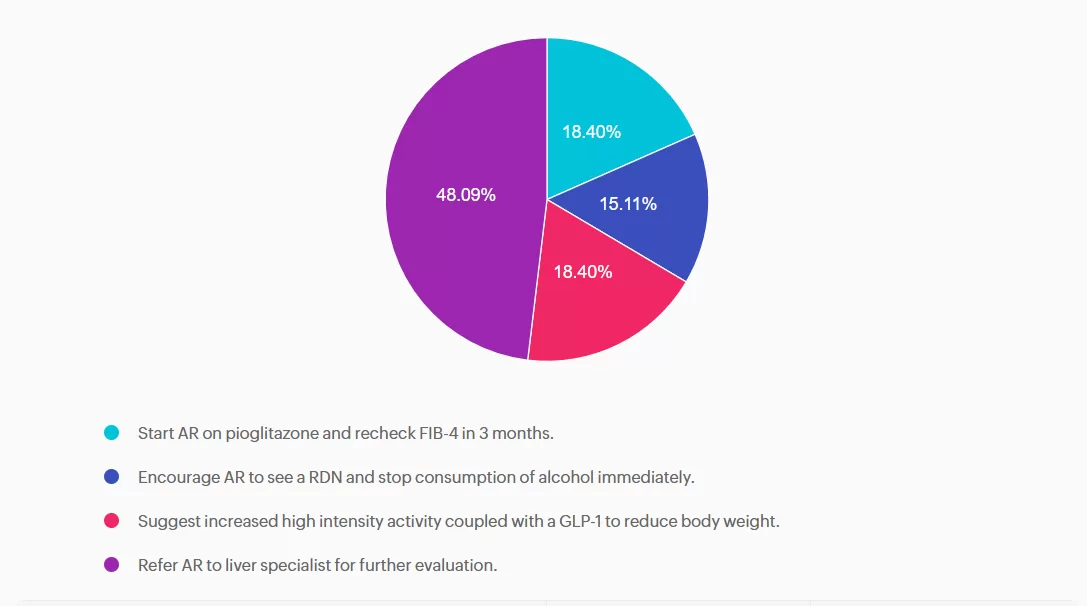
Answer A is incorrect: 18.4% chose this answer, “Start AR on pioglitazone and recheck FIB-4 in 3 months.” Although pioglitazone is a recommended treatment for steatosis, since AR’s FIB- is greater than 2.67, this indicates AR is at high risk for advanced fibrosis and a referral to a liver specialist is warranted.
Answer B is incorrect: 15.11% chose this answer, “Encourage AR to see a RDN and stop consumption of alcohol immediately.” Seeing a RDN is very important for AR to evaluate and customize an eating plan to address their steatosis and support quality of life. However, since AR’s FIB- is greater than 2.67, this indicates AR is at high risk for advanced fibrosis and a referral to a liver specialist is warranted.
Answer C is incorrect: 18.4% chose this answer, “Suggest increased high intensity activity coupled with a GLP-1 to reduce body weight.” Strength training and activity, coupled with a GLP-1 for GLP-1/GIP are important strategies to address steatosis. However, since AR’s FIB- is greater than 2.67, this indicates AR is at high risk for advanced fibrosis and a referral to a liver specialist is warranted.
Answer D is correct: 48.09% chose this answer, “Refer AR to liver specialist for further evaluation.” Great job! AR will require intensive intervention to decrease their risk of worsening steatosis, including MNT, targeted activities, and a referral to a liver specialist to determine the best treatment approach.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!


