
Subscribe
eNewsletter

Ready to get certified?
Free CDCES Coach App
Download
Free Med Pocket Cards

eNewsletter

Free CDCES Coach App
Free Med Pocket Cards
For last week’s practice question, we quizzed participants on Sleep and ADA Recommendations. 71% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it below: Answer Question

Question:
A 62-year-old with type 1 diabetes presents for their follow-up visit. They report struggling with fatigue, poor sleep quality, and difficulty with glucose management despite taking medications as prescribed. Upon review, you find their A1C is 7.6%, and their average nightly sleep duration is 4.5-6 hours per night.
Based on the 2025 ADA Standards of Care, which of the following interventions would be the most appropriate next step to address sleep and glucose management?
Answer Choices:
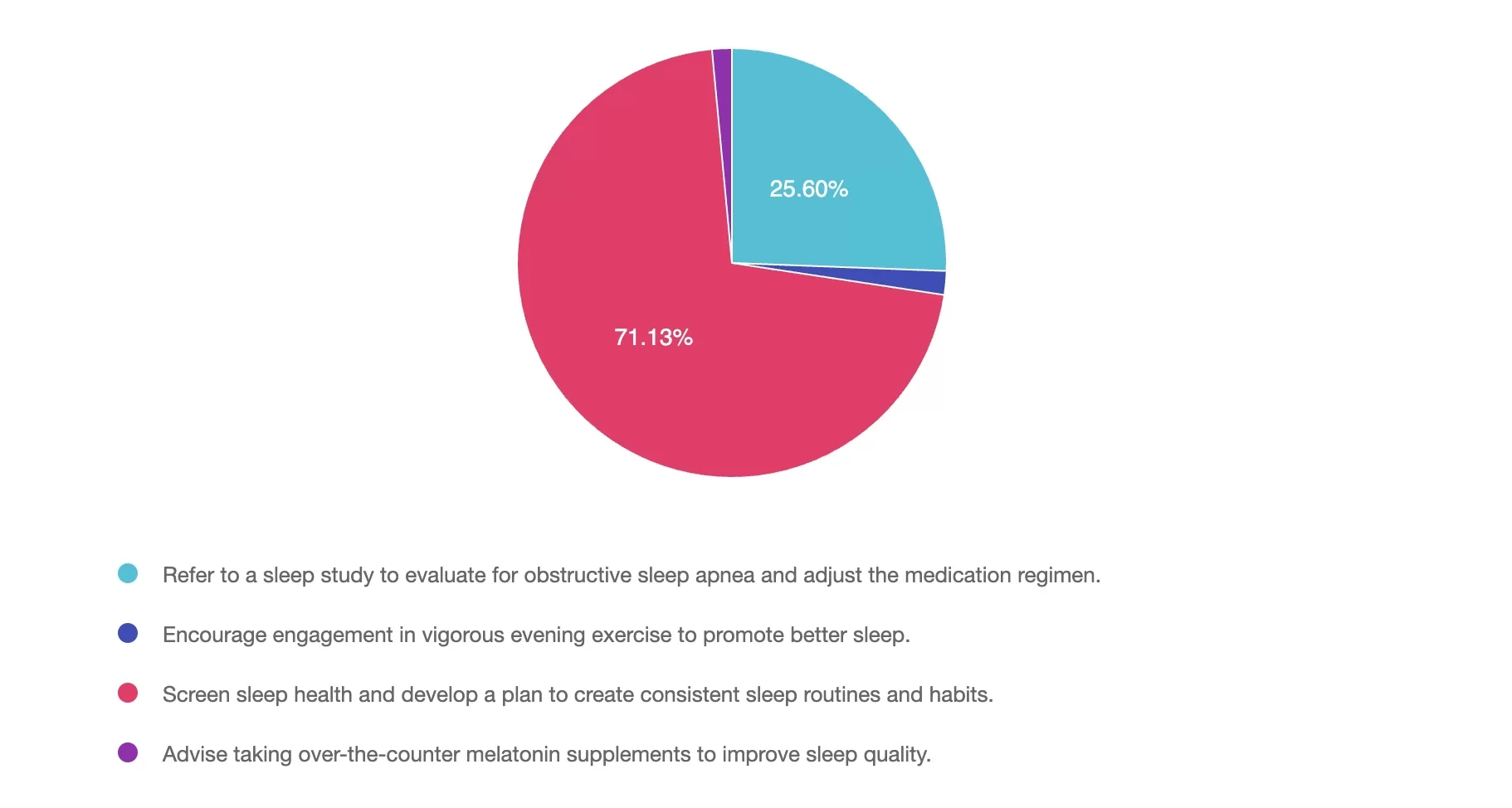
Answer 1 is incorrect. 25% chose this answer, “Refer to a sleep study to evaluate for obstructive sleep apnea and adjust the medication regimen.” While a sleep study may be recommended for suspected sleep disorders, such as sleep apnea (for example: loud snoring, daytime sleepiness), the first step should be a comprehensive sleep health screening. This screening helps identify potential causes of poor sleep, including symptoms of sleep disorders, disruptions from diabetes management (for example: nocturnal hypoglycemia, frequent urination), or anxiety about sleep. Based on the findings, appropriate treatment modifications and referrals can then be made.
Answer 2 is incorrect. 1% of you chose this answer, “Encourage engagement in vigorous evening exercise to promote better sleep.” Although exercise can improve sleep quality, vigorous evening exercise may increase alertness, making it harder to fall asleep. In individuals with type 1 diabetes, this timing of exercise can also increase the risk of nighttime hypoglycemia, further disrupting sleep. Before recommending vigorous exercise, it’s important to first assess sleep habits to better understand the underlying causes of poor sleep quality.
Answer 3 is correct. About 71% of respondents chose the BEST ANSWER – GREAT JOB! “Screen sleep health and develop a plan to create consistent sleep routines and habits.” The 2025 ADA Standards emphasize the importance of screening for sleep health and providing guidance on sleep-promoting routines and habits. Based on screening results, referrals to sleep medicine programs, adjustment in medications or behavioral therapy programs are a few that may be appropriate. Prioritizing improved sleep duration and consistency can support better glucose management, reduce fatigue, and enhance overall well-being.
Finally, Answer 4 is incorrect. 1% chose this answer, “Advise taking over-the-counter melatonin supplements to improve sleep quality.” While melatonin may be helpful for certain sleep disorders, its use should be evaluated on a case-by-case basis and is not recommended within the ADA 2025 Standards of Care. The first-line recommendation should focus on screening to better determine appropriate actions.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!

