
Subscribe
eNewsletter

Ready to get certified?
Free CDCES Coach App
Download
Free Med Pocket Cards

eNewsletter

Free CDCES Coach App
Free Med Pocket Cards
For last week’s practice question, we quizzed participants on the new ADA Standards and the development of type 2 diabetes. 42.48% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it below: Answer Question

According to the new 2026 ADA Standards, “type 2 diabetes is associated with insulin secretory defects related to” which of the following?
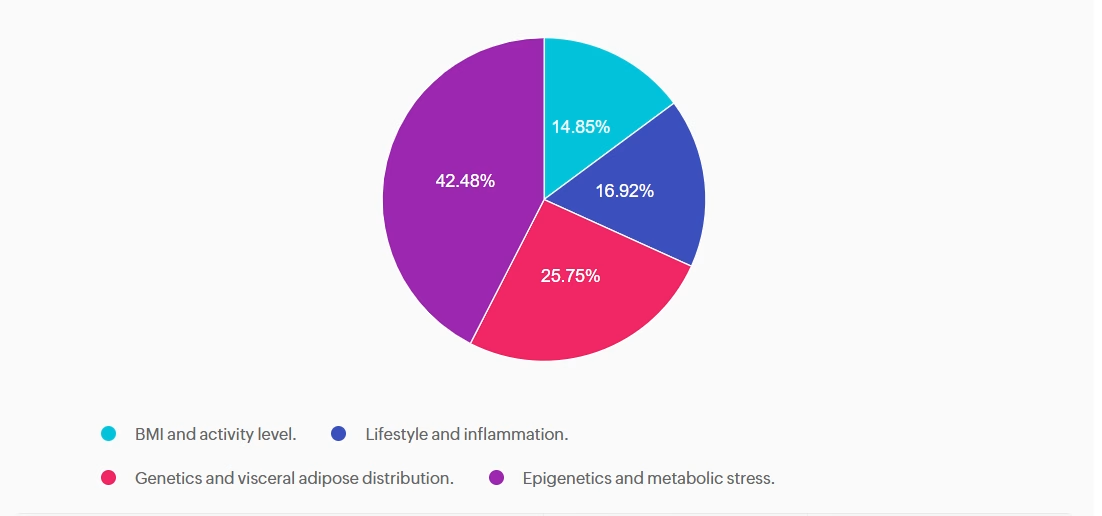
Answer A is incorrect: 14.85% chose this answer, “BMI and activity level.” This answer is incorrect but tempting. BMI level is used as a a screening tool for prediabetes and diabetes risk, but is not included as a factor contributing to secretory defects. According to the ADA, there are four factors related to insulin secretory defects in type 2 diabetes. They include; genetics, epigenetics, metabolic stress and inflammation.
Answer B is incorrect: 16.92% chose this answer, “Lifestyle and inflammation.” This juicy answer is incorrect. Lifestyle is not a direct factor related to insulin secretory defects, but inflammation is a contributor. According to the ADA, there are four factors related to insulin secretory defects in type 2 diabetes. They include; genetics, epigenetics, metabolic stress and inflammation.
Answer C is incorrect: 25.75% chose this answer, “Genetics and visceral adipose distribution.” This answer is incorrect. Visceral adiposity is associated with an increased risk for diabetes, but does not contribute to insulin secretory defects. According to the ADA, there are four factors related to insulin secretory defects in type 2 diabetes. They include; genetics, epigenetics, metabolic stress and inflammation.
Answer D is correct: 42.48% chose this answer, “Epigenetics and metabolic stress.” This answer is correct, GREAT JOB! According to the ADA, there are four factors related to insulin secretory defects in type 2 diabetes. They include; genetics, epigenetics, metabolic stress and inflammation.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!

For last week’s practice question, we quizzed participants on JR studying to take their CDCES exam, and they have questions studying for the 2025 or 2026 ADA Standards of Care. 55.56% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it below: Answer Question

JR has been diligently studying to take their CDCES exam at the end of January 2026. They are wondering if they should study the 2025 or 2026 ADA Standards of Care.
As a mentor to healthcare professionals entering the field of diabetes, what do you recommend?
