
Subscribe
eNewsletter

Ready to get certified?
Free CDCES Coach App
Download
Free Med Pocket Cards

eNewsletter

Free CDCES Coach App
Free Med Pocket Cards
Question of the Week:
A 62-year-old person with type 2 diabetes has an A1C of 9.1% despite metformin, SGLT-2i and a GLP-1 receptor agonist. You are considering once-weekly insulin icodec when it becomes available. Which of the following is the most appropriate rationale for selecting insulin icodec (Awiqli) therapy?

What is the BEST response?
A. Eliminates the risk of hypoglycemia compared to daily basal insulin.
B. Provides superior A1C reduction compared to all daily basal insulins.
C. Does not require dose titration due to its long duration of action.
D. Reduces injection frequency while improving time-in-range.


Walk away with tools you can apply immediately in clinical practice or while preparing for CDCES or BC-ADM exams. From insulin dosing protocols to behavior change strategies that work in the real world—this content bridges theory and practice.
Get exam-ready with confidence.
Course credits through AMA PRA Category 1 Credits™, ACPE, ANCC, and CDR!
Full accreditation details are available on the registration page

Our CDCES Boot Camp Online Prep Bundle is a comprehensive, high-impact program built specifically for healthcare professionals preparing for the Certified Diabetes Care and Education Specialist (CDCES) exam who want to level up their clinical knowledge and skills.

This evidence-based study bundle is a comprehensive BC-ADM Boot Camp designed for advanced-level healthcare professionals preparing for the Board Certified in Advanced Diabetes Management (BC-ADM) exam and will also provide you with state-of-the-art information to level up your clinical practice.

Recognizing the importance of comprehensive cardiovascular risk assessment, this article narrows in to review the newly recognized lipid screening strategies within the 2026 Dyslipidemia Guidelines from the American College of Cardiology/American Heart Association Joint Committee.¹
For diabetes care professionals, these updates are especially relevant, as cardiovascular disease remains the leading cause of mortality in individuals with both type 1 and type 2 diabetes.
Current ADA Standards of Care recommend statin therapy for most adults aged 40–75 with diabetes, with treatment intensity guided by overall cardiovascular risk.
While a standard lipid profile remains the foundational marker in estimation of ASCVD risk (PREVENT-ASCVD equations), the 2026 Dyslipidemia guidelines² highlight that additional lipid measures that may provide a more complete assessment of individual atherogenic risk.
Specifically,
In the following sections, we will review what each of these lipid components represents and how they contribute to a more comprehensive understanding of cardiovascular risk.
Non-HDL is part of a standard lipid profile.
It represents all atherogenic, plaque-forming particles in the blood and correlates with ApoB.¹ It is easily calculated by subtracting high-density lipoprotein (HDL) from total cholesterol.
Non-HDL may add risk prediction beyond LDL, especially if triglycerides exceed 150 mg/dL, and is reported to be a better predictor of ASCVD risk than LDL.
Non-HDL Targets:
This threshold also applies to individuals with diabetes who have ASCVD or diabetes-specific risk factors.1 In those with subclinical or clinical atherosclerosis, an optional, even more intensive Non-HDL goal of <85 mg/dL is advised.¹
While LDL estimates the amount of cholesterol carried within LDL particles, apoB reflects the total number of atherogenic lipoproteins and provides a more direct measure of the number of atherogenic particles in circulation.
Each atherogenic particle, including LDL, very-low-density lipoprotein (VLDL), intermediate-density lipoprotein, and Lp(a), contains a single apoB molecule,1 meaning apoB serves as a one-to-one marker of total particle number.4
In contrast, LDL particles vary in size and composition. Larger LDL particles tend to carry more cholesterol, while smaller, denser LDL particles carry less cholesterol per particle but are considered more atherogenic. These small, dense LDL particles easily penetrate the arterial wall, are more susceptible to oxidation, and have a longer circulating half-life, all of which increase their potential to promote atherosclerosis.5
An individual may have an LDL value at goal yet still have a high number of small, dense LDL particles and higher cardiovascular risk. This discordance is more common in individuals with ASCVD, cardiometabolic kidney syndrome, elevated triglycerides (>150 mg/dL), or diabetes.
In these cases, apoB can provide better insight into individual risk and therapeutic guidance. A higher particle number is strongly associated with an increased risk of myocardial infarction and other ASCVD events.
ApoB goals for individuals with diabetes are stratified as follows:

The Dyslipidemia guidelines recommend that Lp(a) should be measured at least once in all adults to identify inherited cardiovascular risk.³
As diabetes care providers committed to person-centered care, the 2026 Dyslipidemia Guidelines emphasize additional assessment strategies (see footnote) to better individualize cardiovascular risk.
While achieving LDL targets remains an important therapeutic goal; incorporating non–HDL-C, apoB, and Lp(a) into lipid monitoring may help identify residual risk, particularly in individuals with diabetes, elevated triglycerides, or other cardiometabolic conditions.
With the ADA endorsing these guidelines, we are encouraged to consider when expanded lipid testing is appropriate, advocate for comprehensive risk assessment, and use these insights to guide shared decision-making for therapeutic interventions.
Christine Craig, MS, RDN, CDCES
Founder: Nutrition for Daily Living
2026 Dyslipidemia Guidelines recommends use of CPR. Calculating 10 year risk using the PREVENT equation (https://professional.heart.org/en/guidelines-and-statements/prevent-calculator), Personalizing the estimated risk for the individual and Reclassifying and Reassessing treatment recommendations with additional tools such as the Coronary artery calcium.

Use Code “Nurse20” during checkout to apply the discount
Sale ends May 12th at 11:59 PM PST
All healthcare professionals are welcome to save!
Get exam-ready with confidence.
Course credits through AMA PRA Category 1 Credits™, ACPE, ANCC, and CDR!
Full accreditation details are available on the registration page

Our CDCES Boot Camp Online Prep Bundle is a comprehensive, high-impact program built specifically for healthcare professionals preparing for the Certified Diabetes Care and Education Specialist (CDCES) exam who want to level up their clinical knowledge and skills.

This evidence-based study bundle is a comprehensive BC-ADM Boot Camp designed for advanced-level healthcare professionals preparing for the Board Certified in Advanced Diabetes Management (BC-ADM) exam and will also provide you with state-of-the-art information to level up your clinical practice.

Join national experts including Dr. Diana Isaacs (Cleveland Clinic), Beverly Thomassian (30+ years of experience), and Christine Craig for high-impact, virtual learning—no travel required.
✔ Learn from National Experts — Anywhere
Get the same expert-level instruction you’d receive in person, delivered live to your home or office.
✔ 1-year Access

There is a lot of exciting news contained in this month’s newsletter. The world of diabetes pharmacology is advancing at a breakneck pace, and we are here to keep you abreast of advances that will impact your clinical practice and your care for people with diabetes.
The first article describes the pharmacology and dosing considerations for icodec (Awiqli), an ultra-long-acting insulin scheduled for release in the second quarter of 2026. As we wait for its release, you can consider people with type 2 diabetes in your care who might benefit from this once-weekly basal insulin.
There has been significant movement in the GLP-1/GIP med class, from high-dose Wegovy to Mounjaro’s pediatric approval, highlighted in our next article. You are going to love our updated PocketCards, which neatly consolidate this shifting landscape at a glance for easy reference. Continued below…
In a thoughtful comparison of the ADA and the American College of Cardiology dyslipidemia treatment guidelines, Christine Craig, MS, RDN, CDCES, concludes that both recognize the critical impact of dietitians and MNT in addressing elevated lipid levels.
Sarah Beattie, DNP, CDCES, highlights the importance of eye exams and encourages the use of remote retinal screening for those without access to an eye care professional in their area.
Test your knowledge with a quiz that investigates potential candidates for once-weekly insulin and check out our rationale of the week too.
Lastly, we hope to see you at our Virtual Conference. Diana Issaacs, PharmD, CDCES, BC-ADM, will dive into the newly approved diabetes meds and insulins, helping you sort out how to best use these tools in clinical practice.
In celebration of Spring,
Coach Beverly, Bryanna, and Katarina