The use of DES products does not guarantee the successful passage of the certification exam. CBDCE and ADCES do not endorse any preparatory or review materials for the CDCES or BC-ADM exams, except for those published by CBDCE & ADCES.

Spring into New Course Offerings!
You are gonna love this new course bundle we are officially launching – today. This new Level 5 Expert-led Series, designed for HCPs committed to staying at the leading edge of this fast-evolving field, is ready. Featuring a dynamic and diverse faculty of top experts and educators, each session explores timely, advanced topics—such as emerging therapies, nutrition, integrating new technologies, and addressing social determinants of health. Join us to sharpen your clinical skills, broaden your care strategies, or drive innovation.
Also, if you are taking the CDCES or BC-ADM exam this year, you won’t want to miss our FREE Behavior Change Theories Made Easy webinar. Coach Bev will save you hours of studying tedious theories and provide you with a summary of the information you need to know for exam success.
There is still time to sign up for our ADA Standards Webinars. Don’t worry if you can’t make it live. Once you register, you can access the recorded version for a year. Save 10% on our online courses, by entering coupon code Success10 at checkout.
With love,
Coach Beverly, Bryanna, Tiffany, Christine, & Katarina


BT was started on a GLP-1 and is losing weight. BT has read articles about the importance of strength training to maintain muscle. They ask you questions about whether using weights or resistance bands is better.
According to the transtheoretical model, what stage of change is BT in?

Keeping all the behavior change and learning theories straight can be daunting, especially if you are trying to get to the “best” answer for certification exams. Coach Beverly feels your pain and wants to help out. To say thanks for 25 years, she’s hosting a FREE Behavior Change Webinar to sort out and dissect the theories most relevant in clinical practice and for exam preparation.
All hours earned count toward your CDCES Accreditation Information
The use of DES products does not guarantee the successful passage of the certification exam. CBDCE and ADCES do not endorse any preparatory or review materials for the CDCES or BC-ADM exams, except for those published by CBDCE & ADCES.