Two out of three individuals with type 2 diabetes are affected by liver steatosis.¹ In May 2025, the American Diabetes Association (ADA) published a consensus report, which emphasized recommendations for early diagnosis, long-term monitoring, and highlighted lifestyle interventions as critical in preventing progression to cirrhosis.¹
In the past year, two medications have been approved for the treatment of MASH; however, lifestyle change remains at the foundation of treatment. These changes focus on improving dietary quality, increasing physical activity, promoting weight loss, and reducing sedentary behaviors.
Nutrition therapy, ideally guided by a registered dietitian nutritionist and reinforced by the entire diabetes care team, needs to be individualized to each person’s social, cultural, and financial needs.¹ Ivancovsky Wajcman et al. ² published a fascinating review of different country’s MASLD management guidelines summarizing recommended lifestyle interventions, their findings indicated many similarities with only a few differences.
Most groups recommended evidence-based eating patterns with the following themes:
The Mediterranean diet eating pattern is recommended in the MASLD/MASH ADA consensus report as well as the EASL–EASD–EASO Clinical Practice Guidelines ¹,²,³ due to its relationship with improving diet quality and evidence of hepatic and cardiovascular health benefits, even without weight loss.
Other dietary patterns, such as the low-fat, low-carbohydrate, Dietary Approaches to Stop Hypertension, high protein, meal replacement, and intermittent fasting, have also been shown to be comparable strategies to improve steatosis due to weight loss.¹
In people with overweight and obesity, the magnitude of weight loss has been associated with improving glycemic management, insulin sensitivity, as well as histological improvements in MASH.¹
Weight reduction over 5% has been associated with reduced steatosis, and greater weight loss of 7-10% has been shown to reverse steatohepatitis and liver fibrosis.¹,²,³ However, it is recognized that achieving long-term weight reduction may be challenging.³
Avoidance of alcohol is recommended for individuals with moderate fibrosis, as even modest use may aggravate injury.
Physical activity, including aerobic and resistance training, has independent effects beyond weight loss: decreasing intrahepatic fat, improving cardiovascular risk, improving insulin sensitivity, and supporting weight‐loss maintenance. Guidelines generally recommend greater than or equal to 150 minutes per week of moderate intensity (or equivalent) and resistance activities 2-3 times per week, with greater benefit when increasing activity.
However, reducing sedentary time and breaking up prolonged sitting bouts can be effective ways to reach this goal.¹,³ Emerging evidence highlights the importance of stress reduction, adequate sleep and treatment of sleep apnea, and management of comorbidities such as dyslipidemia and hypertension, due to their impact on liver steatosis, inflammation, and fibrosis.¹,²
Until recently, there were no FDA-approved medications specifically for MASH; treatment was either off-label or targeted at comorbidities such as weight reduction or lipid and glycemic management. However, in the past 2 years, two different medications have been released to address MASH. In March 2024, the FDA approved resmetirom (brand name Rezdiffra) for adults with noncirrhotic MASH to be prescribed in conjunction with lifestyle therapy. 4 In August 2025, the FDA approved semaglutide (brand name Wegovy) for the treatment of MASH and moderate to advanced liver fibrosis. 5
MASLD and MASH are high-risk health conditions for people with diabetes, with approximately 10-30% progressing to advanced liver disease, including cirrhosis.³ While new FDA-approved medications such as resmetirom and semaglutide offer promising options, lifestyle modification remains a cornerstone treatment.
As diabetes healthcare professionals, we are uniquely positioned to implement evidence-based strategies into the individualized care plan.
We can screen, educate, and empower individuals living with diabetes to take proactive steps that protect liver health, improve metabolic outcomes, and prevent progression to cirrhosis. Through nutrition and lifestyle therapy, pharmacotherapy, and incorporating broad strategies into DSMES services (¹) we can strengthen prevention and outcomes.
References

Explore the magnificent world of diabetes and the gut — from periodontal disease to the microbiome and everything in between.
Join Coach Beverly Thomassian, RN, MPH, CDCES, BC-ADM, for a fascinating journey through gastrointestinal health from top to bottom. This course covers fatty liver disease, gastroparesis, intestinal complications of diabetes, the gut microbiome, and more — giving you the knowledge to better support whole-body health.

Kyle is a 55-year-old man with type 2 diabetes for ten years. He was recently diagnosed with retinopathy in both eyes. His grandmother lost her eyesight due to diabetes. Due to this family history, he is very concerned about his new diagnosis. He uses a Libre continuous glucose monitor (CGM) to monitor his blood sugar levels. During your visit, he is preoccupied with checking his Libre CGM and tells you that he uses his glucometer to verify CGM readings at least four to six times per day. When you ask him about this, he reports that he can’t focus on his work or home life if he isn’t over 90% time in range.
As a diabetes care and education specialist, what is the best approach to this situation?
For last week’s practice question, we quizzed participants on FDA approved treatment for MASH. 33.75% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it below: Answer Question