Join national experts including Dr. Diana Isaacs (Cleveland Clinic), Beverly Thomassian (30+ years of experience), and Christine Craig for high-impact, virtual learning—no travel required.
✔ Learn from National Experts — Anywhere
Get the same expert-level instruction you’d receive in person, delivered live to your home or office.
✔ Interactive & Flexible

Walk away with tools you can apply immediately in clinical practice or while preparing for CDCES or BC-ADM exams. From insulin dosing protocols to behavior change strategies that work in the real world—this content bridges theory and practice.
Get exam-ready with confidence.
Course credits through AMA PRA Category 1 Credits™, ACPE, ANCC, and CDR!
Full accreditation details are available on the registration page

Our CDCES Boot Camp Online Prep Bundle is a comprehensive, high-impact program built specifically for healthcare professionals preparing for the Certified Diabetes Care and Education Specialist (CDCES) exam who want to level up their clinical knowledge and skills.

This evidence-based study bundle is a comprehensive BC-ADM Boot Camp designed for advanced-level healthcare professionals preparing for the Board Certified in Advanced Diabetes Management (BC-ADM) exam and will also provide you with state-of-the-art information to level up your clinical practice.
For last week’s practice question, we quizzed participants on checkpoint inhibitors triggering hyperglycemia. 34% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it by clicking here.

Betty, a 60-year-old female, is receiving pembrolizumab, an immune checkpoint inhibitor, as treatment for melanoma. She is worried about the potential adverse effects. She is very concerned about the risk of developing diabetes. Her recent lab work shows normal fasting blood glucose and hemoglobin A1c.
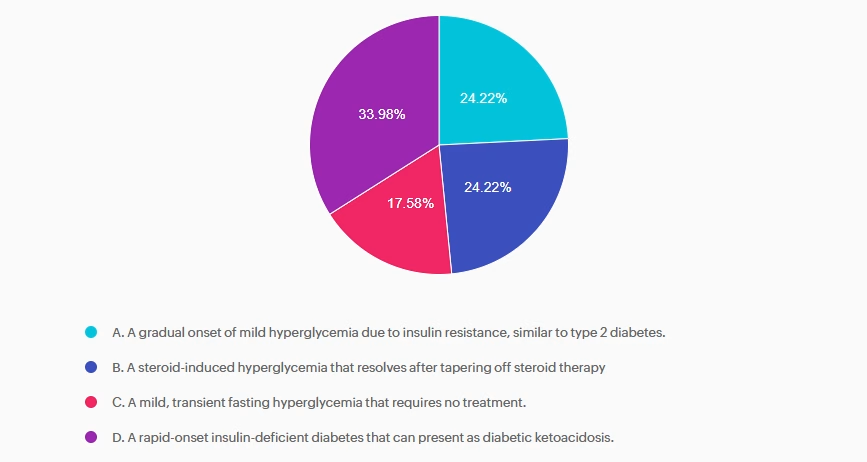
Answer 1 is incorrect. 24.22% chose this answer, “A gradual onset of mild hyperglycemia due to insulin resistance, similar to type 2 diabetes.” This answer is incorrect. Immune checkpoint inhibitor medications do not cause mild hyperglycemia but instead cause significant hyperglycemia and DKA similar to type 1 diabetes.
Answer 2 is incorrect. 24.22% of you chose this answer, “A steroid-induced hyperglycemia that resolves after tapering off steroid therapy.” This answer is incorrect. Though steroid treatment is often needed, hyperglycemia in immune checkpoint inhibitor-associated diabetes is not resolved after tapering off steroids.
Answer 3 is incorrect. About 17.58% of respondents chose this: “A mild, transient fasting hyperglycemia that requires no treatment.” This answer is incorrect. Though steroid treatment is often needed, hyperglycemia in immune checkpoint inhibitor-associated diabetes is not resolved after tapering off steroids.
Finally, Answer 4 is correct. 33.98% chose this answer, “A rapid-onset insulin-deficient diabetes that can present as diabetic ketoacidosis.” This answer is correct. Due to immune checkpoint inhibitor-induced immune system alterations, hyperglycemia and insulin deficiency can rapidly develop, often leading to DKA.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!