The Virtual Conference starts next week. If you haven’t secured your spot yet, this is your final opportunity to register and join us.
Gain fresh insights, practical tools, and a deeper understanding of the latest in person-centered diabetes care. Our expert team brings the ADA Standards of Care to life—covering medications, behavior change, technology, and more! If you’re preparing for the CDCES or BC-ADM exam, this conference—paired with free bonus courses—serves as the ideal study companion!
With interactive co-teaching, we keep sessions engaging, relevant, and fun. Let’s learn and grow together!

Our expert team transforms complex diabetes science into clear, practical insights—keeping it real, engaging, and fun! The faculty includes:
The use of DES products does not guarantee the successful passage of the certification exam. CBDCE and ADCES do not endorse any preparatory or review materials for the CDCES or BC-ADM exams, except for those published by CBDCE & ADCES.
For last week’s practice question, we quizzed participants on Remote Eye Screening Precautions. 84% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it below: Answer Question

Retinal photography with remote reading by experts has great potential to provide screening services in areas where qualified eye care professionals are not readily available.
However, in person exams are still necessary in which of the following scenarios?
Answer Choices:
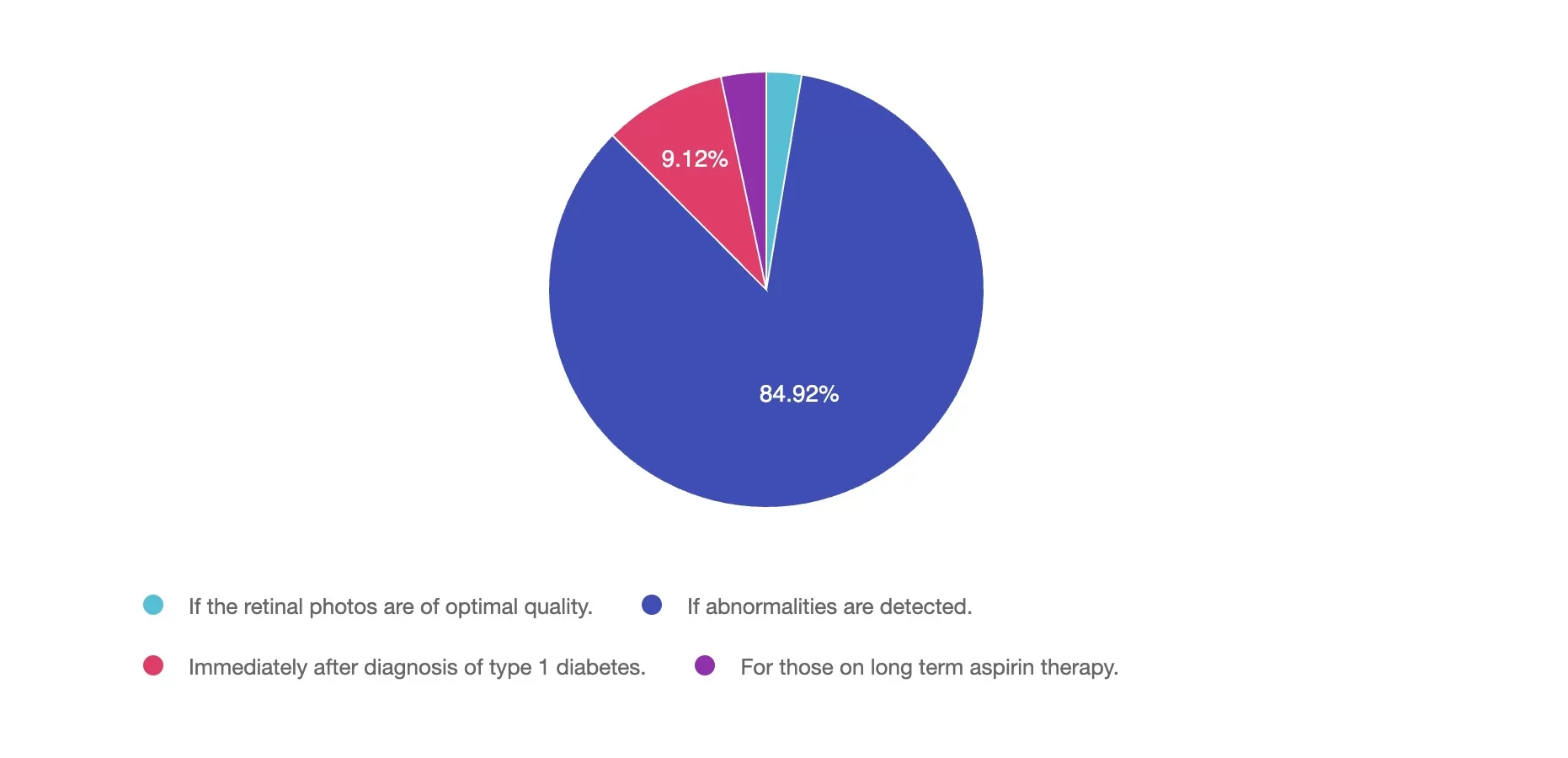
Answer 1 is incorrect. 2% chose this answer, “If the retinal photos are of optimal quality.” If retinal photos of are of high quality and there are no detected abnormalities, the retinal photo is sufficient.
Answer 2 is correct. 84% of you chose this answer, “If abnormalities are detected.” YES, GREAT JOB. If the retinal photos detect any abnormalities, an in-person comprehensive eye exam is necessary.
Answer 3 is incorrect. About 9% of respondents chose this, “Immediately after diagnosis of type 1 diabetes.” People diagnosed with type 1 diabetes are not required to get an immediate eye exam. The ADA Standards state that people with new type 1 diabetes need an eye exam within 5 years.
Finally, Answer 4 is incorrect. 3% chose this answer, “For those on long term aspirin therapy.” Since aspirin therapy does not elevate the risk of eye disease, individuals taking aspirin can safely participate in remote eye exams without concern.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!