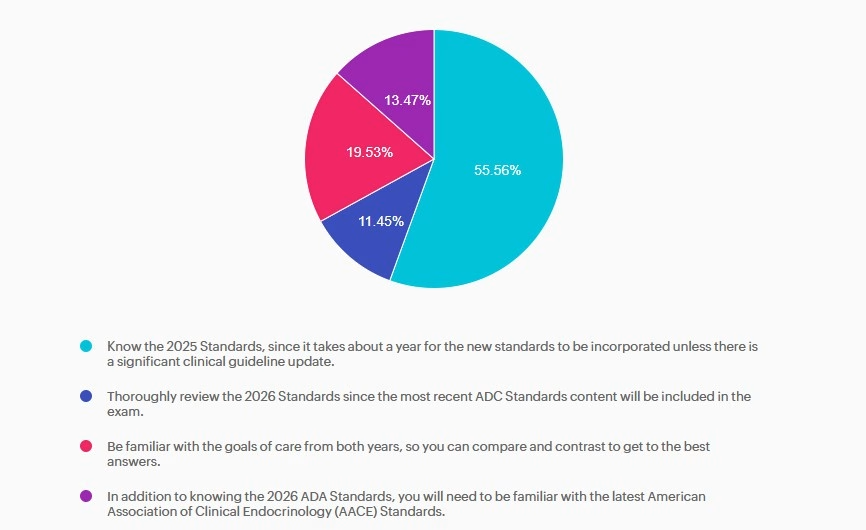
Answer A is correct: 55.56% chose this answer, “Know the 2025 Standards, since it takes about a year for the new standards to be incorporated unless there is a significant clinical guideline update.” Answer A is the BEST answer. It takes at least a year for the CBDCE to update the exam based on the ADA Standards. Knowing the 2025 Standards along with any urgent clinical updates announced in 2026 will help prepare JR for success.
Answer B is incorrect: 11.45% chose this answer, “Thoroughly review the 2026 Standards since the most recent ADC Standards content will be included in the exam.” Answer B is not the best answer. Since it takes at least a year for the CBDCE to update the exam based on the ADA Standards, JR can feel comfortable knowing the 2025 Standards along with any urgent clinical updates announced in 2026.
Answer C is incorrect: 19.53% chose this answer, “Be familiar with the goals of care from both years, so you can compare and contrast to get to the best answers.” Answer C is not the best answer. Thinking about comparing and contrasting two consecutive years standards and lead to testing confusion. JR can feel comfortable knowing the 2025 Standards along with any urgent clinical updates announced in 2026.
Answer D is incorrect: 13.47% chose this answer, “In addition to knowing the 2026 ADA Standards, you will need to be familiar with the latest American Association of Clinical Endocrinology (AACE) Standards.” Answer D is not the best answer. Since it takes at least a year for the CBDCE to update the exam based on the ADA Standards, JR can feel comfortable knowing the 2025 Standards along with any urgent clinical updates announced in 2026.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!
For last week’s practice question, we quizzed participants on SJ having questions about their insulin pen, and what would be the best response. 41.72% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it below: Answer Question

SJ is 52 years old with a 10-year history of type 2 diabetes. They recently started on insulin degludec U-100 Flex Touch pen 15 units per day. At a follow-up visit, SJ brings their insulin pen and mentions they have been keeping it in their work bag since starting therapy. They are unsure how long they can continue to use this same pen.
What is the best advice for SJ for insulin storage in this situation?