Join national experts including Dr. Diana Isaacs (Cleveland Clinic), Beverly Thomassian (30+ years of experience), and Christine Craig for high-impact, virtual learning—no travel required.
✔ Learn from National Experts — Anywhere
Get the same expert-level instruction you’d receive in person, delivered live to your home or office.
✔ Interactive & Flexible

Walk away with tools you can apply immediately in clinical practice or while preparing for CDCES or BC-ADM exams. From insulin dosing protocols to behavior change strategies that work in the real world—this content bridges theory and practice.
Get exam-ready with confidence.
Course credits through AMA PRA Category 1 Credits™, ACPE, ANCC, and CDR!
Full accreditation details are available on the registration page

Our CDCES Boot Camp Online Prep Bundle is a comprehensive, high-impact program built specifically for healthcare professionals preparing for the Certified Diabetes Care and Education Specialist (CDCES) exam who want to level up their clinical knowledge and skills.

This evidence-based study bundle is a comprehensive BC-ADM Boot Camp designed for advanced-level healthcare professionals preparing for the Board Certified in Advanced Diabetes Management (BC-ADM) exam and will also provide you with state-of-the-art information to level up your clinical practice.


Question of the Week:
KC is a 62-year-old individual with type 2 diabetes who presents for follow-up after initiating a weight loss program 3 months ago. They report consuming approximately 1,000–1,100 kcal/day and have lost 12% of their body weight, with a current rate of weight loss averaging 5% in the last month.
Their diet excludes most grains and fruits, and they report occasional fatigue and constipation. Current medications include metformin, tirzepatide, and atorvastatin.
Based on current standards of care, what is the most appropriate response regarding nutrition and weight changes?

What is the BEST response?
Get exam-ready with confidence.
Course credits through AMA PRA Category 1 Credits™, ACPE, ANCC, and CDR!
Full accreditation details are available on the registration page

Our CDCES Boot Camp Online Prep Bundle is a comprehensive, high-impact program built specifically for healthcare professionals preparing for the Certified Diabetes Care and Education Specialist (CDCES) exam who want to level up their clinical knowledge and skills.

This evidence-based study bundle is a comprehensive BC-ADM Boot Camp designed for advanced-level healthcare professionals preparing for the Board Certified in Advanced Diabetes Management (BC-ADM) exam and will also provide you with state-of-the-art information to level up your clinical practice.

Join national experts including Dr. Diana Isaacs (Cleveland Clinic), Beverly Thomassian (30+ years of experience), and Christine Craig for high-impact, virtual learning—no travel required.
✔ Learn from National Experts — Anywhere
Get the same expert-level instruction you’d receive in person, delivered live to your home or office.
✔ Interactive & Flexible

Walk away with tools you can apply immediately in clinical practice or while preparing for CDCES or BC-ADM exams. From insulin dosing protocols to behavior change strategies that work in the real world—this content bridges theory and practice.


In diabetes care, what is the reported percentage
of patients who have missed or not returned for follow-up care due to feelings of shame, blame, or judgment?