MJ just discovered that in addition to their type 2 diabetes and a BMI of 31, they also have MASH.
Based on this diagnosis, which FDA approved medication would help address their steatosis?
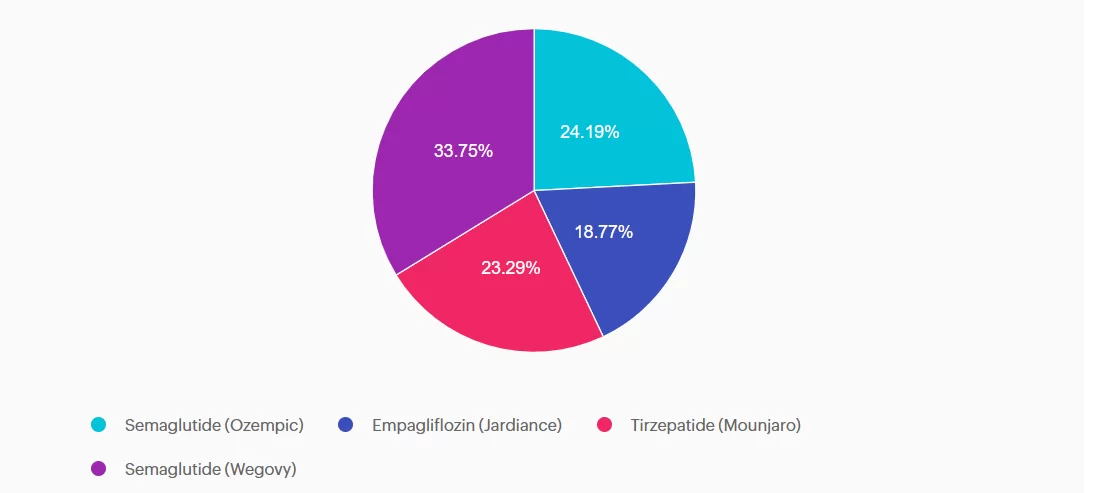
Answer A is incorrect: 24.19% chose this answer, “Semaglutide (Ozempic).” The diabetes approved version of semaglutide (Ozempic) does not yet have FDA approval as a medication that is used for treatment of MASH.
Answer B is incorrect: 18.77% chose this answer, “Empagliflozin (Jardiance).” Although empagliflozin will reduce blood glucose and can help with weight loss, it is not FDA approved for treatment of MASH.
Answer C is incorrect: 23.29% chose this answer, “Tirzepatide (Mounjaro).” Tirzepatide (Mounjaro) is approved for treatment of diabetes, helps with weight loss and is FDA approved for sleep apnea. However it is not FDA approved for treatment of MASH.
Answer D is correct: 33.75% chose this answer, “Semaglutide (Wegovy).” The weight loss approved version of semaglutide (Wegovy) has FDA approval as a medication that is used for treatment of MASH.
Please see our new “Indications for GLP-1/GIP” Cheat Sheet for a complete run down.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!

🌟Updated Schedule: ADA Boot Camp, Tech, MNT & More
Live in Beautiful San Diego – Oct 22-23, 2026
Re-Ignite your Passion & Prepare for Diabetes Certification Exams
🎓 Earn 30+ CEs: AMA PRA Category 1 Credits™, ACPE, ANCC, and CDR!
📅
2-Day Conference
Oct 22–23, 2026
⏱️
15.5 Live CEs
+ 17 bonus CEs
🏅
CDCES & BC-ADM
Exam Prep + Renewal
📍
San Diego, CA
1.7 mi from airport
The field of diabetes care is expanding and evolving rapidly. This unique training conference will keep you on the cutting edge plus prepare you for certification exams. It also fulfills the Standards of Care renewal requirement. Join us for two days of intensive education that is fun and inspiring. Add on the optional Day 3 (Engaging the Disengaged), to complete your conference exeperience.
Coach Beverly and Diana Isaacs, PharmD, BC-ADM, CDCES co-lead an exciting day that brings the ADA and AACE Standards to life. Gain fresh insights, practical tools, and a deeper understanding of the latest in person-centered diabetes care. After attending, you will be empowered to share the latest in diabetes care with your colleagues and the people in your care.
Take your knowledge to the next level with this intensive deep-dive into insulin therapy, dosing and pattern management with Dr. Diana Isaacs. Next, stay for the diabetes tech show-and-tell as Diana demonstrates the specs of the latest pumps and sensors. After lunch, nutrition whiz Christine Craig, MS, RDN, CDCES expertly details the latest in MNT and provides real strategies on translating this content to your clinical practice. You will have a chance to put it all together as Coach Beverly leads you through a series of case studies that integrates content from Day 1 and Day 2.
On Saturday, join this exceptional day-long program led by William H. Polonsky, PhD, CDCES & Susan Guzman, PhD (Behavioral Diabetes Institute) that reveals psychosocial forces behind diabetes self-management — tools to break through resistance and inspire change.
Read more below
📜 Essentials
Registration
+ Printed Syllabus
$559.00
🌟 Deluxe
Essentials
+ ADA Standards Book
$589.00
🏆 Complete – Best Value!
Deluxe
+ ADCES Review Guide e-Book
$669.00