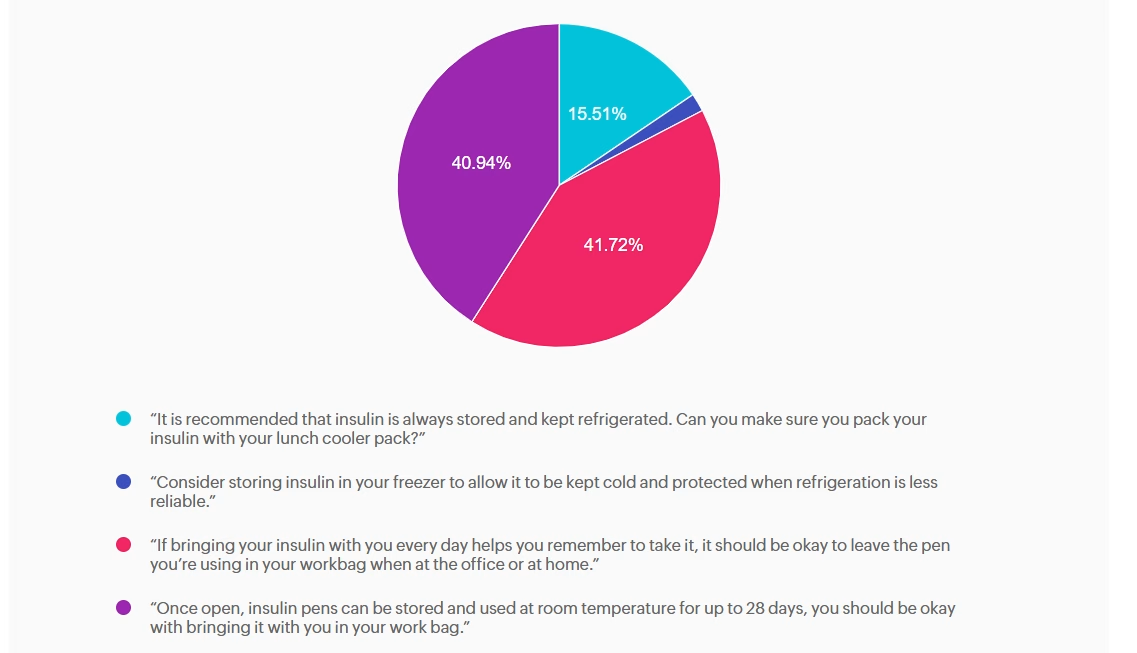
Answer A is incorrect: 15.51% chose this answer, “It is recommended that insulin is always stored and kept refrigerated. Can you make
sure you pack your insulin with your lunch cooler pack?” While refrigeration is ideal for insulin storage, insulin does not always need to be refrigerated. Once in use, most insulins, including degludec, are stable at room temperature (below 86F or 30 C). Advising refrigeration may create unnecessary barriers and does not reflect degludec’s stability profile.
Answer B is incorrect: 1.83% chose this answer, “Consider storing insulin in your freezer to allow it to be kept cold and protected when
refrigeration is less reliable.” Freezing damages insulin molecules, making the insulin ineffective and unsafe to use. This option contradicts manufacturer and clinical safety guidance.
Answer C is correct: 41.72% chose this answer, “If bringing your insulin with you every day helps you remember to take it, it should be
okay to leave the pen you’re using in your workbag when at the office or at home.” Insulin degludec is stable at room temperature below 86°F (30°C) for up to 56 days (8 weeks) once opened. If SJ’s work bag is not exposed to excessive heat or freezing, keeping the pen there is acceptable and may in fact support consistent dosing. We can also calculate SJ’s monthly insulin pen usage (15 units per day + 2 unit prime per injection = 510 units per month or 2 pens per month), knowing he will easily use more insulin than open insulin pen stability time window.
Answer D is incorrect: 40.94% chose this answer, “Once open, insulin pens can be stored and used at room temperature for up to 28 days, you should be okay with bringing it with you in your work bag.” While it is correct that insulin does not always require refrigeration once in use, the specific duration varies by insulin type; degludec lasts longer than 28 days.
To learn more, check out our Insulin Storage Cheat Sheet.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!

For last week’s practice question, we quizzed participants on RT forgetting their insulin, and what would be the best response. 62.93% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it below: Answer Question

JR was recently diagnosed with type 2 diabetes, but based on their history of pancreatitis, you suspect JR actually has Diabetes Type 3c.
Which of the following symptoms match a diagnosis of Diabetes Type 3c?