Gain fresh insights, practical tools, and a deeper understanding of the latest in person-centered diabetes care. Our expert team brings the ADA Standards of Care to life—covering medications, behavior change, technology, and more! If you’re preparing for the CDCES or BC-ADM exam, this conference—paired with free bonus courses—serves as the ideal study companion!
With interactive co-teaching, we keep sessions engaging, relevant, and fun. Let’s learn and grow together!

Our expert team transforms complex diabetes science into clear, practical insights—keeping it real, engaging, and fun! The faculty includes:
The use of DES products does not guarantee the successful passage of the certification exam. CBDCE and ADCES do not endorse any preparatory or review materials for the CDCES or BC-ADM exams, except for those published by CBDCE & ADCES.
By: Beverly Thomassian

In the ever-evolving world of diabetes care, medications come in and out of favor based on new research, shifting safety data, and individual needs. Pioglitazone (Actos), once a go-to medication for improving insulin sensitivity, fell out of favor in the early 2010s due to concerns about bladder potential side effects and newer medications.
Now, pioglitazone is gaining renewed interest, especially for individuals with increased cardiovascular risk and steatosis, who may benefit from its unique profile. Even though pioglitazone only lowers A1C by 0.5 – 1.0%, this medication’s properties compel us to consider reintroducing it into the medical management of diabetes, especially in the presence of liver and heart disease. Plus, as a generic medication, its price tag of less than $5.00 a month makes it affordable for most people.
Pioglitazone is one of the thiazolidinedione (TZD) class of medications that work by enhancing insulin sensitivity, primarily through activation of PPAR-γ receptors in adipose and muscle tissue.
In a recent podcast, Banting Award Recipient, Dr. Ralph DeFronzo, provides an Insulin Resistance Master Class. He notes that pioglitazone, an insulin-sensitizing medication, improves cardiometabolic health, in part, by shifting fat distribution from visceral to subcutaneous areas. This redistribution of fat, may be associated with some weight gain. But, Dr. DeFronzo explains that this weight gain is actually a sign that the pioglitazone is working to improve insulin sensitivity. Compared to other oral agents, pioglitazone remains one of the most effective insulin sensitizers, especially useful in those with significant insulin resistance.
1. Cardiovascular Benefits – Decrease stroke and MI
The IRIS trial demonstrated that pioglitazone reduced the risk of stroke and myocardial infarction in insulin-resistant patients with a history of cerebrovascular events (Kernan et al., 2016). This benefit is being re-evaluated in the context of cardiometabolic risk, especially in people with atherosclerotic disease or metabolic syndrome.
The ADA Standard #3 states, “In people with a history of stroke and evidence of insulin resistance and prediabetes, pioglitazone may be considered to lower the risk of stroke or myocardial infarction. However, this benefit needs to be balanced with the increased risk of weight gain, edema, and fractures. Lower doses may mitigate the risk of adverse effects but may be less effective.”
2. Role in MASLD and MASH
Pioglitazone has shown promise in improving liver histology in people with metabolic-associated steatohepatitis (MASH), making it one of the few medications with such benefits (Cusi et al., 2017). Studies demonstrate it improves hepatic insulin sensitivity, reduces liver fat, and may slow fibrosis progression.
The ADA Standards of Care #4, include recommendations to start pioglitazone and GLP-1’s for individuals with diabetes and steatosis to prevent progression and slow fibrosis. “In phase 2 clinical trials, pioglitazone and some GLP-1 RAs have been shown to be potentially effective to treat steatohepatitis and to slow fibrosis progression. They may also decrease CVD, which is the number one cause of death in people with type 2 diabetes and MASLD.
3. Re-Evaluating Safety Concerns
Initial concerns about the risk of bladder cancer stemmed from observational studies; however, more recent analyses suggest that the risk is low or not statistically significant (Lewis et al., 2015). Furthermore, thoughtful prescribing—avoiding use in individuals with heart failure or active bladder cancer risk—helps mitigate potential harm. In addition, this medication is not recommended for those at risk of falls and fractures.
Comparative Benefits of Diabetes Medications
Here is a visual summary comparing the relative effects of pioglitazone versus other common medications:
Clinical Considerations
When considering pioglitazone (Actos), carefully assess:
Pioglitazone may also be especially helpful in combination with agents like metformin or GLP-1 receptor agonists, balancing out each other’s side effects and mechanisms of action.
Conclusion
Pioglitazone (Actos) may never regain its former status as a front-line diabetes treatment, but it has a clear and valuable role in today’s therapeutic landscape. For select individuals—especially those with insulin resistance, cardiovascular risk, or liver disease—pioglitazone offers an underutilized tool backed by strong evidence and decades of experience.
In diabetes care, what’s old can be new again—especially when paired with clinical wisdom and person-centered decision-making.
📚 References

This course provides the need-to-know information regarding the microvascular complications of diabetes. It includes a brief overview of pathophysiology & clinical manifestations along with prevention strategies & screening guidelines. This straightforward program will provide participants with the information they can use in a clinical setting & also provides critical content for certification exams.

A 62-year-old with type 1 diabetes presents for their follow-up visit. They report struggling with fatigue, poor sleep quality, and difficulty with glucose management despite taking medications as prescribed. Upon review, you find their A1C is 7.6%, and their average nightly sleep duration is 4.5-6 hours per night.
Based on the 2025 ADA Standards of Care, which of the following interventions would be the most appropriate next step to address sleep and glucose management?

Gain fresh insights, practical tools, and a deeper understanding of the latest in person-centered diabetes care. Our expert team brings the ADA Standards of Care to life—covering medications, behavior change, technology, and more! If you’re preparing for the CDCES or BC-ADM exam, this conference—paired with free bonus courses—serves as the ideal study companion!
With interactive co-teaching, we keep sessions engaging, relevant, and fun. Let’s learn and grow together!