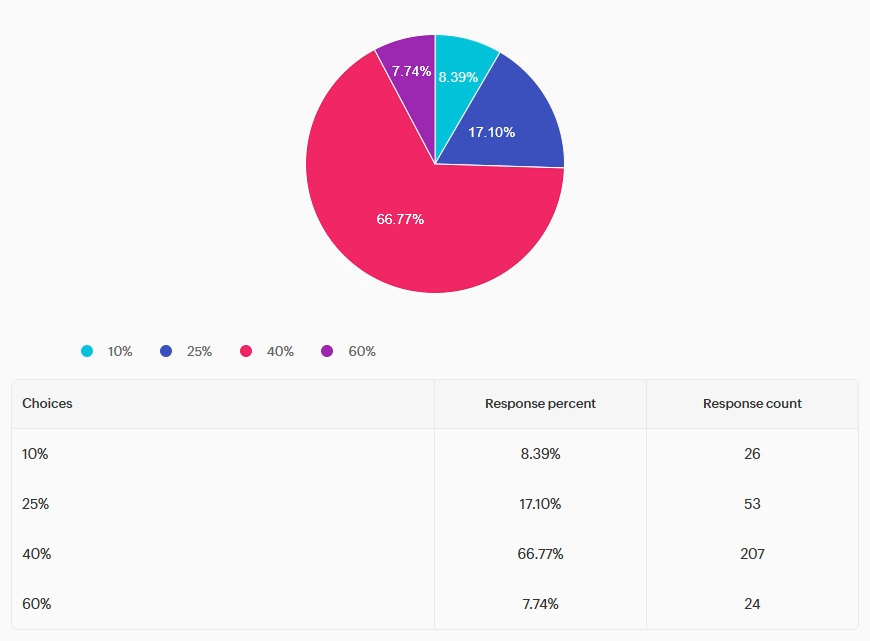
Answer A is incorrect: 8.39% chose this answer, “10%.” This answer underestimates the problem. Research indicates that approximately 40% of patients with diabetes may miss or avoid follow-up appointments because they experience feelings of shame, blame or judgment related to their condition or care. This highlights the importance of delivering diabetes care with stigma-free, supportive communication approaches as a means to improve engagement and outcomes
Answer B is incorrect: 17.10% chose this answer, “25%.” This answer underestimates the problem. Research indicates that approximately 40% of patients with diabetes may miss or avoid follow-up appointments because they experience feelings of shame, blame or judgment related to their condition or care. This highlights the importance of delivering diabetes care with stigma-free, supportive communication approaches as a means to improve engagement and outcomes.
Answer C is correct: 66.77% chose the correct answer, GREAT JOB. “40%.” Per the 2026 ADA Standards of Care, bone health needs to be assessed in men aged ≥50 years with type 2 diabetes and an A1c >8%. He is also on pioglitazone, a thiazolidinedione, which is another risk factor for low bone density.
Answer D is incorrect: 7.74% chose this answer, “60%.” This answer overestimates the problem. Research indicates that approximately 40% of patients with diabetes may miss or avoid follow-up appointments because they experience feelings of shame, blame or judgment related to their condition or care. This highlights the importance of delivering diabetes care with stigma-free, supportive communication approaches as a means to improve engagement and outcomes.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!

All hours earned count toward your CDCES Accreditation Information
The use of DES products does not guarantee the successful passage of the certification exam. CBDCE and ADCES do not endorse any preparatory or review materials for the CDCES or BC-ADM exams, except for those published by CBDCE & ADCES.