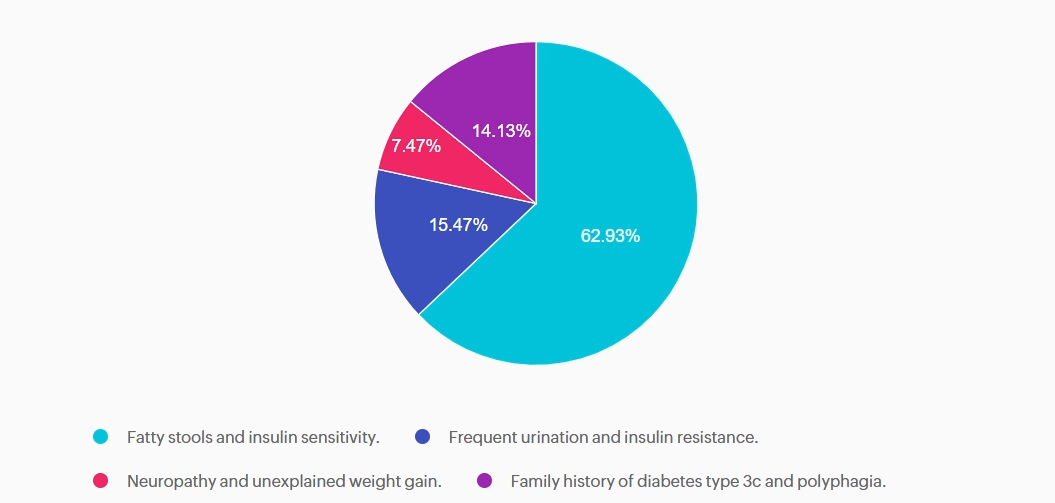
Answer A is correct: 62.93% chose this answer, “Fatty stools and insulin sensitivity.” Steatorrhea, or fatty stools, results from poor fat digestion due to insufficient pancreatic enzymes—a key feature of type 3c diabetes, with it’s hallmark exocrine enzyme insufficiency. People with diabetes type 3c, can also be very insulin sensitive, since they don’t have the insulin resistance associated with type 2 diabetes. In addition to diabetes medications, they may benefit from pancreatic enzyme replacement therapy (PERT) to improve absorption of fatty foods and decrease steatorrhea.
Answer B is incorrect: 15.47% chose this answer, “Frequent urination and insulin resistance.” Frequent urination and insulin resistance is associated with type 2 diabetes. With type 3c, since many of the beta cells are destroyed due to trauma not genetics, these individuals may have polyuria from hyperglycemia, but they are not usually insulin resistant, just deficient.
Answer C is incorrect: 7.47% chose this answer, “Neuropathy and unexplained weight gain.” They may get neuropathy if their blood glucose is elevated for a long period of time, but that is not part of the differential. People with type 3c usually experience weight loss due to the lack of pancreatic enzymes that help with nutrient absorption.
Answer D is incorrect: 14.13% chose this answer, “Family history of diabetes type 3c and polyphagia.” Type 3c diabetes is not passed on through genes, it is due to exocrine damage to the pancreas which can lead to destruction of beta cells. Most common causes of diabetes type 3c include pancreatitis, cystic fibrosis, pancreatic cancer, and hemochromatosis. Some people could experience extreme hunger if their glucose levels are elevated for an extended period of time.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!
For last week’s practice question, we quizzed participants on Gestational Diabetes: Diabetes Care in the Fourth Trimester. 51% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it below: Answer Question

MT is a 29-year-old with Type 1 diabetes who is currently 14 weeks pregnant. She uses a continuous glucose monitor (CGM) with concurrent fingersticks and uploads her glucose data weekly. Her CGM settings was already set to the recommended time in
range and the latest CGM report shows the following: time in range (TIR): 67%, time below range: 6%, time above range: 27%.
Based on current ADA Standard of Care, which of the following statements is most accurate regarding her CGM values?