Transform how you engage patients with diabetes — master behavior change, reduce distress, and overcome medication hesitancy.
Why do so many patients know what they should do — but still struggle to do it?
The answer lies in the psychology of diabetes.
In this transformative full-day course, world-renowned experts William H. Polonsky, PhD, CDCES, and Susan Guzman, PhD, from the Behavioral Diabetes Institute reveal the hidden psychosocial forces that drive — or derail — diabetes self-management.
You’ll walk away with a completely new toolkit for breaking through patient resistance, dissolving medication hesitancy, and creating clinical encounters that actually inspire change!

AR lives with type 2 diabetes, and their waistline is 41 inches. Since their ALT and AST levels are elevated, you know they are at risk for steatosis (MASH). You quickly calculate their Fibrosis-4 Index (FIB-4), by plugging in AR’s Age, AST, ALT, platelet count into the FIB-4 calculator. AR’s result is 2.83.
According to the ADA Standards, with a FIB-4 value of 2.83, which action is required?

🌟Updated Schedule: ADA Boot Camp, Tech, MNT & More
Live in Beautiful San Diego – Oct 22-23, 2026
Re-Ignite your Passion & Prepare for Diabetes Certification Exams
🎓 Earn 30+ CEs: AMA PRA Category 1 Credits™, ACPE, ANCC, and CDR!
📅
2-Day Conference
Oct 22–23, 2026
⏱️
15.5 Live CEs
+ 17 bonus CEs
🏅
CDCES & BC-ADM
Exam Prep + Renewal
📍
San Diego, CA
1.7 mi from airport
The field of diabetes care is expanding and evolving rapidly. This unique training conference will keep you on the cutting edge plus prepare you for certification exams. It also fulfills the Standards of Care renewal requirement. Join us for two days of intensive education that is fun and inspiring. Add on the optional Day 3 (Engaging the Disengaged), to complete your conference exeperience.
Coach Beverly and Diana Isaacs, PharmD, BC-ADM, CDCES co-lead an exciting day that brings the ADA and AACE Standards to life. Gain fresh insights, practical tools, and a deeper understanding of the latest in person-centered diabetes care. After attending, you will be empowered to share the latest in diabetes care with your colleagues and the people in your care.
Take your knowledge to the next level with this intensive deep-dive into insulin therapy, dosing and pattern management with Dr. Diana Isaacs. Next, stay for the diabetes tech show-and-tell as Diana demonstrates the specs of the latest pumps and sensors. After lunch, nutrition whiz Christine Craig, MS, RDN, CDCES expertly details the latest in MNT and provides real strategies on translating this content to your clinical practice. You will have a chance to put it all together as Coach Beverly leads you through a series of case studies that integrates content from Day 1 and Day 2.
On Saturday, join this exceptional day-long program led by William H. Polonsky, PhD, CDCES & Susan Guzman, PhD (Behavioral Diabetes Institute) that reveals psychosocial forces behind diabetes self-management — tools to break through resistance and inspire change.
Read more below
📜 Essentials
Registration
+ Printed Syllabus
$559.00
🌟 Deluxe
Essentials
+ ADA Standards Book
$589.00
🏆 Complete – Best Value!
Deluxe
+ ADCES Review Guide e-Book
$669.00

Transform how you engage patients with diabetes — master behavior change, reduce distress, and overcome medication hesitancy.
Why do so many patients know what they should do — but still struggle to do it?
The answer lies in the psychology of diabetes.
In this transformative full-day course, world-renowned experts William H. Polonsky, PhD, CDCES, and Susan Guzman, PhD, from the Behavioral Diabetes Institute reveal the hidden psychosocial forces that drive — or derail — diabetes self-management.
You’ll walk away with a completely new toolkit for breaking through patient resistance, dissolving medication hesitancy, and creating clinical encounters that actually inspire change!
For last week’s practice question, we quizzed participants on Lifestyle Therapy for MASLD and MASH. 83% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it below: Answer Question