Our expert team transforms complex diabetes science into clear, practical insights—keeping it real, engaging, and fun! The faculty includes:
For last week’s practice question, we quizzed participants on Who Benefits Most from Mindful Eating as a Primary Strategy? 67% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it below: Answer Question

Question: Mindful eating can support diabetes management in various ways.
For which of the following individuals would mindful eating be most effective as a primary strategy rather than a complementary approach?
Answer Choices:
If you are thinking about taking the certification exam, this practice test question will set you up for success. Test writers anticipate possible answers based on the details in the question. They will wave those “juicy answers” right under your nose. Your job is to weed through the particulars, pluck out the most important elements and choose the BEST answer.
Mindful eating is a flexible, non-restrictive approach that promotes awareness, self-regulation, and a healthier relationship with food. While many people with diabetes can benefit from mindful eating, individuals with a history of disordered eating often find it to be the most transformative strategy (Kristeller & Hallett, 1999; Miller et al., 2012; Mercado et al., 2021).
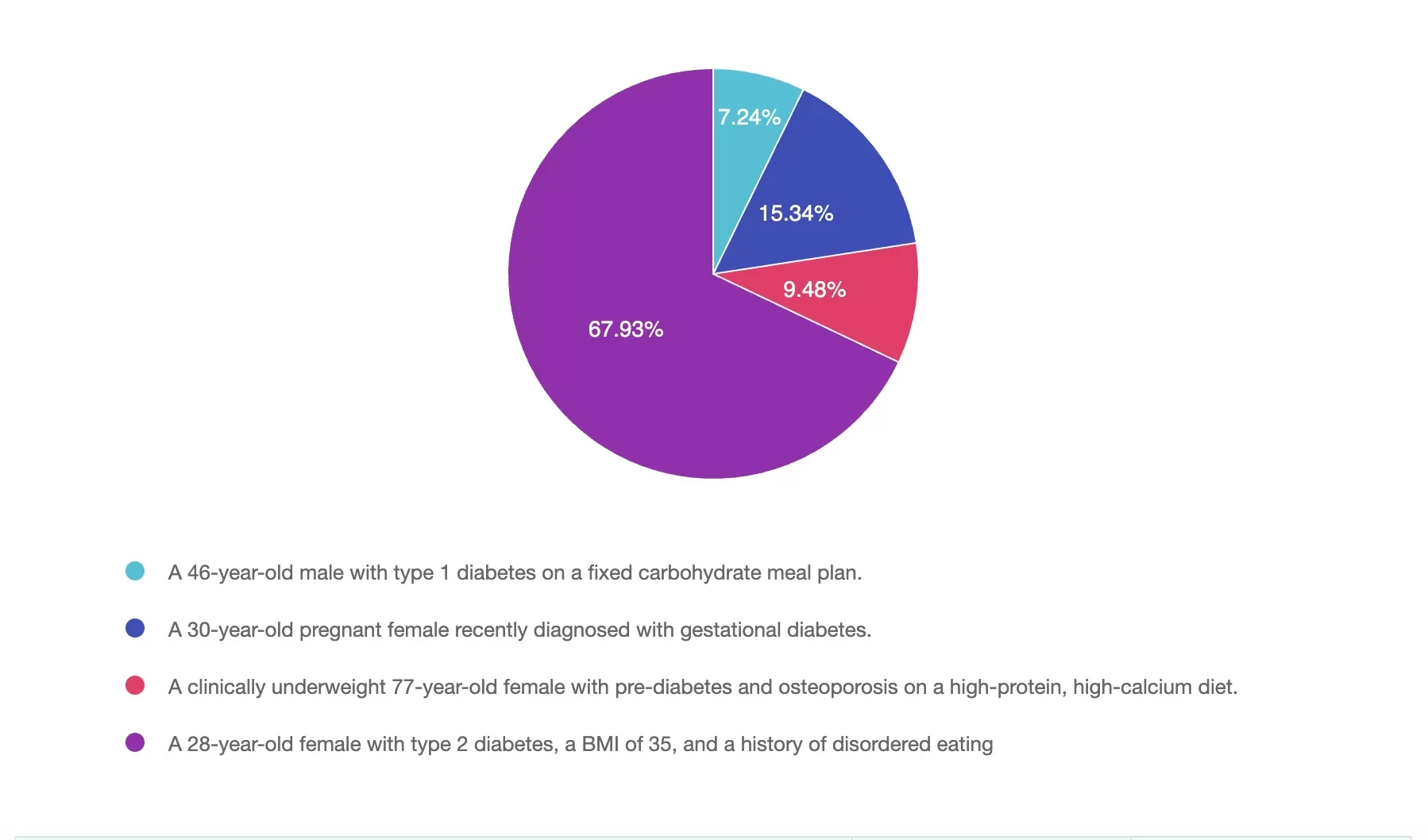
Answer 1 is incorrect. 7% chose this answer, “A 46-year-old male with type 1 diabetes on a fixed carbohydrate meal plan:
Answer 2 is incorrect. 15% of you chose this answer, “30-year-old pregnant female recently diagnosed with gestational diabetes:
Answer 3 is incorrect. About 9% of respondents chose this, “A clinically underweight 77-year-old female with prediabetes and osteoporosis on a high-protein, high-calcium diet:
Finally, Answer 4 is correct. 67% chose this answer, “A 28-year-old female with type 2 diabetes, BMI 35, and a history of disordered eating:
Mindful eating is most beneficial as a primary approach for individuals who have struggled with disordered eating patterns. Unlike restrictive diets, it provides a structured yet flexible way to reconnect with hunger cues, reduce emotional eating, and develop sustainable habits.
We hope this week’s rationale clarifies the diverse applications of mindful eating. Thank you for engaging with this question, and we look forward to more learning opportunities together!