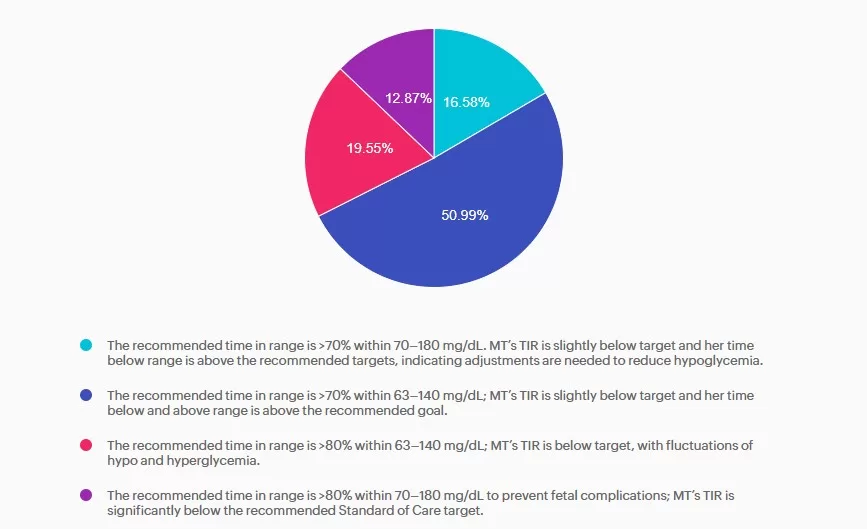
Answer A is incorrect: 16.58% chose this answer, “The recommended time in range is >70% within 70–180 mg/dL. MT’s TIR is slightly below target and her time below range is above the recommended targets, indicating adjustments are needed to reduce hypoglycemia.” Answer A is incorrect. The answer uses non-pregnancy CGM target range of 70–180 mg/dL. Pregnancy target range for individuals with type 1 diabetes are lower, keep reading for the best answer.
Answer B is correct: 51% chose this answer, “The recommended time in range is >70% within 63–140 mg/dL; MT’s TIR is slightly below target and her time below and above range is above the recommended goal.” Answer B is correct. Based on the 2025 ADA Standards of Care the recommended time in range targets for individuals with type 1 diabetes during pregnancy is >70% between 63-140 mg/dL, < 4% under 63 mg/dL with < 1 % under 54 mg/dL, and < 25% over 140 mg/dL.
Answer C is incorrect: 19.55% chose this answer, “The recommended time in range is >80% within 63–140 mg/dL; MT’s TIR is below target, with fluctuations of hypo and hyperglycemia.” Answer C is incorrect. The time in range target is above the evidenced-based
minimum and MT is having frequent hypoglycemia in addition to hyperglycemia, both outside the goal ranges.
Answer D is incorrect: 12.87% chose this answer, “The recommended time in range is >80% within 70–180 mg/dL to prevent fetal
complications; MT’s TIR is significantly below the recommended Standard of Care target.” Answer D is incorrect. The recommended target range for individuals with type 1diabetes during pregnancy is 63-140 mg/dL as stated above.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!
with Coach Beverly Thomassian RN, MPH, CDCES, BC-ADM
Course credits through AMA PRA Category 1 Credits™, ACPE, ANCC, and CDR!
This course is included in our Level 2 | Standards of Care Intensive
This Level 2 course fulfills the annual ADA Standards of Care component required for CDCES certification renewal. They also count toward your CDCES and BC-ADM certification CE requirements.

Join Coach Bev for an in-depth exploration of the 2026 ADA Standards! This is our most popular course of the year, offering the perfect opportunity to immerse yourself in the essential content featured in this comprehensive 300-page clinical guidebook.
This course, updated annually, is an essential review for anyone in the field of diabetes. Join Coach Beverly as she summarizes the annual updates to the American Diabetes Association’s (ADA) Standard of Medical Care in Diabetes. This course provides critical teaching points and content for healthcare professionals involved in diabetes care and education.
Topics:
Course Objectives:
Upon completion of this activity, participants will be able to:
For last week’s practice question, we quizzed participants on RT forgetting their insulin, and what would be the best response. 63.10% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it below: Answer Question

RT has type two diabetes and has been maintaining a time and range of 70% or greater. However, when they show up at the office, the last week’s time in range dropped to 30%. You ask what was different this week from the previous few months. RT tells you they went on a five day fishing trip and forgot their insulin.
What’s the best response?