Did you know that in ancient times, diabetes was identified by the sweet taste of a person’s urine?
Thankfully, science has come a long way from this ancient practice! The introduction of fingerstick blood glucose meters in the 1970s and continuous glucose monitors (CGMs) in the early 2000’s marked significant advancements in blood glucose monitoring. With more than 800 million people worldwide living with diabetes, interest in pain-free glucose testing is growing.1
Although current CGMs and fingerstick methods still require skin penetration, needle-free alternatives are being promoted, prompting many questions. Let’s discuss how healthcare professionals can address these products using evidence-based information.
Noninvasive (NI) glucose monitoring is a method of measuring blood glucose that does not involve breaking the skin. NI glucose monitoring technology under development includes: 2
FDA approval is granted for glucose monitoring devices used for either medical or lifestyle management. FDA approval for medical management is based on sufficient evidence of safety and accuracy for people living with diabetes. FDA approval ensures adequate evidence to guide treatment decisions, such as insulin dosing. FDA approval for lifestyle use applies to individuals who do not use the device for the medical management of diabetes and who are not on insulin therapy.
Currently, no NI glucose monitoring devices have received FDA approval for medical management of diabetes. In 2024, the FDA issued a safety announcement that NI glucose devices could pose a possible threat to those with diabetes, as the FDA has not approved them.3 Numerous companies are currently in the research process to advance NI glucose monitoring devices toward FDA approval.
When considering noninvasive glucose monitoring, it’s essential to understand how these devices fit into everyday diabetes care. Despite the lack of FDA approval, clients can purchase NI glucose monitoring devices without a prescription. Clients may be using these before the healthcare provider is ever aware.
Individuals living with diabetes should be aware that many factors, including hydration status, skin characteristics, temperature, and movement, can affect NI glucose device readings. These devices may be better suited for detecting general trends but are not approved for making real-time treatment decisions. As diabetes healthcare professionals, we can provide guidance on the use of FDA-approved devices to verify readings and inform treatment decisions. Arming our clients with this information can help avoid frustration and unsafe treatment decisions.
Diabetes healthcare providers often approach noninvasive (NI) glucose monitoring with cautious optimism. While the appeal of “no more pokes” is understandable, clients may be influenced by strong marketing claims. As providers, our role is to meet clients where they are to start the conversation.
As with any other FDA-approved diabetes technology, not every device is the right fit for everyone. Ask clients about their diabetes goals, barriers, and assess their digital literacy. Address what clients are seeing on social media and online ads, and how these NI devices compare to current FDA-approved blood glucose monitoring technology.
Here are some helpful tips that can further the conversation:
As technology advances, we hope to see accurate and safe NI glucose monitoring options for those living with diabetes. Until then, we can partner with our clients to provide education and clinical insights on the latest trends in diabetes technology.
References:
Get exam-ready with confidence.
Course credits through AMA PRA Category 1 Credits™, ACPE, ANCC, and CDR!
Full accreditation details are available on the registration page

Our CDCES Boot Camp Online Prep Bundle is a comprehensive, high-impact program built specifically for healthcare professionals preparing for the Certified Diabetes Care and Education Specialist (CDCES) exam who want to level up their clinical knowledge and skills.

This evidence-based study bundle is a comprehensive BC-ADM Boot Camp designed for advanced-level healthcare professionals preparing for the Board Certified in Advanced Diabetes Management (BC-ADM) exam and will also provide you with state-of-the-art information to level up your clinical practice.

Join national experts including Dr. Diana Isaacs (Cleveland Clinic), Beverly Thomassian (30+ years of experience), and Christine Craig for high-impact, virtual learning—no travel required.
✔ Learn from National Experts — Anywhere
Get the same expert-level instruction you’d receive in person, delivered live to your home or office.
✔ Interactive & Flexible

Walk away with tools you can apply immediately in clinical practice or while preparing for CDCES or BC-ADM exams. From insulin dosing protocols to behavior change strategies that work in the real world—this content bridges theory and practice.



Betty, a 60-year-old female, is receiving pembrolizumab, an immune checkpoint inhibitor, as treatment for melanoma. She is worried about the potential adverse effects. She is very concerned about the risk of developing diabetes. Her recent lab work shows normal fasting blood glucose and hemoglobin A1c.
Get exam-ready with confidence.
Course credits through AMA PRA Category 1 Credits™, ACPE, ANCC, and CDR!
Full accreditation details are available on the registration page

Our CDCES Boot Camp Online Prep Bundle is a comprehensive, high-impact program built specifically for healthcare professionals preparing for the Certified Diabetes Care and Education Specialist (CDCES) exam who want to level up their clinical knowledge and skills.

This evidence-based study bundle is a comprehensive BC-ADM Boot Camp designed for advanced-level healthcare professionals preparing for the Board Certified in Advanced Diabetes Management (BC-ADM) exam and will also provide you with state-of-the-art information to level up your clinical practice.

Join national experts including Dr. Diana Isaacs (Cleveland Clinic), Beverly Thomassian (30+ years of experience), and Christine Craig for high-impact, virtual learning—no travel required.
✔ Learn from National Experts — Anywhere
Get the same expert-level instruction you’d receive in person, delivered live to your home or office.
✔ Interactive & Flexible

Walk away with tools you can apply immediately in clinical practice or while preparing for CDCES or BC-ADM exams. From insulin dosing protocols to behavior change strategies that work in the real world—this content bridges theory and practice.