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!
by Evgenia Evans, MS, RDN, CDCES
Aikens, J. E. (2012). Prospective associations between emotional distress and poor outcomes in type 2 diabetes. Diabetes Care, 35(12), 2472–2478. https://doi.org/10.2337/dc12-0181
Forman, E. M., Shaw, J. A., Goldstein, S. P., Butryn, M. L., Martin, L. M., Meiran, N., Crosby, R. D., & Manasse, S. M. (2016). Mindful decision making and inhibitory control training as complementary means to decrease snack consumption. Appetite, 103, 176-183. https://doi.org/10.1016/j.appet.2016.04.014
Framson, C., Kristal, A. R., Schenk, J. M., Littman, A. J., Zeliadt, S., & Benitez, D. (2009). Development and validation of the Mindful Eating Questionnaire. Journal of the American Dietetic Association, 109(8), 1439–1444. https://doi.org/10.1016/j.jada.2009.05.006
Fredrickson, B. L. (2004). The broaden-and-build theory of positive emotions. Philosophical Transactions of the Royal Society of London. Series B, Biological Sciences, 359(1449), 1367–1377. https://doi.org/10.1098/rstb.2004.1512
Garland, E. L., Fredrickson, B. L., Kring, A. M., Johnson, D. P., Meyer, P. S., & Penn, D. L. (2010). Upward spirals of positive emotions counter downward spirals of negativity: Insights from the broaden-and-build theory and affective neuroscience on the treatment of emotion dysfunctions and deficits in psychopathology. Clinical Psychology Review, 30(7), 849–864. https://doi.org/10.1016/j.cpr.2010.03.002
Harvard T.H. Chan School of Public Health. (2024, November 7). Mindful Eating. The Nutrition Source. https://nutritionsource.hsph.harvard.edu/mindful-eating/
Kabat-Zinn, J. (2009). Full catastrophe living: Using the wisdom of your body and mind to face stress, pain, and illness. Random House Publishing Group.
Kristeller, J. L., & Hallett, C. B. (1999). An exploratory study of a meditation-based intervention for binge eating disorder. Journal of Health Psychology, 4(3), 357–363. https://doi.org/10.1177/135910539900400305
Kristeller, J. L., Wolever, R. Q., & Sheets, V. (2014). Mindfulness-based eating awareness training (MB-EAT) for binge eating: A randomized clinical trial. Mindfulness, 5(3), 282–297. https://doi.org/10.1007/s12671-012-0179-1