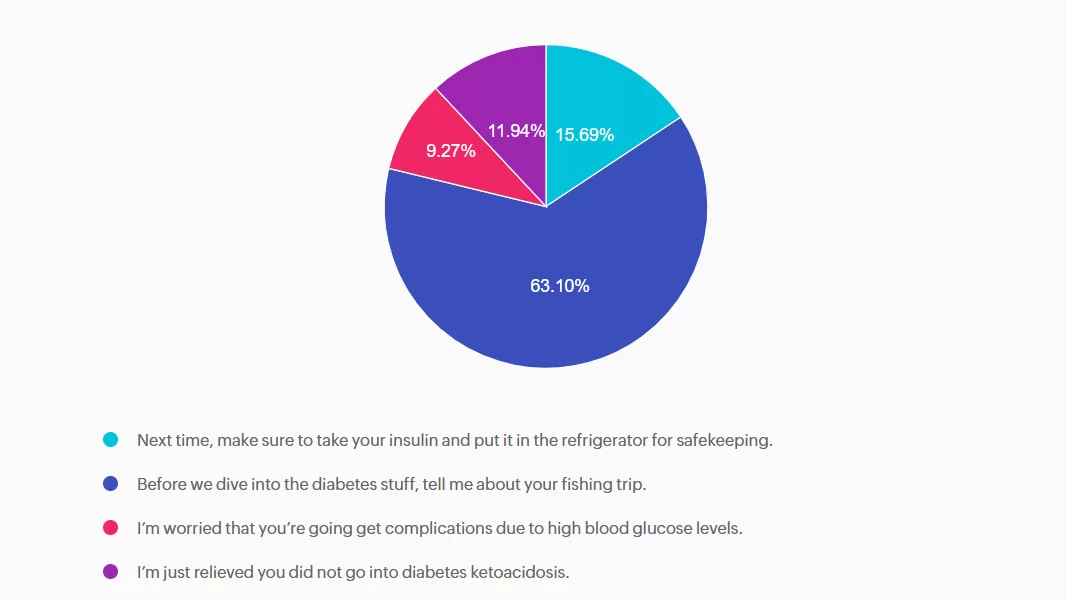
Answer A is incorrect: 15.69% chose this answer, “Next time, make sure to take your insulin and put it in the refrigerator for safekeeping.” This approach goes under the compliance model, where the healthcare professional only provides one way instruction without considering the individuals insights and problem solving skills. We want to work toward a person-centered collaborative approach to foster connection.
Answer B is correct: 63.10% chose this answer, “Before we dive into the diabetes stuff, tell me about your fishing trip.” Great job! This is the best answer. By asking RT about their fishing trip first, you let them know you are interested in their life experiences and this helps to establish a connection. After hearing about the trip, we might pivot and say something like, “Do you want to discuss strategies to bring your insulin on your next fishing trip?”
Answer C is incorrect: 9.27% chose this answer, “I’m worried that you’re going get complications due to high blood glucose levels.” Although this statement shows concern, it is unlikely that RT will get diabetes complications from not taking their insulin for a few days. This statement could lead to feelings of shame and failure, and may close the door to making a meaningful connection.
Answer D is incorrect: 11.94% chose this answer, “I’m just relieved you did not go into diabetes ketoacidosis.” This statement could evoke feelings of guilt and shame, that could close the door to future communication. And if RT has type 2 diabetes, the chance of DKA is minimal. Instead of focusing on the HCP feelings, let’s check in with RT and explore problem solving strategies for future trips that would work for them.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!
For last week’s practice question, we quizzed participants on Diabetes Tech and Diabetes Distress. 99.36% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it below: Answer Question

Kyle is a 55-year-old man with type 2 diabetes for ten years. He was recently diagnosed with retinopathy in both eyes. His grandmother lost her eyesight due to diabetes. Due to this family history, he is very concerned about his new diagnosis. He uses a Libre continuous glucose monitor (CGM) to monitor his blood sugar levels. During your visit, he is preoccupied with checking his Libre CGM and tells you that he uses his glucometer to verify CGM readings at least four to six times per day. When you ask him about this, he reports that he can’t focus on his work or home life if he isn’t over 90% time in range.
As a diabetes care and education specialist, what is the best approach to this situation?