PJ has had type 2 diabetes for 8 years and is here for a follow-up visit. Labs indicate A1c at 7.2%, lipids at target, eGFR of 78 mL/min/1.73m², and urine albumin-to-creatinine ratio (UACR) of 65 mg/dL. Blood pressure at the office visit today was 142/86, which is consistent with home monitored values. PJ confirms taking medications, metformin and simvastatin. PJ inquires about recently completed lab work.
According to the ADA Standards of Care, what would be an appropriate next step in the diabetes care plan?
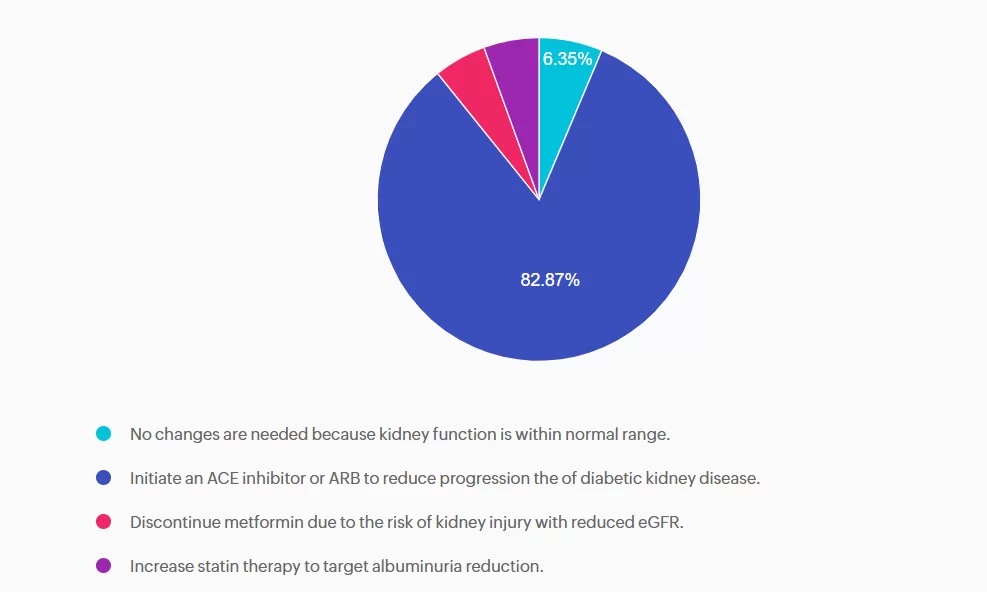
Answer A is incorrect: 6.35% chose this answer, “No changes are needed because kidney function is within normal range.” A is incorrect. Although eGFR indicates stage 2 kidney disease, the elevated UACR, ≥30 mg/g, confirms moderately increased risk and recommendation to treat. Additionally, PJ’s blood pressure is also above the target. Intervention is needed to protect kidney and cardiovascular health.
Answer B is correct: 83% chose this answer, “Initiate an ACE inhibitor or ARB to reduce progression the of diabetic kidney disease.” PJ has a mildly decreased eGFR, but UACR is elevated above 30 mg/g, indicating a recommendation to treat. Additionally, intervention is needed to optimize blood pressure. According to the ADA Standards of Care in Diabetes, individuals with diabetes, hypertension, and moderately increased albuminuria should be treated with an ACE inhibitor or angiotensin receptor blocker. The use of sodium-glucose cotransporter 2 (SGLT2) inhibitors or glucagon-like peptide 1 agonists (GLP1-RA), with demonstrated benefits, could also be considered to reduce CKD progression.
Answer C is incorrect: 5.25% chose this answer, “Discontinue metformin due to the risk of kidney injury with reduced eGFR.” Metformin is safe to continue unless eGFR falls below 30 30 mL/min/1.73m². PJ’s kidney function is adequate for continued use. However, consideration to add a change to SGLT2 or GLP1 with kidney benefit could also promote additional A1c reduction.
Answer D is incorrect: 5.52% chose this answer, “Increase statin therapy to target albuminuria reduction.” Statins are recommended for ASCVD prevention, but they do not reduce albuminuria. Lipids are within normal range, and albuminuria should be addressed with an ACE inhibitor/ARB or potentially a SGLT2 inhibitor or GLP-1 RA.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!

Explore the magnificent world of diabetes and the gut — from periodontal disease to the microbiome and everything in between.
Join Coach Beverly Thomassian, RN, MPH, CDCES, BC-ADM, for a fascinating journey through gastrointestinal health from top to bottom. This course covers fatty liver disease, gastroparesis, intestinal complications of diabetes, the gut microbiome, and more — giving you the knowledge to better support whole-body health.