Mercado, C., Marasigan, K., Cardona, J., & Ko, E. (2021). Mindfulness-based interventions for emotional eating and binge eating in adults: A meta-analysis. Appetite, 164, 105265. https://pmc.ncbi.nlm.nih.gov/articles/PMC11893636/
Miller, C. K. (2017). Mindful eating with diabetes. Diabetes Spectrum, 30(2), 89–94. https://doi.org/10.2337/ds16-0040
Miller, C. K., Kristeller, J. L., Headings, A., Nagaraja, H., & Miser, W. F. (2012). Comparative effectiveness of a mindful eating intervention to a diabetes self-management intervention among adults with type 2 diabetes: A pilot study. Journal of the Academy of Nutrition and Dietetics, 112(11), 1835–1842. https://doi.org/10.1016/j.jand.2012.07.036
Miller, C. K., Kristeller, J. L., Headings, A., & Nagaraja, H. (2014). Comparative effectiveness of a mindful eating intervention to a diabetes self-management intervention among adults with type 2 diabetes: A randomized controlled trial. Health Education & Behavior, 41(2), 145–154. https://doi.org/10.1177/1090198113493092
Nicolucci, A., Kovacs Burns, K., Holt, R. I. G., Comaschi, M., Hermanns, N., Ishii, H., Kokoszka, A., Pouwer, F., Skovlund, S. E., Stuckey, H., Tarkun, I., Vallis, M., Wens, J., & Peyrot, M. (2013). Diabetes Attitudes, Wishes and Needs second study (DAWN2™): Cross-national benchmarking of diabetes-related psychosocial outcomes for people with diabetes. Diabetic Medicine, 30(7), 767–777. https://doi.org/10.1111/dme.12245
Nelson, J. B. (2017). Mindful eating: The art of presence while you eat. Diabetes Spectrum, 30(3), 171–174. https://doi.org/10.2337/ds17-0015
Enroll in our upcoming webinar led by Evgeniya Evans, MS, RDN, CDCES
This engaging and practical webinar, developed by Evgeniya Evans, MS, RDN, CDCES, a positive psychology practitioner, is tailored explicitly for healthcare professionals including dietitians, diabetes care specialists, and providers.
Using evidence-based strategies, participants will gain a deeper understanding of the benefits of incorporating mindfulness into the eating experience, including enhanced glycemic management, improved emotional well-being, and healthier eating behaviors. The webinar includes an overview of mindfulness and mindful eating strategies, such as engaging all five senses, recognizing hunger cues, addressing cravings, and using practical tools to create supportive eating environments.