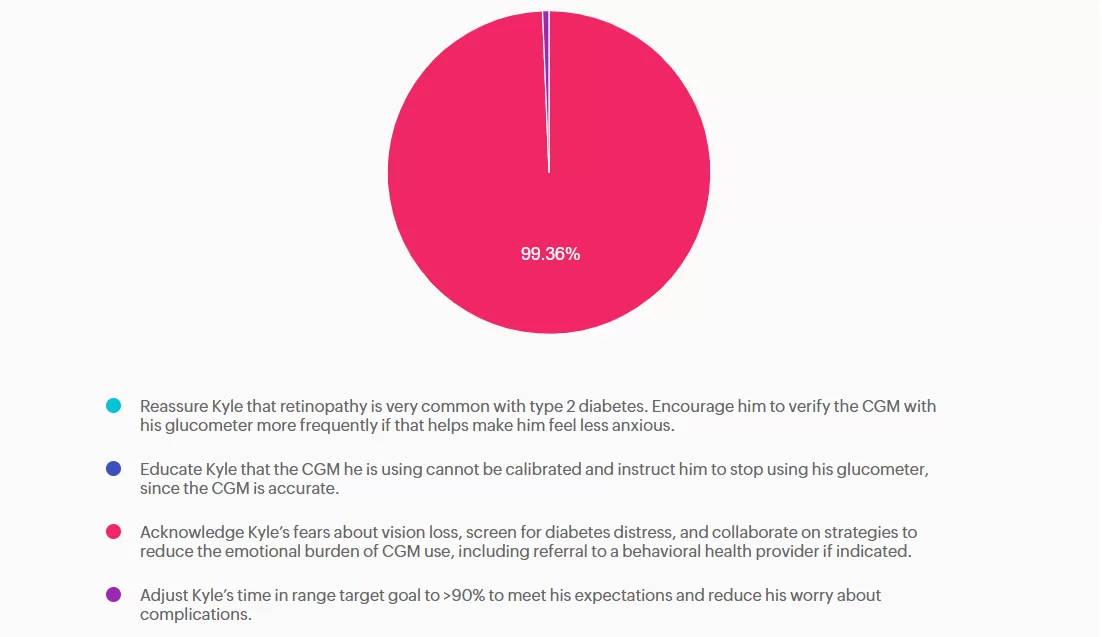
Answer A is incorrect: 0% chose this answer, “Reassure Kyle that retinopathy is very common with type 2 diabetes. Encourage him to verify the CGM with his glucometer more frequently if that helps make him feel less anxious.” This is incorrect. Although diabetes retinopathy is a common complication of diabetes, it is not inevitable, and the risk can be reduced by maintaining optimal glycemic control. Additionally, verifying blood glucose levels with a glucometer when there appears to be no issue with his CGM will not alleviate his anxiety.
Answer B is incorrect: 0% chose this answer, “Educate Kyle that the CGM he is using cannot be calibrated and instruct him to stop using his glucometer, since the CGM is accurate.” This is incorrect. Though his particular CGM cannot be calibrated, fingerstick blood glucose readings are the gold standard when CGM readings are unexpectedly out of range.
Answer C is correct: 99.36% chose this answer, “Acknowledge Kyle’s fears about vision loss, screen for diabetes distress, and collaborate on strategies to reduce the emotional burden of CGM use, including referral to a behavioral health provider if indicated.” This is correct. Kyle is demonstrating symptoms of diabetes distress due to fear of ocular complications, perfectionism, and technology overwhelm. The ADA Standards of Care 2025 recommend routine screening for diabetes distress and other psychosocial concerns at least annually or when complications arise.
Answer D is incorrect: 0.64% chose this answer, “Adjust Kyle’s time in range target goal to >90% to meet his expectations and reduce his worry about complications.” This is incorrect: The time in range goal for most adults living with diabetes is >70%. Adjusting his time-in-range goal to >90% will not work to reduce his obsessive behavior.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!
Get 30% Off Your Entire Order!
From November 30th to December 2nd, use the code “Cyber30″ for 30% off at checkout!
Save the date and shop our sale
For last week’s practice question, we quizzed participants on FIB-4 of 2.83. 48.09% of respondents chose the best answer. We want to clarify and share this important information, so you can pass it on to people living with diabetes and your colleagues, plus prepare for exam success!
Before we start though, if you don’t want any spoilers and haven’t tried the question yet, you can answer it below: Answer Question

AR lives with type 2 diabetes, and their waistline is 41 inches. Since their ALT and AST levels are elevated, you know they are at risk for steatosis (MASH). You quickly calculate their Fibrosis-4 Index (FIB-4), by plugging in AR’s Age, AST, ALT, platelet count into the FIB-4 calculator. AR’s result is 2.83.
According to the ADA Standards, with a FIB-4 value of 2.83, which action is required?
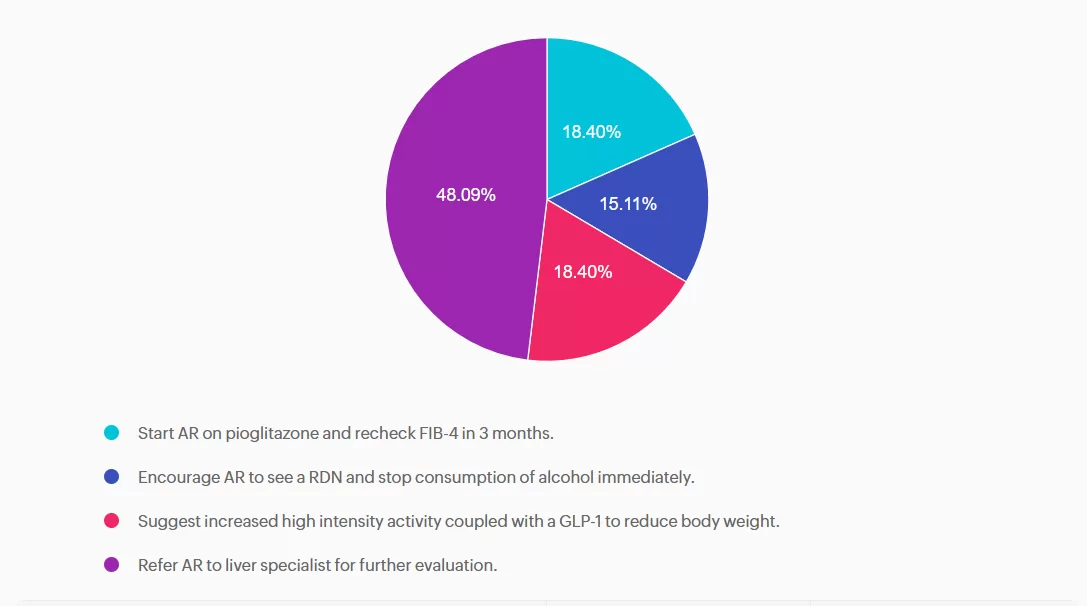
Answer A is incorrect: 18.4% chose this answer, “Start AR on pioglitazone and recheck FIB-4 in 3 months.” Although pioglitazone is a recommended treatment for steatosis, since AR’s FIB- is greater than 2.67, this indicates AR is at high risk for advanced fibrosis and a referral to a liver specialist is warranted.
Answer B is incorrect: 15.11% chose this answer, “Encourage AR to see a RDN and stop consumption of alcohol immediately.” Seeing a RDN is very important for AR to evaluate and customize an eating plan to address their steatosis and support quality of life. However, since AR’s FIB- is greater than 2.67, this indicates AR is at high risk for advanced fibrosis and a referral to a liver specialist is warranted.
Answer C is incorrect: 18.4% chose this answer, “Suggest increased high intensity activity coupled with a GLP-1 to reduce body weight.” Strength training and activity, coupled with a GLP-1 for GLP-1/GIP are important strategies to address steatosis. However, since AR’s FIB- is greater than 2.67, this indicates AR is at high risk for advanced fibrosis and a referral to a liver specialist is warranted.
Answer D is correct: 48.09% chose this answer, “Refer AR to liver specialist for further evaluation.” Great job! AR will require intensive intervention to decrease their risk of worsening steatosis, including MNT, targeted activities, and a referral to a liver specialist to determine the best treatment approach.
We hope you appreciate this week’s rationale! Thank you so much for taking the time to answer our Question of the Week and participate in this fun learning activity!