Participants will also learn how to adapt these approaches to diverse populations and the unique needs of individuals. Join us to deepen your expertise, participate in insightful discussions, and empower individuals to cultivate sustainable, positive relationships with food while achieving long-term health goals.
Course topics:

Evgeniya Evans, MAPP, RDN, LDN, CDCES, specializes in chronic disease prevention, diabetes management, and women’s health. Her unique approach integrates mindfulness-based nutrition and positive psychology, creating transformative impacts on her patients’ health and well-being.
Evgeniya’s academic journey reflects her dedication to lifelong learning and her holistic understanding of nutrition and health. She began with four years of Sociology studies at Omsk State University in Russia, followed by earning a Bachelor of Science in Nutrition and Dietetics from the University of Illinois Chicago. She furthered her expertise with a master’s degree in Applied Positive Psychology from the University of Pennsylvania. This diverse educational foundation allows her to address the socio-psychological factors that influence dietary behaviors and deliver a well-rounded approach to patient care.
At Cook County Health’s Diabetes Clinic within the Endocrinology Department, Evgeniya provides medically tailored nutrition therapy and culturally sensitive counseling. She works with individuals from various socio-economic backgrounds, guiding them through their unique health challenges with compassion and precision. Her dedication to creating personalized, sustainable dietary strategies highlights her commitment to promoting long-term health and vitality for her patients.
In addition to her clinical practice, Evgeniya is a passionate educator. She teaches several classes at her clinic, including Pillars of Diabetes Management with Lifestyle, Nutrition for Health and Vitality, and The Art of Mindful Eating. Her emphasis on education underscores her belief in the transformative power of fostering a healthy, enjoyable lifestyle supported by mindful eating and a positive mindset.
Evgeniya envisions a world where individuals are free from the struggles of dieting and food-related shame. She dreams of a future where no one feels deprecated by their appearance or food choices, and everyone enjoys the vitality and health to pursue their dreams. She is devoted to fostering vibrant, authentic lives where cooking, eating, and sharing meals with loved ones are sources of joy, love, and positive connection.
All hours earned count toward your CDCES Accreditation Information
The use of DES products does not guarantee the successful passage of the certification exam. CBDCE and ADCES do not endorse any preparatory or review materials for the CDCES or BC-ADM exams, except for those published by CBDCE & ADCES.